Serendipity or Fate? Gift Honors Retired Transplant Surgeon

Harry Ward is a practical man who understands probabilities. (If you’ve ever torn through the powder on a snowmobile, you have the retired engineer, and his work on rotary engines, to thank.) Though he’d added his name to the national transplant wait list, he knew the likelihood of receiving a kidney at his age was slim.
“If you have a kidney,” Ward reasoned, “why would you give it to somebody who’s 70 when you could give it to somebody who’s 40 who’s going to live a lot longer?”
But fate has a way of upending our most rational expectations.
The phone rang. It was a young man, the son of a couple Ward and his late wife, Carrie, knew well. Ward hadn’t seen him in years.
“I understand you need a kidney,” he said.
But Ward, who lives in Toledo, couldn’t get anyone to schedule the surgery. His nephrologist – a kidney disease specialist – was baffled by the delay and tried to learn the cause. “We had a person who needed a kidney and we had somebody willing to donate,” says Ward, “and he never got an answer.”
Time was running out. His doctor had an idea: “Let’s call Cleveland Clinic.”
A Good Surgeon and a Good Doctor
Ward’s surgery wasn’t a simple one. Although his donor was healthy, he had been treated for testicular cancer some 10 years earlier. As a general rule, cancer survivors are not eligible to be living donors, but transplant teams can review each case to determine if organs have been damaged by chemotherapy or other treatments.
Stuart M. Flechner, MD, a professor of surgery in the Kidney Transplant Program at Cleveland Clinic Glickman Urological & Kidney Institute, discovered that portions of the donor’s ureter, the tube that connects the kidney to the bladder, had been weakened by radiation therapy. With that knowledge, Dr. Flechner connected Ward’s own ureter to the new kidney. The procedure, called a ureteropyelostomy, is designed to avoid post-operative complications such as bleeding that would require a second, reparative surgery.
In the years that followed, Ward continued to visit his surgeon. “Dr. Flechner was a very easy person to talk to,” says Ward.
The urologist never looked at his watch. Or hustled Ward out the door. Or handed him off to another doctor. Often, Ward, who had to drive two and-a-half hours from Toledo to Cleveland to make it to his appointments, was Flechner’s last patient of the day.
“He was a very good surgeon: but Cleveland Clinic has many very good surgeons,” Ward explains. “He was a very good, helpful doctor, but Cleveland Clinic also has lots of these. But it is rare to find the combination in one person. Dr. Flechner would spend as much time with me as required, even when he knew I came loaded with questions and charts.”
It’s one thing to save a man’s life – to care for his ailing body. It’s another to care about the man himself.
A nurse suggested Ward might want to start seeing a nephrologist for his long-term kidney health instead of his surgeon. But Dr. Flechner, says Ward, was having none of it. “He said, ‘absolutely not. You’re not moving him,” remembers Ward, laughing. ‘I’m continuing to work with him.’ And he did – up until he retired.”
For Ward, loyalty matters; it’s a quality he admires.
“Dr. Flechner, he stuck with me.”
The Patient Comes First
Today, a dozen years later, Ward, who turned 82 in September, takes immunosuppressive drugs to ensure that his body doesn’t attack his life-giving kidney. But those drugs leave him especially vulnerable to infections such as COVID-19, so during the pandemic, he’s had to stay away from most folks. “I tell my friends, now I know what it’s like when the judge puts you on house arrest,” he says. He’s been hunkering down with Norman, the Wire Fox Terrier he rescued from a shelter, who, he readily admits, rescued him right back, offering companionship and a respite from lock down with frequent walks through the neighborhood.
This spring, he signed on the dotted line to establish the “Harry Ward Renal Transplantation Fund, honoring Stuart M. Flechner, MD,” an endowed fellowship of $1.5 million to benefit the Urological & Kidney Institute, payable upon Ward’s death.
When it was suggested to him that he might want to rethink the name – most such gifts don’t use the word “honoring” in the title – Ward was having none of it.
“Nobody knows or cares who Harry Ward is,” he says “But I want recipients of this grant to ask, ‘who is Dr. Flechner, and why is he being honored in this way?
Ward hopes that question will lead some of them to do the research to find out – and aspire to become better doctors by emulating Dr. Flechner. The physician has not been idle since his retirement in 2018. Dr. Flechner is a Professor Emeritus of Surgery and Urology at Cleveland Clinic Lerner College of Medicine. He is active in research and as an editor for the American Journal of Transplantation, Clinical Transplantation and Transplantation International. He is also a member of the medical board of the National Kidney Registry, the largest paired kidney exchange network in the world.
“He cared about his patients and he paid attention to his patients,” says Ward. “The patient seemed to really come first, no matter at what stage of the process.”
It’s fitting that Dr. Flechner’s patient-centric approach was first articulated 100 years ago by a visionary who shared his specialty – urologist William Lower. One of Cleveland Clinic’s four founders, Lower famously declared: “A patient is the most important person in the institution... it is our job to satisfy them.”
A History of Fostering Surgical Innovation
The Urological & Kidney Institute, where Dr. Flechner spent much of his career, is unique in that it merges its urology program (the study of diseases of the male and female urinary tract and male reproductive organs) with its nephrology program (the branch of medicine that deals with chronic kidney disease, kidney infections and kidney failure).
This consolidation of disciplines, explained its Chairman, Eric Klein, MD, encourages specialists to work together, offering grateful patients like Ward better treatments and fostering pioneering research that advances the field of urology.
“The main overlap between those two programs is our transplant program,” says Dr. Klein. “We are one of the very few urology departments in the country – and around the world – that actually do kidney transplants.” To date, surgeons at Cleveland Clinic have done 5,633 kidney transplants since the first such operation was performed in 1963. Before transplantation, the only treatment for kidney failure was dialysis, Klein explains, “a procedure actually invented here at the Cleveland Clinic by one of our nephrologists.”
That dedication to medical and surgical innovation continues today. In 2019, “we were the very first transplant program to do a single port robotic kidney transplant,” says Klein. The minimally invasive, groundbreaking technique enables all surgical instruments and the donor kidney to be placed through one small abdominal incision. Patients experience less post-operative pain and, as a result, have no need for opioids after surgery.
Ward’s gift, says Klein, will help the Urological & Kidney Institute continue to do cutting-edge work and train the next generation of transplant nephrologists and urologists.
Because Harry Ward is a practical man, after all.
“I want to support residents because residents at Cleveland Clinic turn into doctors,” says Ward. “And if we can make better doctors, everybody benefits from that.”
Florida Couple Helps Children at the Pediatric Rehab Center Reach their Full Potential
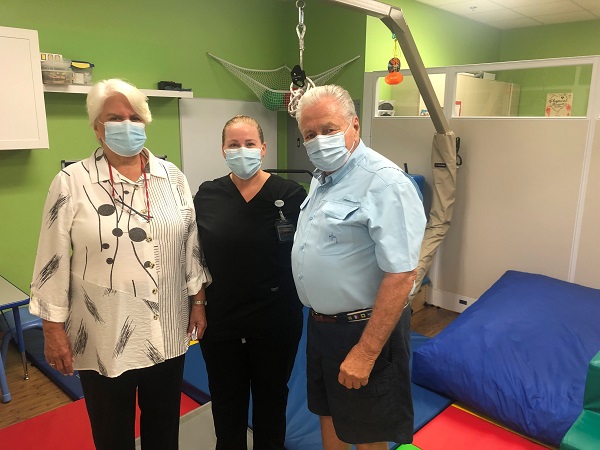
Bright colors of red, yellow, and blue surround the Pediatric Rehabilitation Center at Cleveland Clinic Martin Health Hospital. Although the environment may resemble a playground, it’s not all fun and games for the young patients who receive life-changing therapy there. Wayne and Bonnie Barski donate annually to the rehab center to ensure these children have the best opportunity to reach their full potential.
Located in Jensen Beach, Florida, the Pediatric Rehabilitation Center at Cleveland Clinic Martin Health Hospital provides advanced care to children from infancy to adolescence in need of physical, occupational and speech therapy. Specially-trained therapists utilize an assortment of swings, tricycles and technology devices to engage children and ensure they achieve optimal growth and development.
Treating conditions ranging from cerebral palsy, genetic disorders, orthopaedic and neurological conditions, speech disorders and more, the therapy team provides an array of pediatric screenings, communication assessments and specialized treatments. Over the years, generous supporters have enabled the rehab center to reach more children in need of innovative therapy by helping expand services, upgrade equipment and increase capacity.
Giving Back to Help Make Lives Easier
Wayne and Bonnie do not have children of their own and are passionate about supporting pediatrics. In June, they signed a five-year pledge to fund the rehab center’s initiatives and toured the facilities to see the impact of their gifts thus far. “We want to help those children that enter this world with an uphill battle,” says Wayne.
The couple’s first donation was combined with another donor’s gift to create an intimate Occupational Therapy (OT) space for the center’s youngest patients. Their gift was used to purchase items such as a swing system for one of the OT rooms, stairs and replacement equipment for the physical therapy gym, a low tech communication device, key guards for iPads used with a speech generating application and several toys to be used in OT and speech therapy.
“The Barski donation has been, and will continue to be a huge blessing to this department," says Lynsey Heinold-Edge, MA, CCC-SLP, pediatric therapy lead therapist. “We have already been able to build a treatment room for an occupational therapist, so that she can have a true space instead of working in a confined area. The patients and families she treats are so delighted to have that space. We have also been able to update equipment and assessments, and get new and exciting therapy activities to use with our patients. Knowing we have this funding available, allows us to plan for the future and continue to provide exemplary care.”
How you can help
Your gift to the Pediatric Rehabilitation Center at Cleveland Clinic Martin Health Hospital helps young patients overcome challenges and provides them with the best possible start in life. Please make a gift today.
$12M NIH Grant to Support Team Science into the Biology of Cardiovascular Disease

Cleveland Clinic has received a new five-year, $12 million grant from the National Heart, Lung, and Blood Institute (part of the National Institutes of Health) to investigate the molecular and cellular mechanisms underlying cardiovascular and inflammatory diseases. The grant will focus specifically on defining how a class of receptors called integrins contribute to disease development and progression.
“The long-term goal of our research will be to gain important insights for developing new therapies to treat or prevent blood, cardiovascular and inflammatory diseases,” says Edward Plow, PhD, staff in the Department of Cardiovascular & Metabolic Sciences, and the grant’s program director.
The large collaborative grant will support three related research projects led by Dr. Plow; Jun Qin, PhD, Department of Cardiovascular & Metabolic Sciences; and Daniel Simon, MD, University Hospitals and Case Western Reserve University. All three respective projects will focus on defining the role of integrins, which play an important role in cell adhesion and migration—both of which are critical for an array of physiological processes ranging from blood clotting to host immune defense.
Three Complementary Studies of Integrins
Dr. Plow’s project focuses specifically on a protein named kindlin-2. Previous research has shown that kindlin-2 plays an important role in activating—or “turning on”—integrins. Kindlin-2 has been suggested to bind with dozens of other proteins at multiple different sites, as well, so Dr. Plow plans to study the structure and function of kindlin-2 in various types of blood vessel cells. His team will also use preclinical models to understand how the presence or absence of kindlin-2 in blood vessel cells affects disease-predisposing processes like angiogenesis, vascular permeability and would healing.
In complementary projects, Dr. Qin, who holds the Bonnie and Eunice Collins Endowed Chair for Innovative Diabetes Research at Cleveland Clinic, will study another protein implicated in integrin activation named talin. Dr. Simon will study an integrin on white blood cells named Mac-1, investigating its potential involvement in inflammation and thrombosis.
“Although we will primarily be studying the structure and function of these small molecules, our findings stand to have a big impact on our understanding of pathologies that underlie many different diseases,” says Dr. Plow.
This article first appeared in Lerner Research Institute News.

