Tachycardia is an abnormal heart rhythm with a fast heart rate of more than 100 beats per minute at rest. It can start in the upper or lower chambers of your heart and can range from mild to life-threatening. Treatments include medicines, an ablation procedure and implantable cardioverter defibrillator (ICD) placement.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
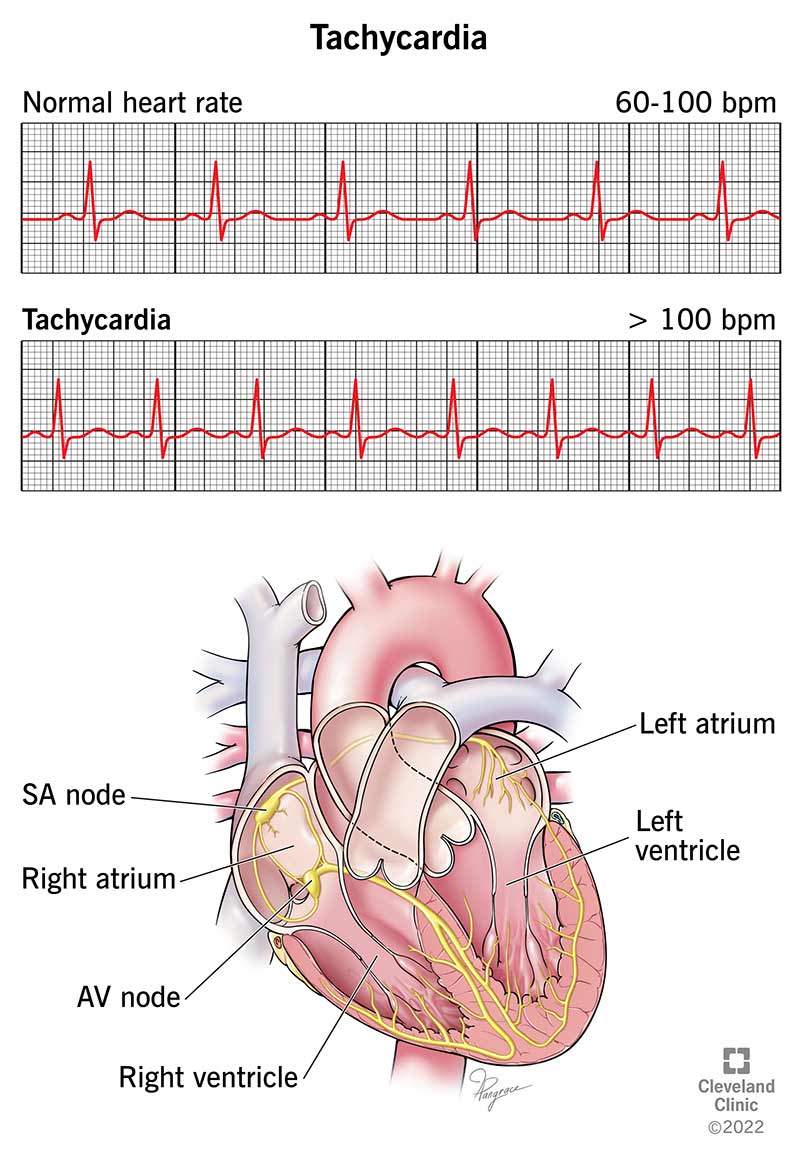
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22108-tachycardia-illustration)
Tachycardia (ta-kih-kar-dee-uh) is a kind of abnormal heart rhythm (arrhythmia). With tachycardia, your heart beats more than 100 times a minute at rest. Your heart beats faster than normal for a few seconds to a few hours. Normally, your heart rate is 60 to 100 beats per minute when you’re not active.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Because your heart beats too often, it doesn’t have the time it needs to fill with blood between beats. This can be dangerous if your heart can’t supply all your cells with the blood and oxygen they need.
Some kinds of tachycardia can come back regularly and can be more serious. Tachycardias can be mild, while others cause issues that are moderately harmful. A healthcare provider can tell you which type of tachycardia you have and how to manage your condition.
Tachycardia can happen in any of your heart’s four chambers. It occurs when you have an issue with electrical signals there.
Types of tachycardia include:
Some people with tachycardia don’t have symptoms, while others may have mild to severe symptoms. Tachycardia symptoms may include:
Your heart normally responds to electrical signals from your heart’s sinoatrial (SA) node. These signals control how often your heart beats. When you’ve had a scare or are very emotional or anxious, or are exercising, your heart may send signals more frequently for a short time. This is called sinus tachycardia and goes away when you calm down or rest.
Advertisement
You may also have a fast heart rate from substance or tobacco use or from too much caffeine or alcohol.
Tachycardia causes include:
Risk factors for tachycardia include:
Without treatment, certain types of tachycardia can cause your kidneys, liver or heart to fail. Tachycardia also can lead to:
Your healthcare provider will ask for your medical history and do a physical exam. They may also order tests like:
Procedures and medications are the main kinds of treatment for tachycardia. Treatments vary depending on the type of tachycardia and what’s causing it. Treatments may include:
Medications providers prescribe may include:
In some situations, you may need CPR.
Your experience will depend on which type of tachycardia you have. You may have harmless symptoms, life-threatening symptoms (from ventricular tachycardia or fibrillation) or something in between. Medicines and other treatments can help you manage your high heart rate.
You may need to wear a Holter monitor or do electrophysiology testing to see how well your medicine is working.
If you have sinus tachycardia, your symptoms will go away once the fear, anxiety or other emotion that caused it ends. For most other types of tachycardia, you’ll need medication or even a procedure to keep your fast heart rate and other symptoms from coming back.
Tachycardia that puts you in danger doesn’t go away on its own. You’ll need to live a healthy lifestyle and take medicines to manage your condition. You may also need to have a procedure, like an ablation.
Although medications can’t cure tachycardia, they can help you regulate it. Ablation may be a long-term solution to certain types of tachycardia. It may even cure them.
Advertisement
You may be able to calm down your tachycardia if your provider teaches you vagal maneuvers.
You can care for yourself in the following ways:
After you get a tachycardia diagnosis, you can expect to have follow-up appointments with your provider. But you should contact them if your medicine isn’t helping you or if you start having new symptoms.
Get medical help right away if you:
You should also get help right away for someone who collapses or is unconscious from ventricular fibrillation. They’ll need CPR to survive until paramedics arrive.
Questions to ask your provider may include:
Feeling your heart race can make you stop what you’re doing and wonder what’s going on. Tachycardia symptoms can range from mild to severe, depending on which type of tachycardia you have. For peace of mind, talk to your healthcare provider if you’re having symptoms. They can tell you if you have a reason to be concerned.
Advertisement
Keep taking the medicines your provider prescribed for you, especially heart medicines. Don’t stop taking them without your provider’s approval. And be sure to keep going to all your follow-up appointments.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
