Cardiac arrest happens because of an electrical issue that makes your heart stop beating. When your heart stops pumping blood, you become unconscious. Cardiac arrest can be fatal in minutes. This is why bystanders should call for help and start CPR immediately. A person’s chances of survival are best when they get help right away.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
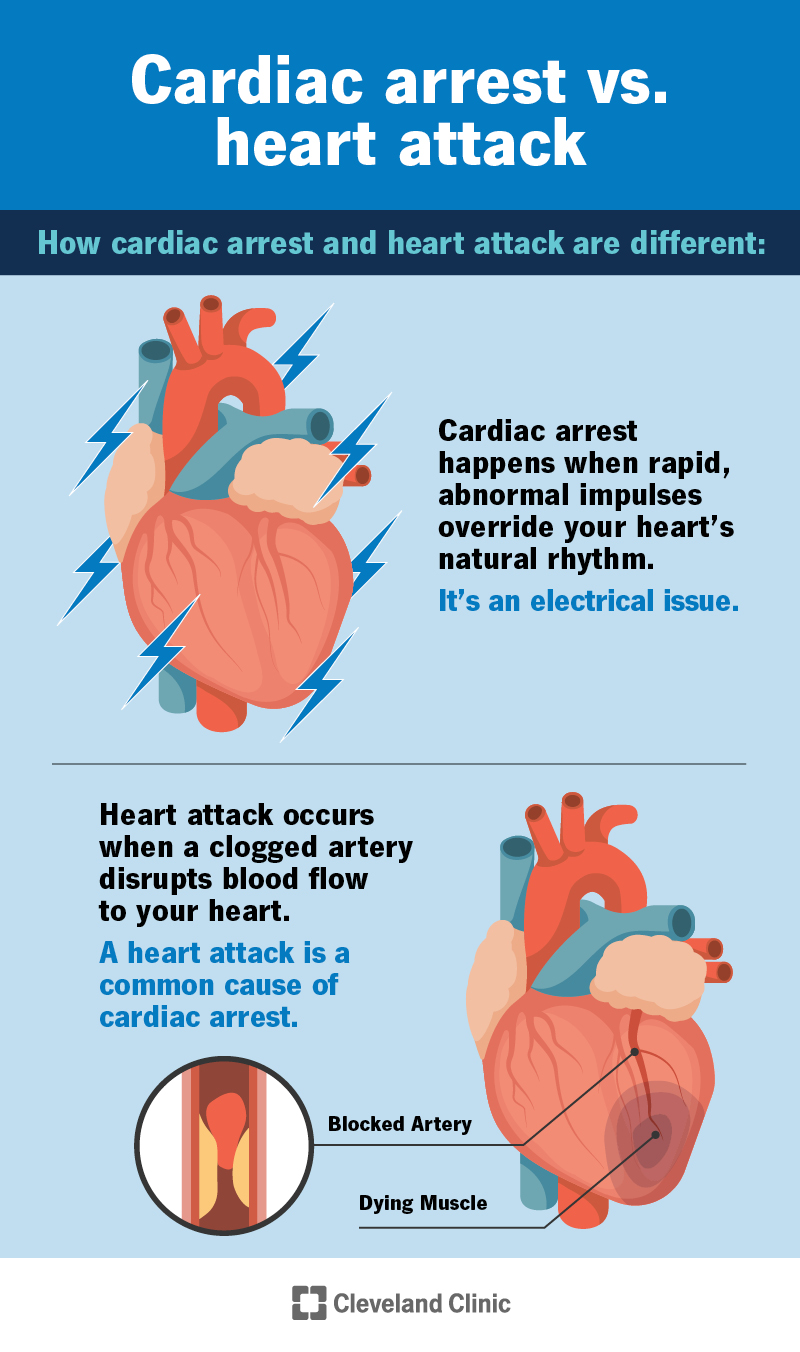
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21736-cardiac-arrest-vs-heart-attack)
Cardiac arrest happens when your heart stops beating or beats so fast that it stops pumping blood. When your heart isn’t pumping blood, this puts your organs and whole body at risk of death within minutes because they need a constant supply of oxygen. Your blood delivers that oxygen.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
With this condition, people typically collapse and can’t respond. Symptoms start without warning. This is why people also call this life-threatening condition sudden cardiac arrest.
Cardiac arrest (an electrical failure) isn’t the same as a heart attack. A heart attack happens when a blocked artery cuts off blood flow to heart muscle.
With cardiac arrest, your heart stops beating, but a rescue is still possible. With immediate treatment, you can survive. If someone doesn’t save you, it leads to sudden cardiac death.
Emergency treatment includes cardiopulmonary resuscitation (CPR) and defibrillation. CPR keeps oxygen flowing to your brain until an electric shock restores a normal heart rhythm. CPR and defibrillation (which delivers an electrical shock) may save your life.
About 350,000 Americans each year experience cardiac arrest outside of a hospital. It typically affects adults, but it can happen in children and teens, too.
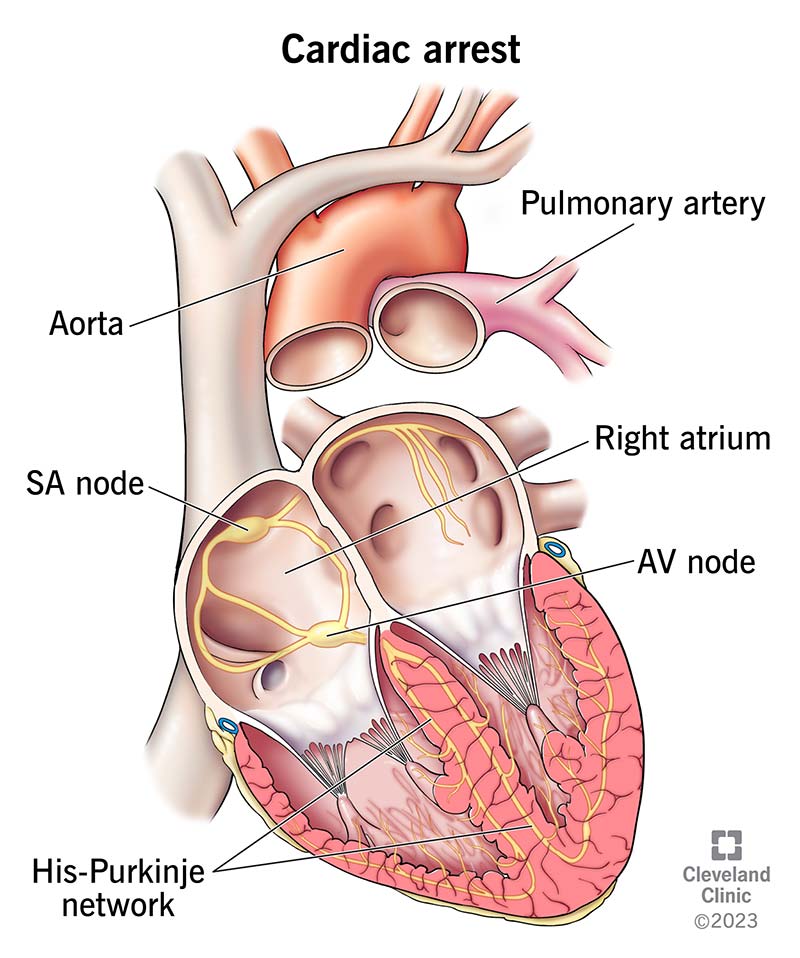
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21736-cardiac-arrest-illustration)
Some people collapse without any other symptoms or warning signs. Right before you faint and have other signs of cardiac arrest, like lack of a pulse or breaths, you may have symptoms like:
Advertisement
Any condition that severely lowers oxygen levels, disrupts your heart’s electrical signals or keeps your heart from pumping well can lead to cardiac arrest. Abnormal heart rhythms (arrhythmias) cause most sudden cardiac arrests. Abnormal, rapid impulses abruptly override the normal electrical impulses that start your heartbeat.
In many cases, a chaotic rhythm, ventricular fibrillation (v-fib), takes over. When this happens, your heart quivers instead of pumping and blood flow stops. Without rapid treatment, you can die within minutes.
Other causes of cardiac arrest include:
Sudden cardiac arrest happens in people with and without heart disease. A family history of cardiac arrest, sudden death or fainting from unexplained causes can raise your risk. Having a heart attack or another heart condition can significantly increase your risk, too. Conditions that can increase the risk of sudden cardiac arrest include:
Cardiac arrest symptoms begin suddenly, leaving little time for tests. The condition can become fatal within minutes. This is why quick action is essential.
Someone in cardiac arrest is usually unconscious, has no pulse, doesn’t respond and isn’t breathing. These signs are enough to make a diagnosis.
A first responder who does an electrocardiogram (EKG) will find an abnormal rhythm or no heartbeat. After a person is revived and stable, healthcare providers often find the cause of cardiac arrest by using:
CPR plus defibrillation rescues a person from sudden cardiac arrest.
To treat cardiac arrest, first responders will:
Advertisement
Cardiac arrest treatment has to start right away, wherever you are. Brain injury can happen after just five minutes without oxygen. Survival drops sharply after eight to 10 minutes without CPR. Starting CPR in the first few minutes is the most important factor for survival.
The biggest difference in survival comes from what happens before first responders arrive. Early action by bystanders is the strongest predictor of better outcomes. If you see someone suddenly collapse and you suspect sudden cardiac arrest, do this:
Surviving cardiac arrest is a major medical event. What happens next depends mostly on how quickly you get treatment. People who get immediate help have the best chance of returning to their normal lives. Recovery takes time. Steady improvement is common.
After returning home, you may have medical problems related to the arrest or its cause.
These may include:
Advertisement
You may need to go back to the hospital for treatments, depending on how your organs and brain recover. Severe cases may lead to a coma or long-term unconscious state. People often need rehabilitation to relearn how to walk or dress. This can take weeks to months.
Be patient with yourself as you slowly get back to doing the things you did every day. Many people improve steadily during the first six months.
You’ll most likely have follow-up appointments with multiple healthcare providers as you recover from sudden cardiac arrest. You’ll also have procedures or treatments that can help prevent you from having another cardiac arrest.
Be sure to tell your provider if you’re having any new symptoms or aren’t feeling better during the expected time frame.
Questions to ask your provider may include:
Yes, you can survive cardiac arrest. But it’s not common. Most people who have sudden cardiac arrest outside of a hospital don’t survive. This is usually because they don’t get help in time.
Still, survival rates are better than they used to be. About 1 in 10 people who have cardiac arrest outside a hospital and get emergency treatment survive and go home from the hospital. About 1 in 4 people who have cardiac arrest inside a hospital survive and go home.
Advertisement
Yes, it’s possible to lower your risk of cardiac arrest. You can do this by managing conditions that strain or damage your heart (like high cholesterol, high blood pressure and diabetes) and living a healthy lifestyle. This includes:
If abnormal heart rhythms run in your family, you may want to talk with a genetic counselor. They can tell you who might be at risk or need a blood test to check for an issue that causes arrhythmia.
Checking for coronary artery disease or heart rhythm problems can let you know whether you’re at risk for sudden cardiac arrest.
To prevent future episodes of sudden cardiac arrest, your healthcare provider will suggest tests to figure out why it happened. Tests may include:
Treatments that can prevent cardiac arrest or lower your risk of a second episode include:
Recovery from cardiac arrest takes time and includes therapies to help make the most of your abilities. Many survivors need ongoing heart care to prevent another episode.
Be sure to go to all your follow-up visits and keep taking any prescribed medicines. It may give you peace of mind if people who live with you take a CPR class in case of another cardiac arrest. Most cardiac arrests outside a hospital happen at home.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
