A tilt table test is a procedure where you lie flat on a table that quickly moves you to an upright position. It can help find the cause of fainting episodes due to nervous system problems, like vasovagal syncope, postural orthostatic tachycardia syndrome (POTS) and orthostatic hypotension. The test happens in a safe, controlled environment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
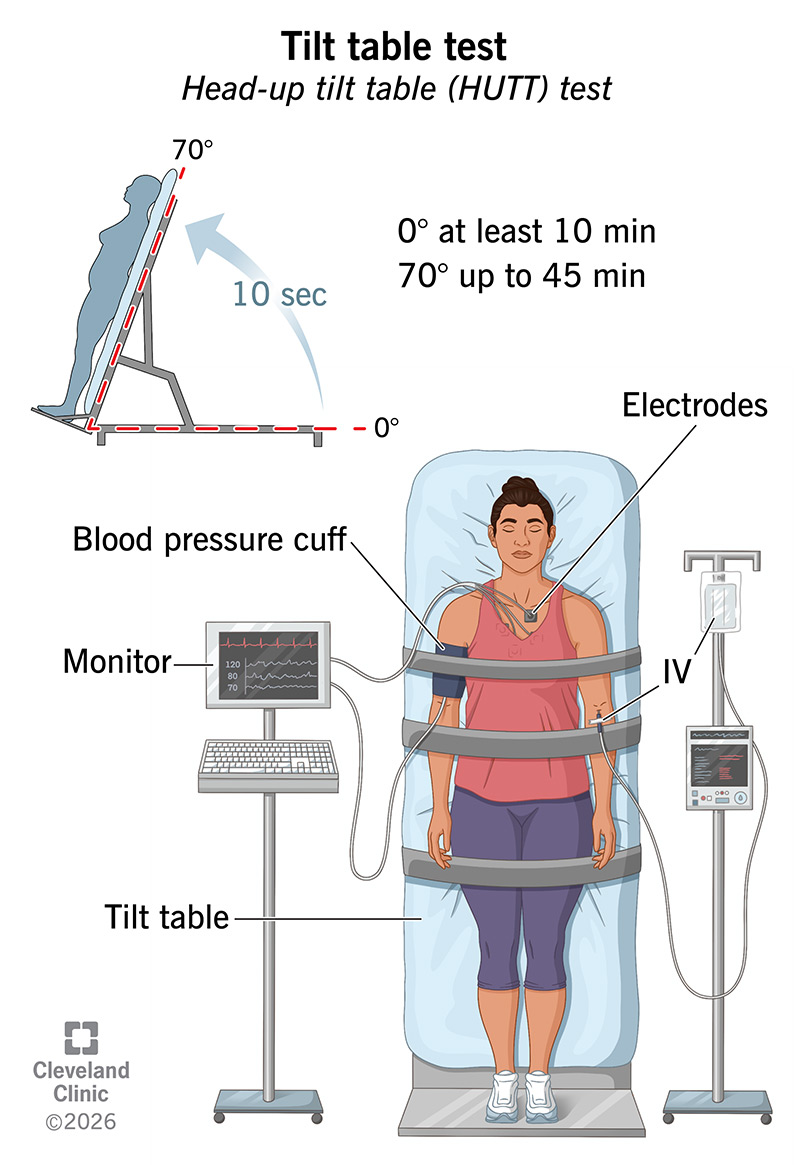
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17043-tilt-table-test-illustration)
A tilt table test, also called head-up tilt table (HUTT) testing, is a procedure that healthcare providers use to understand why you have fainting episodes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In this test, you’re securely fastened to a padded table that providers quickly move from a flat to a vertical position. This mimics the act of standing up. Devices monitor your blood pressure, heart rate and heart rhythm to see how your body reacts. This is among the most detailed ways to study the cause of fainting.
Your provider may suggest this test if you’ve fainted multiple times without a clear reason. Before doing a tilt table test, providers rule out any heart-related causes, like arrhythmias or problems with your heart’s structure. HUTT may help diagnose or manage:
Rarely, people faint during tilt table testing. But providers are right there with you. So, they can put the table back down so you can recover quickly. You may also feel tired and/or have an upset stomach. Some people release pee when they faint.
Advertisement
Tilt table testing may not be safe for you if you’re pregnant or have blockages in arteries that supply blood to your heart or brain. Your provider will review your medical history before doing this test to make sure it’s right for you.
Tilt table testing moves your body from a flat to an upright position. This forces the network of nerves that control automatic processes (autonomic nervous system) to maintain your blood pressure. Normally, it can do that just fine.
But certain medical conditions, like vasovagal syncope and POTS, disrupt those normal processes. That’s why you might faint — or come close to fainting — when you stand up after lying down.
This test lets your healthcare provider see how your blood pressure and heart rate change when you shift body positions. You’re connected to monitors that track your vital signs the whole time. This gives valuable data to your provider. The test can help diagnose or rule out conditions that cause fainting. This lets you get the treatment you need.
The healthcare provider who ordered the test will tell you how to prepare. They may ask you to avoid caffeine and alcohol for 12 hours prior to the test. You may also need to fast (no food or drinks except water) for at least two hours before the test. It’s generally considered unsafe to drive yourself home after tilt table testing. So, be sure to arrange for someone to drive you to and from your appointment.
Tilt table testing happens in a safe, controlled environment. Your healthcare provider will:
Your provider will stop the test if you develop symptoms. You may faint. But try not to be scared or nervous about this happening. If you faint, providers will move the table back down right away so you can recover quickly.
Advertisement
In the past, tilt table testing sometimes involved two parts. The first part was tilting the table. Then, if symptoms didn’t appear, providers would give you medication to make your heart beat faster. This could sometimes trigger symptoms and help get more helpful information. Providers less commonly use medications these days but may still consider doing so in select cases.
After the test, your provider will lower the table to a flat position. You’ll stay on the table for five to 10 minutes as you lie flat. This lets them make sure you’re OK. They’ll measure your blood pressure, heart rate and heart rhythm.
It’s rare for severe symptoms to continue after the test. But if this happens, you may need care in the emergency department. Most people can go home after the test is done.
You can eat normally after the test unless you have other tests scheduled that require you to fast.
There are two types of results you can get from tilt table testing:
Advertisement
If you get a positive result, your healthcare provider will explain what this might mean for you. They’ll look at the data from the monitors along with your symptoms and medical history to reach a diagnosis.
Your provider may want to run the test again if they think the results aren’t right.
You may need more tests to figure out what’s causing you to faint. Your healthcare provider will explain next steps. Ask if anything’s unclear.
It’s also important to ask your provider about medications. Based on your tilt table test results, you may need to make changes to the types or amounts of medications you take. Follow the treatment plan your provider prescribes.
Call your provider with any questions about tilt table testing or how to prepare. They’ll help you feel comfortable about the process.
And be sure to tell your provider if you have new or changing symptoms at any point.
Fainting can make you feel afraid to be alone or go anywhere. Providers have been using the tilt table test for decades to get the information they need to find out what’s making people faint. Once they know the cause, they can make a treatment plan to help you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
