Brugada syndrome is a rare heart condition that can make your heart’s lower chambers (ventricles) beat in an abnormal rhythm. This can make you faint or have a cardiac arrest, putting you at risk of sudden cardiac death. Some people inherit this condition from a biological parent, but many others don’t know the cause.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
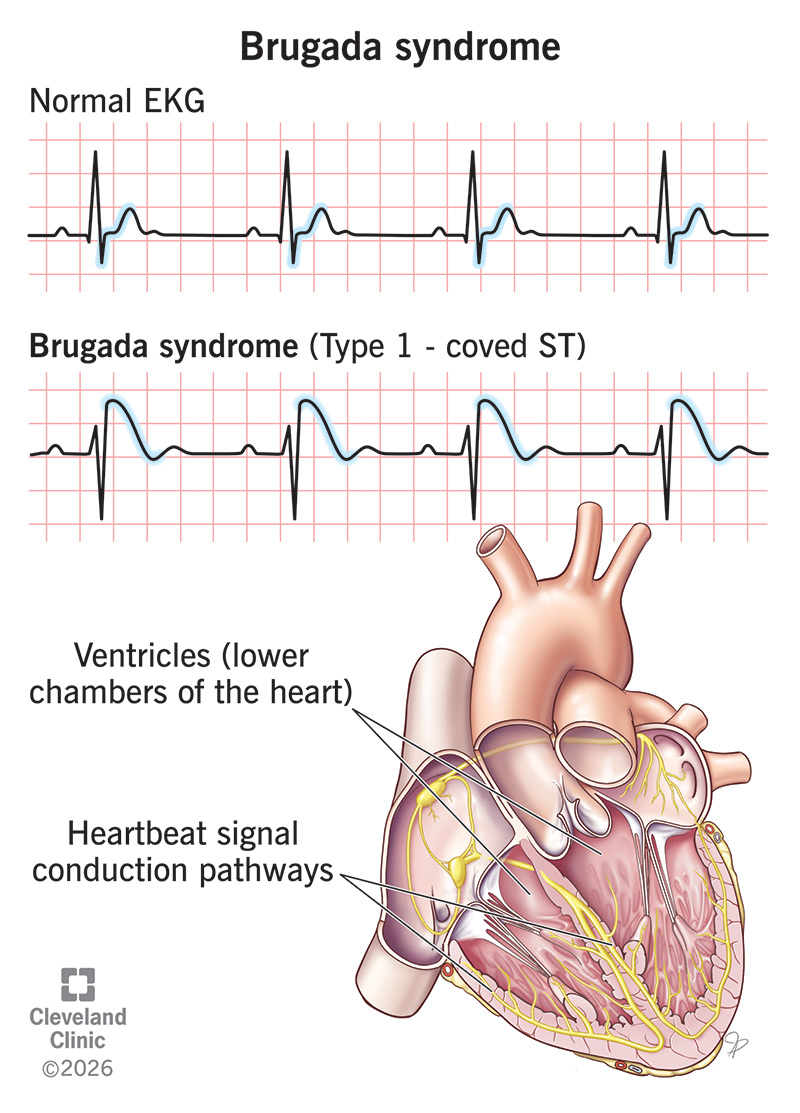
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/brugada-syndrome-illustration)
Brugada syndrome (BrS) is a genetic disease that can cause an abnormal rhythm in your heart’s lower chambers (ventricles). This irregular heart rhythm, ventricular fibrillation (v-fib), prevents your heart from pumping blood to your brain. When this happens, you faint.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
V-fib can lead to sudden cardiac death. This often happens while you’re at rest or asleep. Cardiac arrest may be the first symptom and the reason some people with this syndrome die in their sleep. To prevent cardiac arrest, healthcare providers put in an implantable cardioverter defibrillator (ICD).
You can inherit this rare syndrome from a biological parent. About 5 people in 10,000 around the world have Brugada syndrome.
Brugada syndrome type 1 has a specific electrocardiogram (EKG) pattern that a provider sees in your results.
Brugada syndrome types 2 and 3 have a less prominent version of this pattern and aren’t a definite diagnosis. You may need further testing in an electrophysiology lab.
Most people with BrS don’t have any symptoms. Brugada syndrome symptoms can happen at any age, but often start when you’re around 40 years old. Symptoms may include:
A genetic variation causes some cases of Brugada syndrome. But most people with this syndrome may not have a detectable genetic abnormality.
You may have a genetic variation in one of 18 or more genes, most often in SCN5A. These variations interfere with heartbeat signal conduction in your heart.
Advertisement
It only takes one copy of an affected gene from one parent to inherit BrS. Any child of someone with a Brugada-related gene variation has a 50% chance of having it, too.
Other biological family members may want to get a test for this variation. It’s important to schedule a screening for Brugada if you have a biological first-degree relative with Brugada syndrome. First-degree relatives are your parents, siblings and children.
A fever can trigger Brugada symptoms. This is why people with Brugada syndrome need to treat a fever right away — even if they have an ICD. You can take over-the-counter (OTC) medicines like acetaminophen to bring your fever down.
Other symptom triggers include:
Most people with a Brugada syndrome diagnosis are male. Other risk factors include:
Some people with Brugada syndrome develop abnormal heart rhythms in their upper heart chambers. Atrial fibrillation (AFib) is the most common one. Ventricular fibrillation (in your lower heart chambers) from this syndrome can lead to sudden cardiac death.
To make a Brugada syndrome diagnosis, a healthcare provider will perform a physical exam and review your medical history. They’ll also review your biological family history, especially a history of sudden cardiac death. Then, they’ll request tests.
Tests for diagnosing Brugada syndrome include:
Based on your EKG results, you may also have:
Advertisement
The goal of Brugada syndrome treatment is to keep you from having ventricular arrhythmias and treat them when they happen. If you have ventricular tachycardia, fainting spells or a cardiac arrest, you may need an implantable cardioverter defibrillator (ICD).
Even if you’re not having symptoms, your provider may decide you need an ICD because of your family history or test results. Some providers may do frequent follow-ups and only treat you when you have symptoms. Others don’t agree with this approach because your first symptom could be sudden cardiac death.
Besides an ICD, other treatments may include:
You should have an appointment with your provider at least once a year. If you have an ICD, your provider should check your device at least twice a year. Tell your provider about anything unusual.
You need immediate medical care if you’re in cardiac arrest. As you won’t be able to call for help yourself if this happens, someone near you will need to help. If you’re at risk of cardiac arrest, ask your family to get CPR training and call 911 or a local emergency number. You can also let coworkers know about your risk in case you need their help.
Advertisement
There’s no cure for Brugada syndrome. But treatments can lower your risk for sudden cardiac death, which is a complication of Brugada syndrome.
People with Brugada syndrome who have symptoms but aren’t receiving treatment have a high risk of sudden cardiac death. People without symptoms and with a normal EKG have a much lower risk.
Early diagnosis and treatment with an ICD can help you live longer. But an ICD can sometimes shock you when it shouldn’t. Also, part of the device can break or you can have an infection around it.
It’s not easy to hear that you have Brugada syndrome and the serious risks that come with it. But having a diagnosis allows you to take action to reduce those risks. Your healthcare provider can find the best treatment for you. It may give you peace of mind to have an automatic external defibrillator (AED) in your home and/or your child’s school. Also, it’s a good idea to ask people who live or work with you to learn CPR.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
