Post-traumatic stress disorder (PTSD) is a mental health condition that can develop after trauma. It may cause flashbacks, mood shifts, sleep issues or avoidance. A healthcare provider can help you get the support you need.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Post-traumatic stress disorder, or PTSD, is a mental health condition that can develop after you experience or witness a traumatic event. These could include war, natural disaster, abuse or sexual assault, among others.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You might have symptoms like having unwanted memories and flashbacks, negative mood changes, feeling on edge or being easily startled. These can last more than a month at a time and may affect your routine, relationships and school or work.
A healthcare provider can help you manage these symptoms.
This condition may show up in different ways. Providers recognize several subtypes based on age, timing or specific symptoms:
Advertisement
Knowing the type of PTSD you have helps your provider plan care. They’ll determine the type after reviewing your symptoms and health history.
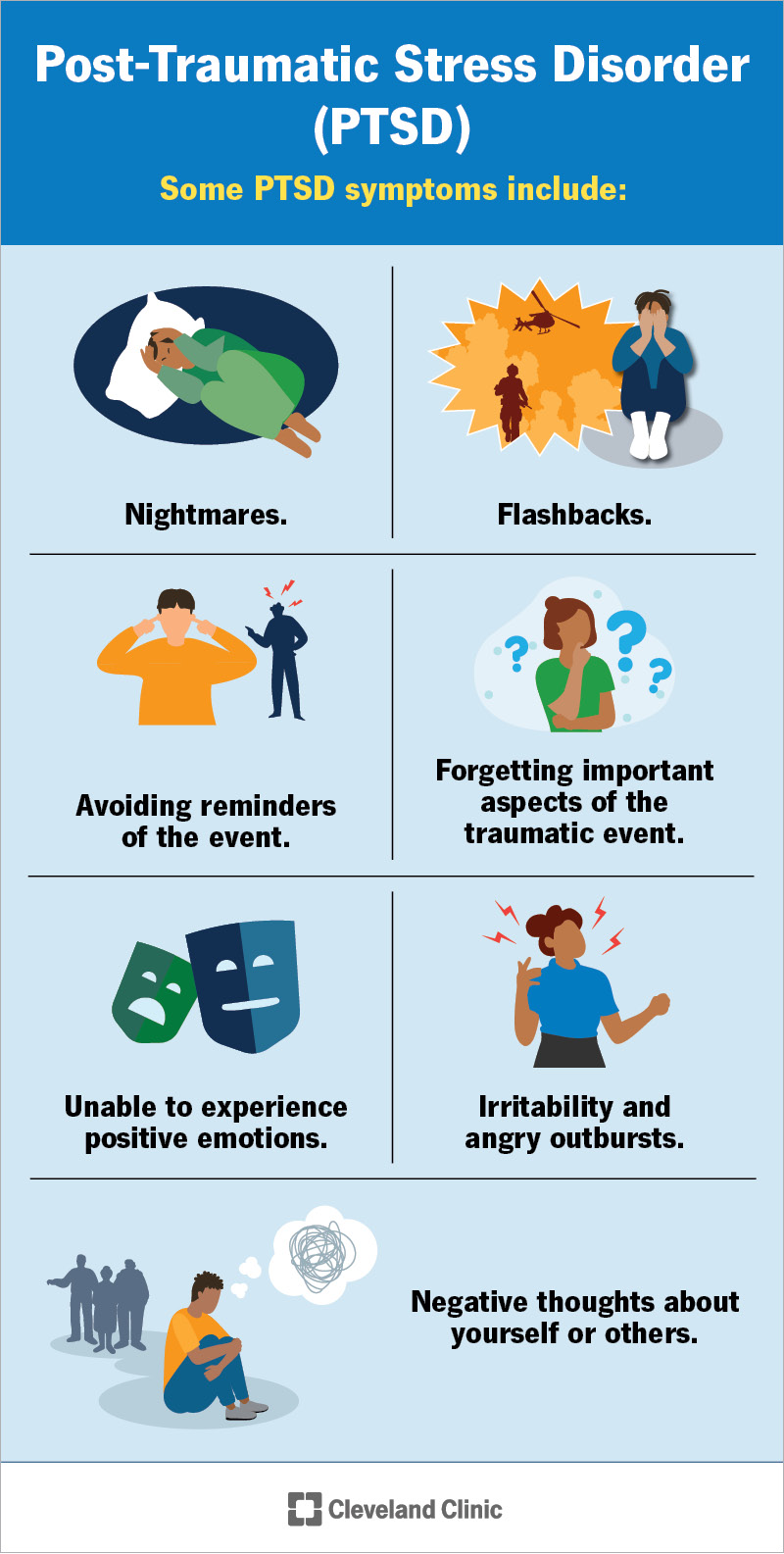
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/9545-post-traumatic-stress-disorder-ptsd.jpg)
Symptoms of post-traumatic stress disorder usually fall into four main groups. Each group affects how you think, feel or react after a traumatic event. If symptoms last more than a month or interfere with daily life, talk to a healthcare provider.
These bring the negative memory back into your mind, even when you don’t want to think about it. You might:
These involve trying to stay away from reminders of the trauma. You might:
These affect how you feel about yourself, others and the world around you. You might:
These affect how alert or reactive your body feels. You may:
This condition can look different in children. And kids may not have the words to explain how they feel.
Common PTSD symptoms in kids may include:
Some symptoms can also look like ADHD, so it’s important to have a mental health specialist evaluate your child. If you notice these symptoms lasting or getting worse, a pediatrician can help determine the next steps for children.
A trigger is something that reminds you of the trauma and makes symptoms feel more intense.
Triggers can include sights, sounds, smells, places or situations. For example, a loud noise or fireworks may bring back memories from a war zone, or a song may remind you of someone who hurt you. Even certain dates or times of year can cause symptoms to flare. When a trigger happens, symptoms like anxiety, flashbacks or strong emotions may return, even if you were feeling better before.
Advertisement
Triggers are a normal part of this condition. A healthcare provider can help you identify them and manage your reaction.
Exposure to a traumatic event causes post-traumatic stress disorder. Trauma is a situation that feels life-threatening or deeply stressful. Examples of these events include:
Many people experience these situations, but not everyone develops PTSD. Experts don’t fully understand why people respond differently. Research shows that this condition may involve changes in brain chemicals and how certain parts of your brain work:
Advertisement
PTSD can affect anyone. But certain factors may raise the risk before, during or after an experience.
Risk factors include:
Having one or more risk factors doesn’t mean you’ll develop PTSD, but it may make managing this condition more difficult without support.
PTSD may affect more than your emotions. Over time, symptoms may lead to other mental health, physical and life challenges if they aren’t treated. Complications may include:
In children and teens, complications may also include:
Advertisement
If you or a loved one is thinking about suicide, call or text 988 to reach the Suicide and Crisis Lifeline. Someone is available to help you 24/7.
There’s no single test to diagnose PTSD. Instead, a mental health specialist makes the diagnosis by talking with you about your symptoms, your medical and mental health history, and any trauma you’ve experienced. It can all be hard to talk about, so you may want to bring a trusted person with you for support.
In some cases, your provider may order blood tests to rule out other medical causes of your symptoms. There are no lab tests that can diagnose PTSD directly. They may also use questionnaires or interviews to better understand how your life experiences affect you.
Your provider may also check for related conditions like depression, anxiety or substance use, as these may occur alongside PTSD.
To diagnose this condition, a mental health provider compares your symptoms to criteria in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR). The criteria include:
PTSD treatment often includes therapy and medications. Many people benefit from using both together. Your provider will work with you to choose what fits your symptoms, needs and comfort level.
Therapy is usually the first choice for treating this condition. There are different types to help you process negative experiences and build coping skills:
Medications may help you manage symptoms, especially when therapy feels hard to start.
Your provider can adjust your treatment plan as your needs change.
Alternative therapies are nontraditional approaches that may support PTSD treatment. Providers often recommend them alongside therapy and medications to help manage stress and other symptoms.
Options may include:
Reach out to a provider if you:
If you feel at immediate risk of harming yourself, seek emergency help right away or call or text 988 to reach the Suicide and Crisis Lifeline.
PTSD doesn’t have a quick cure, but it can be managed. Some days may feel harder, especially during stress or reminders. Progress often isn’t a straight line, and ups and downs are common.
This condition doesn’t define who you are, but it may change your routines, relationships and energy for a while. With support, you might find ways to reconnect with work, relationships and activities that matter most to you.
Finding the right treatment can take time. Your provider may adjust your plan as your needs change. Improvement often happens gradually. Even when symptoms don’t fully disappear, they may feel less disruptive over time.
You can’t prevent all causes. But certain steps after trauma may lower the risk and support your recovery. You may try:
Post-traumatic stress disorder (PTSD) may change the way you feel and think — often in ways that are hard to explain to others. Whether your symptoms began recently or have been building over time, it’s OK to acknowledge that things feel different.
Healing doesn’t mean forgetting what happened. It means finding ways to carry your experiences with less weight and more support, often through evidence-based treatments and supportive relationships. That might look like therapy, medications, connecting with others or simply learning new ways to cope when triggers show up.
Progress can take time. That’s not a sign of failure. It’s part of how healing works.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your mental well-being is just as important as your physical well-being. Cleveland Clinic’s mental health experts can help you live life to the fullest.
