Cardiac arrest happens because of an electrical issue that makes your heart stop beating. When your heart stops pumping blood, you become unconscious. Cardiac arrest can be fatal in minutes. This is why bystanders should call for help and start CPR immediately. A person’s chances of survival are best when they get help right away.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cardiac arrest happens when your heart stops beating or beats so fast that it stops pumping blood. During cardiac arrest, people typically collapse and become unresponsive. Symptoms start without warning. This is why people also call it sudden cardiac arrest.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This life-threatening condition can become fatal if you don’t get immediate treatment.
During cardiac arrest (cardiopulmonary arrest), your heart isn’t pumping blood anymore. Within minutes, this puts your organs and whole body at risk of death because they must constantly receive oxygen. Your blood delivers that oxygen.
Emergency treatment includes cardiopulmonary resuscitation (CPR) and defibrillation. CPR keeps enough oxygen in your lungs and gets it to your brain until an electric shock restores a normal heart rhythm. CPR and defibrillators may save your life.
Call 911 (or your local emergency services number) if you see someone drop to the ground and you suspect sudden cardiac arrest. The faster someone gets help, the better their chances of survival with good health outcomes.
More than 356,000 Americans each year experience cardiac arrest outside of a hospital. It typically affects adults, but it can happen in children, too.
Sudden cardiac arrest happens in people with and without heart disease. Having a heart attack or other heart condition can significantly increase your risk.
Cardiac arrest symptoms may include:
Advertisement
Sudden cardiac arrest happens without preceding symptoms.
Before you faint, you may have other signs of cardiac arrest, including:
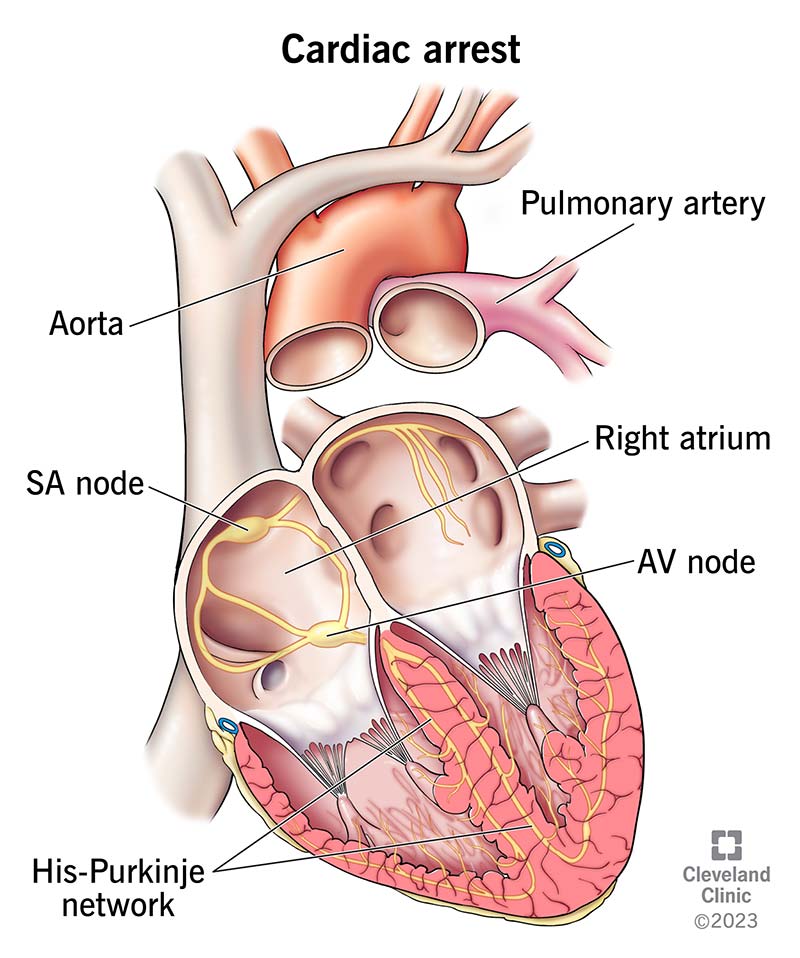
Before cardiac arrest, abnormal, rapid impulses abruptly override the normal electrical impulses that start your heartbeat.
Abnormal heart rhythms (arrhythmias) cause most sudden cardiac arrests. The most common life-threatening arrhythmia is ventricular fibrillation (also called v-fib). This is an erratic, disorganized firing of impulses from your heart’s ventricles (lower chambers). When this happens, your heart can’t pump blood. When your heart isn’t beating, there’s no way to get oxygen-rich blood to the rest of your body.
Without treatment, you can die within minutes.
Conditions and situations that can lead to these abnormal heart rhythms are the underlying causes of sudden cardiac arrest. These include:
Other cardiac arrest causes include:
Some of these issues lower oxygen levels or reduce the volume of blood. This prevents your heart from functioning.
You may be at a higher risk for cardiac arrest if you:
Survivors of cardiopulmonary arrest often have medical issues that continue months or years later. They may deal with:
Cardiac arrest symptoms begin suddenly, leaving little time for tests. The condition can become fatal within minutes. This is why a quick diagnosis is essential.
A person’s symptoms are often the best way to diagnose cardiac arrest, especially if they:
Advertisement
You can treat and reverse sudden cardiac arrest. But cardiac arrest treatment has to start immediately, wherever you are. Survival can be as high as 90% if treatment starts within the first minutes after sudden cardiac arrest. The rate drops by about 10% each minute longer.
Sudden cardiac arrest can be fatal if it lasts longer than eight minutes without CPR. Brain damage can happen after just five minutes.
If you see someone experiencing sudden cardiac arrest, do this:
Once emergency personnel arrive, defibrillation can restart the person’s heart if they haven’t received a shock from an AED yet. Defibrillators shock your heart through paddles placed on your chest. The current travels to your heart. This stops the abnormal impulses and restores the normal impulses that make it beat. It may take more than one shock for your heart to pump on its own again.
Advertisement
Through an IV (intravenous) in your arm, emergency personnel will give you antiarrhythmics. These medications work to restore your heart’s electrical rhythm.
After successful defibrillation, most people need hospital care to recover from the effects of their sudden cardiac arrest and to treat and prevent future heart problems.
CPR can cause chest injuries like broken ribs or a broken breastbone (sternum). Some people also have injuries to their abdomen (belly). But these are worth the risk to save someone’s life.
After returning home, complications can happen. You may need to go back to the hospital for treatments for kidney failure, liver failure and long-term heart disease.
People who survive sudden cardiac arrest have a varied outlook, depending on how quickly they received medical treatment. They usually need help regaining skills they had before their sudden cardiac arrest. This happens because you can have brain damage if too many minutes pass without oxygen reaching your brain.
Nearly 9 out of 10 people who survive cardiopulmonary arrest have permanent brain damage from a lack of oxygen. This can bring changes to your daily life and abilities.
You may experience:
Advertisement
Survival without brain damage is far more likely with early CPR and defibrillation.
Yes, you can survive cardiac arrest. But it’s not common. Most people who have a sudden cardiac arrest outside of a hospital don’t survive. This is usually because they don’t get help in time.
Still, survival rates are better than they were just 10 years ago. About 11% of people who have cardiac arrest outside a hospital and get emergency treatment survive and go home from the hospital. About 26% of people who have cardiopulmonary arrest inside a hospital survive and go home.
Yes, it’s possible to prevent a cardiac arrest.
If abnormal heart rhythms run in your family, you may want to talk with a genetic counselor. They can tell you who might be at risk or need testing for an issue that causes arrhythmia.
Testing can let you know whether you’re at risk for sudden cardiac arrest.
To prevent future episodes of sudden cardiac arrest, your healthcare provider will want to do tests to figure out what caused your cardiac event. Tests may include:
Treatments that can prevent cardiac arrest or lower your risk of a second episode include:
You can help prevent cardiac arrest by working on your risk factors for it. That means managing conditions that put you at risk (like high cholesterol, high blood pressure and diabetes) and living a healthy lifestyle. This includes:
Surviving sudden cardiac arrest is the start of a long recovery for many. Depending on how long your brain was without oxygen, you’ll likely have brain damage.
If a rehabilitation program is available, you can use it to regain your abilities. It can take months to relearn once-simple activities like walking and getting dressed. Many people return to their daily lives, but some need ongoing help.
Be patient with yourself while you slowly get back to being able to do things you did every day. Researchers have seen improvements in cardiopulmonary arrest survivors’ quality of life after six months.
Surviving a life-threatening condition can cause mental health challenges (post-intensive care syndrome).
You may benefit from mental health services to help you cope with:
You’ll most likely have follow-up appointments with multiple healthcare providers as you recover from sudden cardiac arrest. You’ll also have procedures or treatments that can help prevent you from having another sudden cardiac arrest.
Be sure to tell your provider if you’re having any new symptoms or if you aren’t feeling better during the expected time frame.
If you witness someone collapsing into unconsciousness, call 911 or your local emergency number. They can send help and talk you through giving CPR. Start CPR and send someone else to find an AED.
Questions you may want to ask your provider include:
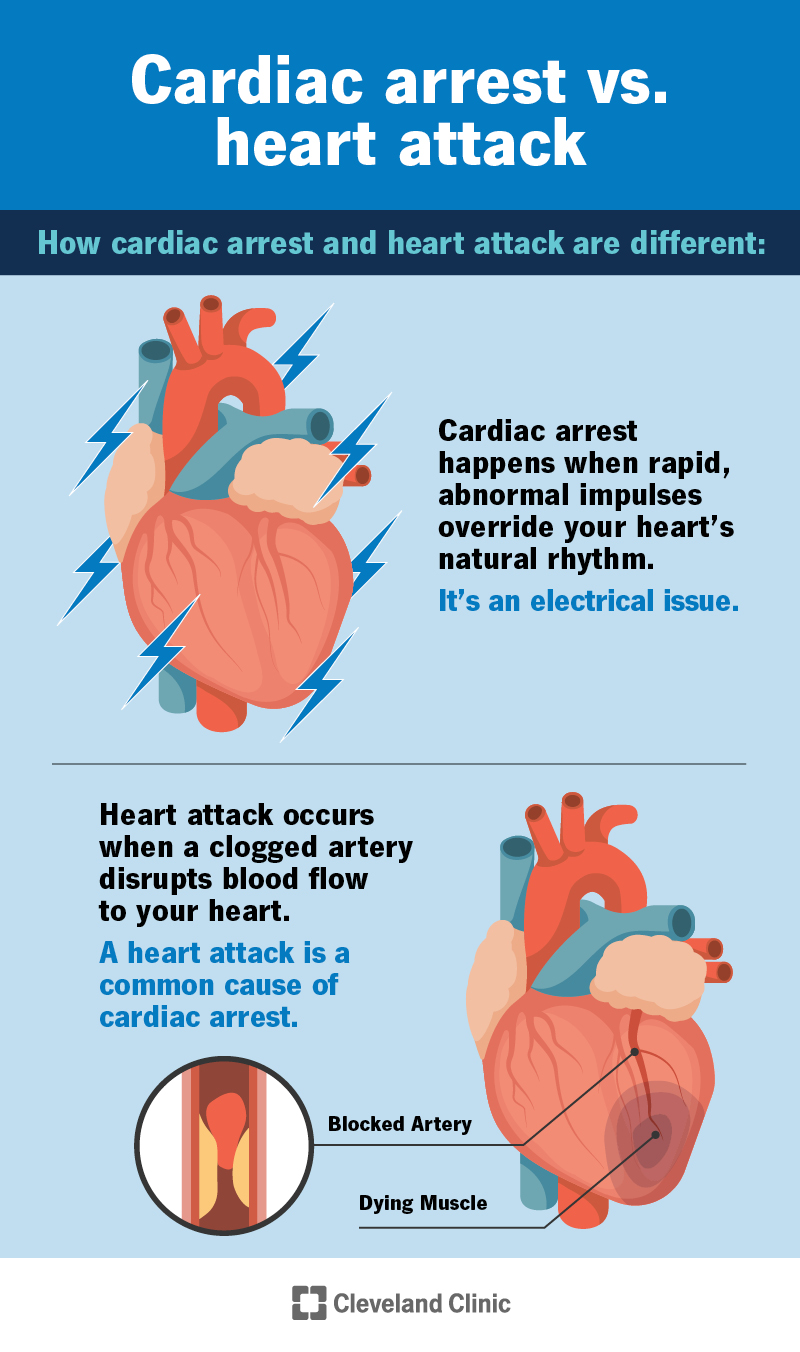
The difference between a cardiac arrest and a heart attack is that a cardiac arrest happens because of an electrical issue and a heart attack comes from a blood flow issue.
Sudden cardiac arrest isn’t a heart attack. But you can have one after a heart attack.
With cardiac arrest, your heart stops beating, but a rescue is still possible. With immediate treatment, you can survive.
Sudden cardiac death refers to cardiac arrest without someone saving you.
Some people have chest pain before they become unconscious from cardiac arrest. However, you won’t feel pain once you lose consciousness. People may experience chest pain after receiving CPR.
Recovery from cardiac arrest takes time and includes therapies to help maximize your abilities. Many survivors need ongoing heart care to prevent another episode of sudden cardiac arrest. Be sure to go to all of your follow-up appointments and keep taking any prescribed medicines. It may give you peace of mind if people who live with you take a CPR class in case of another cardiac arrest. Most cardiac arrests outside a hospital happen at home.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.

Last reviewed on 12/27/2023.
Learn more about the Health Library and our editorial process.