Hashimoto’s disease is a chronic autoimmune disease that affects your thyroid gland. It can cause lower-than-normal levels of thyroid hormone in your body. This affects several areas of your body and causes symptoms like fatigue, weight gain and constipation. Hashimoto’s disease is treatable with medication.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
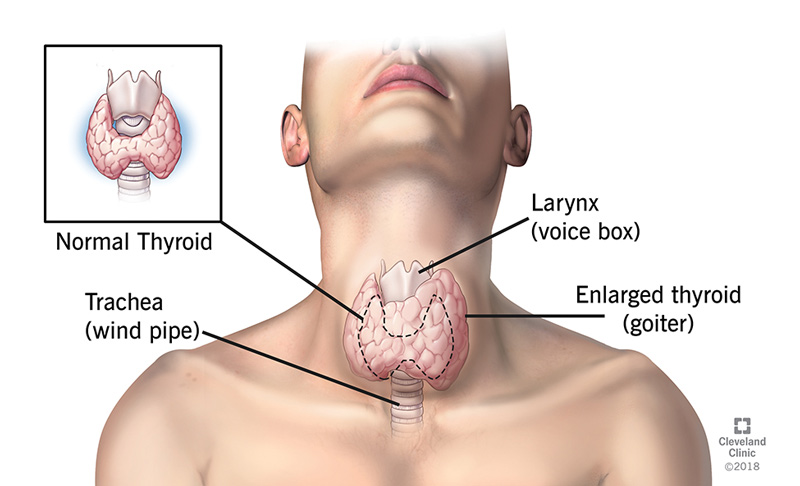
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17665-hashimotos-disease)
Hashimoto’s disease is an autoimmune condition that can cause hypothyroidism (underactive thyroid). It’s a lifelong (chronic) condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your thyroid is a small, butterfly-shaped gland located at the front of your neck under your skin. It’s a part of your endocrine system and releases thyroid hormones.
Your thyroid’s main job is to control the speed of your metabolism. This is the process of how your body transforms the food you consume into energy. It’s common to mainly think of metabolism in terms of weight gain or weight loss. But this process affects every organ in your body, including your heart and brain.
In most cases of Hashimoto’s disease, your thyroid can’t produce enough thyroid hormone for your body. This slows down your metabolism and causes a range of symptoms.
The condition is named after Dr. Hakaru Hashimoto, who identified it in 1912. Other names for Hashimoto’s disease include:
Hashimoto’s disease is common. It affects about 5 in 100 people in the United States.
Hashimoto’s disease is the most common cause of hypothyroidism in countries with widely available iodized salt and other iodine-enriched foods. Iodine deficiency is the most common cause in other countries.
Anyone at any age can develop Hashimoto’s disease. But females are 10 times more likely to get it than males. Diagnosis most commonly occurs between the ages of 30 to 50 for females.
Advertisement
Some people with Hashimoto’s disease may not have any symptoms at first.
As the condition slowly progresses, your thyroid gland will sometimes become enlarged (a condition called goiter). Goiter is a common first sign of Hashimoto’s disease. It’s shouldn’t hurt, but it can create a feeling of fullness in your lower neck. It can make the front of your neck look swollen.
If Hashimoto’s disease leads to hypothyroidism, it can cause the following symptoms over time:
You might not feel different if you have Hashimoto’s disease without hypothyroidism.
However, if you develop hypothyroidism, it can make you feel “off.” “Hypo-” means “low” or “under.” So you can think of symptoms of hypothyroidism as a slowing down of various bodily functions.
You may have less energy than you used to or can’t exercise as much or as long as you once did. If you have a fitness tracker, you may notice that your heart rate is slower than it used to be. You may have brain fog or problems remembering things. Hypothyroidism can also “slow down” your mood — you may feel sad or depressed. It can also lower your sex drive and your digestive system — you may not poop as frequently as before.
If your body and mind feel stuck in slow motion, talk to your healthcare provider.
Hashimoto’s disease is an autoimmune disease, which means your body’s immune system attacks your cells and organs.
Normally, your immune system protects your body against harmful outside invaders, like bacteria and viruses. But in Hashimoto’s disease, the following happens:
Factors that may increase your risk of developing Hashimoto’s disease include your:
Advertisement
You’re also more likely to get Hashimoto’s if you have other autoimmune conditions, like:
First, your healthcare provider will:
After this assessment, they’ll order blood tests to confirm the diagnosis, including:
In some cases, your provider may recommend a thyroid ultrasound (imaging test) to check the size of your thyroid and to make sure you don’t have thyroid nodules (growths).
Not everyone with Hashimoto’s disease develops hypothyroidism. If you have high antibody levels but don’t have clinical hypothyroidism, your healthcare provider will likely monitor your thyroid levels instead of starting treatment.
Advertisement
If Hashimoto’s disease leads to hypothyroidism, the go-to treatment is a medication called levothyroxine. It’s a synthetic (manufactured) form of the hormone T4 that your thyroid makes.
Brand names of levothyroxine include:
This medication helps restore the normal levels of thyroid hormone your body needs. You’ll need to take it every day for the rest of your life.
Over time, you may need a different dose of the medication. Your provider will know how to adjust your dose to make sure that your hypothyroidism is well-managed.
If you experience side effects from levothyroxine, it’s most likely because your dose is too high. This can cause thyrotoxicosis — too much thyroid hormone.
Symptoms of thyrotoxicosis include:
There’s no special diet for Hashimoto’s disease. But some foods, medicines or supplements may affect your ability to absorb levothyroxine. These include:
Advertisement
Taking these four hours before or after you take levothyroxine may solve this problem.
Talk to your healthcare provider or a registered dietitian about any dietary questions you have.
Eating well and having a healthy lifestyle — exercising, sleeping well and managing stress — can help your immune system. But no matter what, you’ll need to keep taking your medications if you have hypothyroidism.
There’s no way to cure or reverse Hashimoto’s disease. But lifelong medication works well to manage hypothyroidism and your thyroid hormone levels.
With lifelong monitoring and treatment, the prognosis (outlook) for people with Hashimoto’s disease is excellent.
If you have hypothyroidism from Hashimoto’s disease that’s untreated, it can lead to certain health problems, including:
Without treatment, hypothyroidism can also cause problems during pregnancy.
Untreated hypothyroidism during pregnancy can increase the risk of:
Or it may cause a dangerous rise in your blood pressure in late pregnancy called preeclampsia. Untreated hypothyroidism can also affect the fetus’s growth and brain development. Your providers will work with you to make sure your hypothyroidism is well-managed during pregnancy.
Hypothyroidism during pregnancy isn’t common. But it can be easy to miss its symptoms that are also common during pregnancy, like fatigue and weight gain. Let your providers know right away if you notice any hypothyroidism symptoms or feel like you’re developing a goiter.
Unfortunately, there’s nothing you can do to prevent Hashimoto’s disease. The risk factors for it — like your genetics and age — aren’t modifiable.
If you have Hashimoto’s disease, you’ll need to see your healthcare provider regularly. They’ll perform routine thyroid hormone blood tests to make sure your levels are in range and that the dose of medication you’re taking is right for you.
Otherwise, see your healthcare provider if you develop new or worsening symptoms or notice a change in your thyroid.
If you have symptoms of myxedema coma, call 911 or get to the emergency room as soon as possible. This complication of severe hypothyroidism is life-threatening.
Symptoms include:
Getting a new diagnosis can be stressful. The good news is that Hashimoto’s disease is a manageable and treatable condition. If you’re experiencing symptoms of Hashimoto’s or have certain risk factors, such as a family history of thyroid disease, be sure to contact your healthcare provider. They can run some simple tests to see if your thyroid isn’t making enough thyroid hormone.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s experienced healthcare providers treat all kinds of thyroid disorders, including issues that cause hypothyroidism and hyperthyroidism.
