Hyperlipidemia (high cholesterol) is an excess of lipids or fats in your blood. This can increase your risk of heart attack and stroke because blood can’t flow through your arteries easily. Adding exercise and healthy foods can lower your cholesterol. Some people need medication, as well. Managing your cholesterol is a long-term effort.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
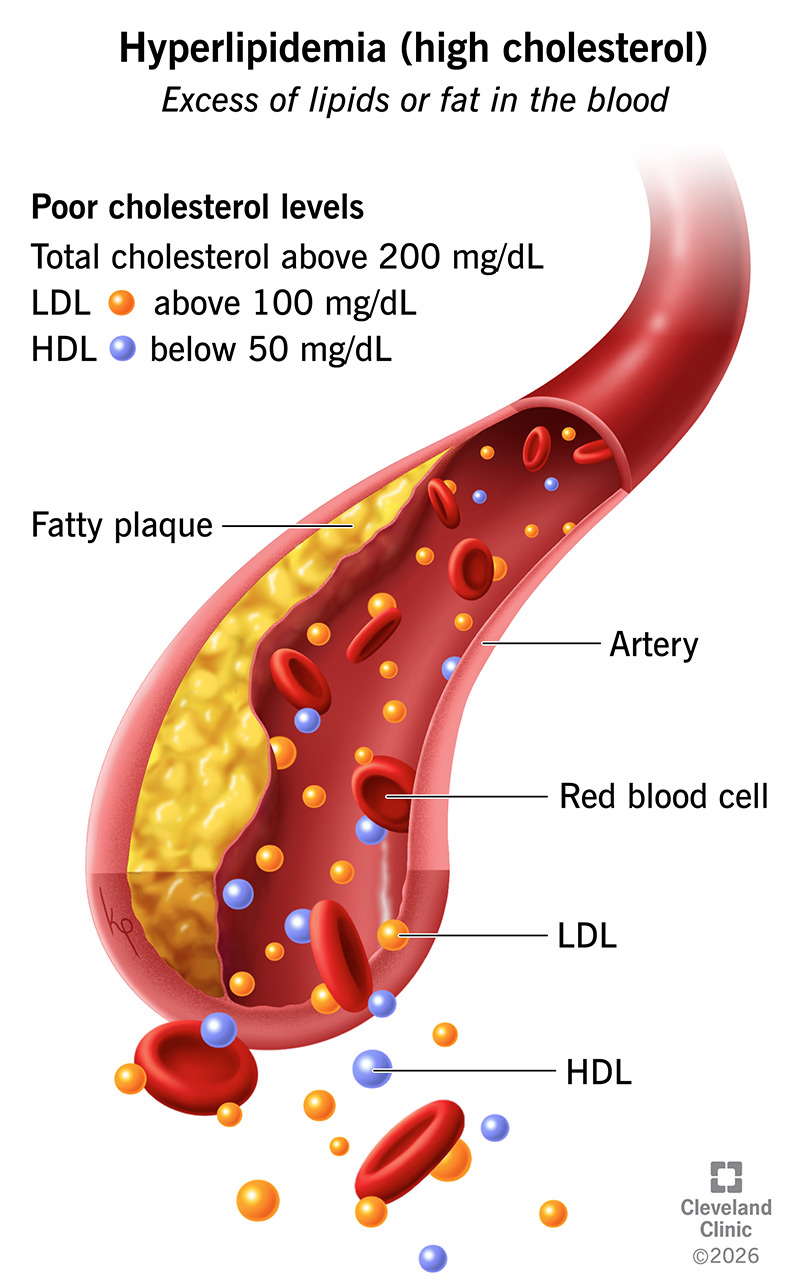
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21656-hyperlipidemia)
Hyperlipidemia (high cholesterol) means you have too many lipids (fats) in your blood, which increases your risk of heart attack and stroke. Your liver creates cholesterol to help you digest food and make things like hormones. But you also eat cholesterol in meat and dairy products. Because your liver can make as much cholesterol as you need, the cholesterol in foods you eat is extra.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
High levels of cholesterol in the blood may lead to a buildup of plaque in your blood vessels, particularly arteries. As plaque builds up in an artery, it gradually reduces the amount of blood that can flow through that artery. As a result, some organs may not receive enough blood. Over time, this can result in permanent damage to those organs.
Bad cholesterol (LDL) is the most dangerous type because it causes deposits of cholesterol and fats (plaque) to collect inside of your blood vessels. This makes it harder for your blood to get through.
Think of cholesterol, a kind of fat, as traveling in lipoprotein (fat and protein) cars through your blood.
Advertisement
Hyperlipidemia is a very common cause of heart and blood vessel disease, which remains the leading cause of death in the U.S.
High cholesterol doesn’t cause symptoms directly. But it plays a role in developing coronary artery disease that leads to chest pain, for example. Over time, plaque buildup can slow down or stop blood flow to your heart or brain. You may feel chest pain with exertion, jaw pain and shortness of breath.
Plaque in a heart artery can lead to a heart attack, with symptoms like severe chest pain, flushing, nausea and difficulty breathing. This is a medical emergency.
People who have a genetic problem that causes very high cholesterol levels may get xanthomas (waxy, fatty plaques on their skin) or corneal arcus (cholesterol rings around the irises of their eyes).
Many different things can cause high cholesterol. Some are beyond your control. Others are factors you can change.
Causes include:
Several things can put you at a higher risk of hyperlipidemia, including:
Without treatment, high cholesterol can let plaque collect inside your body’s blood vessels (atherosclerosis). This can bring on complications that include:

Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21656-high-cholesterol-diseases-infographic-cv)
High cholesterol can cause many complications, like a stroke or heart attack, that affect your heart and blood vessels.
Your provider will order a blood test to check the cholesterol levels in your blood. They can help you interpret your numbers and prescribe a treatment tailored to you.
A blood test called a lipid panel will tell you these numbers:
Your provider will also do a physical exam and ask about your personal and family medical history. They may also do these tests:
High cholesterol can start in childhood or adolescence. That’s why current guidelines suggest it might be reasonable to screen all children for high cholesterol. The guidelines are:
Advertisement
These are general guidelines. Talk to your healthcare provider about the right time to check your cholesterol levels. Someone in their 20s with high cholesterol numbers may need yearly tests for a while. People with other heart disease risk factors may need more frequent tests, too.
You may be able to just change your daily habits to improve your high cholesterol levels. If that’s not enough, you may need medication. People who need medicine to treat their high cholesterol usually take statins. These decrease how much bad cholesterol is circulating in your blood. Your provider may order a different type of medicine if you can’t take a statin or need another medicine in addition to a statin.
Things you can do include:
Advertisement
You should see your provider if your blood test shows that you have high cholesterol. Your provider will order another blood test about two or three months after you start taking medication or making changes. The test results will show whether your cholesterol levels have improved, which means the medicine and/or lifestyle changes are working.
Questions to ask your provider may include:
Although high cholesterol puts you at risk for heart attacks and stroke, you can protect yourself. Making a few changes in your daily routine and taking medicine if needed can help. Talk to your provider about estimating your risk of heart disease and stroke so they can help you manage your risk.
Hyperlipidemia is a condition you’ll need to manage for the rest of your life. You’ll need to keep using healthy habits for years to come. You’ll also need to have follow-up visits with your provider and continue to take your medicine. If you and your provider are able to manage your cholesterol level, you may not have serious health problems from it.
Advertisement
Changes you make in your daily habits can keep you from getting hyperlipidemia. Things you can do include:
Hyperlipidemia, or high cholesterol, can let plaque collect inside your blood vessels and put you at risk of a heart attack or stroke. The good news is that there are ways to reduce your risk. Ask your provider what you can do to improve your cholesterol numbers. Taking medicine your provider orders makes a difference, too.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you need treatment for coronary artery disease, you want expert care. At Cleveland Clinic, we’ll create a treatment plan that’s personalized to you.
