Blood pressure is the amount of force your blood uses to get through your arteries. A normal blood pressure reading for most adults is below 120/80 mm Hg. Blood pressure that’s too high raises your risk for heart disease. But blood pressure that’s very low can also cause issues. Seeing a provider for yearly blood pressure checks can be lifesaving.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_07a9lgme/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Learn how blood pressure is measured.
Blood pressure is a measure of the force of blood inside your arteries. Each time your heart beats, it pumps blood into a large artery called your aorta. This happens 60 to 100 times a minute, 24 hours a day. Your aorta connects to other arteries that deliver oxygen and nutrients to all your organs and tissues.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your blood pressure doesn’t stay the same all the time. It changes based on what you’re doing. When you’re exercising or excited, your blood pressure goes up. When you’re resting, your blood pressure is lower. Your blood pressure can also change because of medicines you take, shifts in your body position and aging.
Blood pressure matters because it can have a big effect on your health. For example:
You usually can’t tell what your blood pressure is just by how you feel. The only way to know your blood pressure is to measure it with proper equipment. This typically happens at your healthcare provider’s office. You can also check your blood pressure at home — but this shouldn’t replace seeing your provider.
You should check your blood pressure at least once a year. Your healthcare provider will measure it for you at each annual physical exam. You may need more frequent blood pressure checks if your provider is concerned about your numbers or wants to see how well treatment is working.
Advertisement
Your provider may also ask you to check your blood pressure at home. They’ll tell you how often to do this — anywhere from several times a day to once a week.
In certain situations, they may ask you to do 24-hour blood pressure monitoring. This lets your provider see how your blood pressure changes over the course of your day and even while you sleep. It can also diagnose white coat syndrome. This is when your blood pressure is high at your provider’s office because you’re nervous.
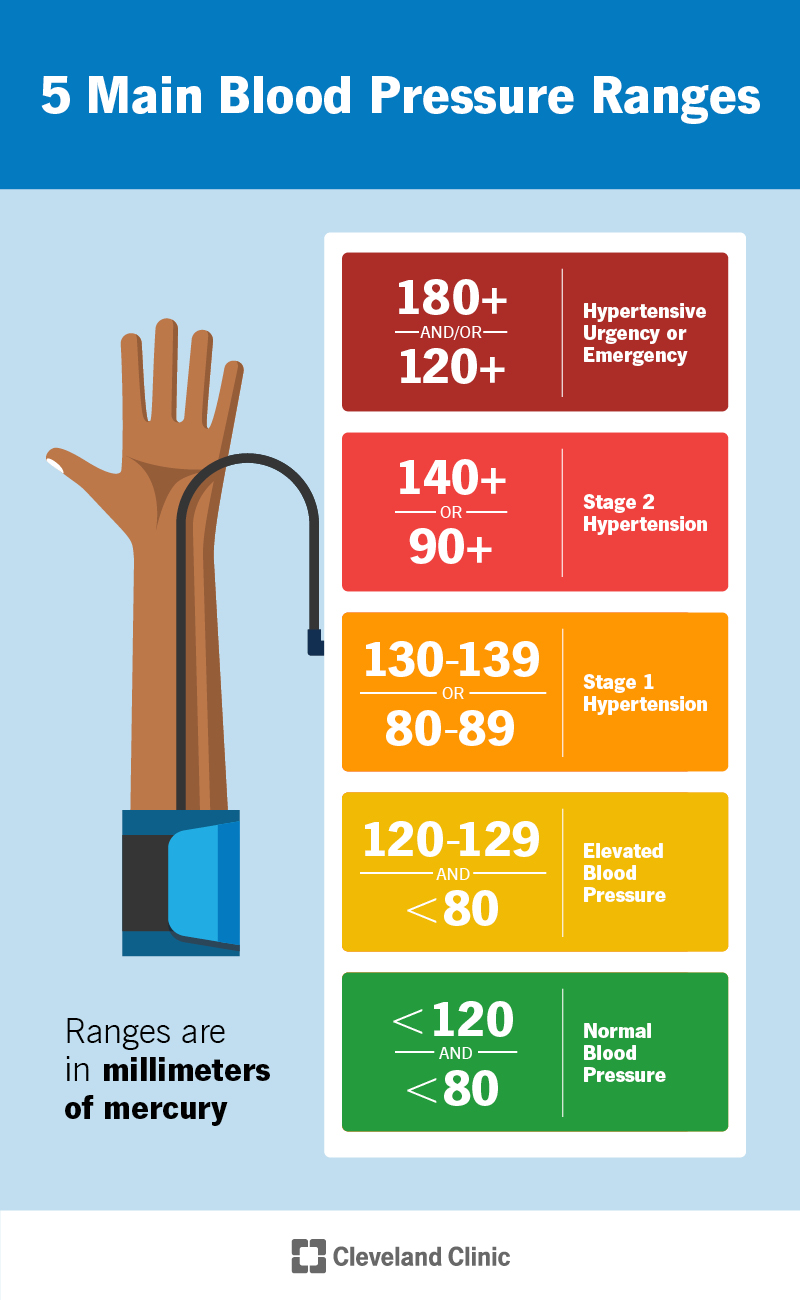
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17649-blood-pressure)
A blood pressure test measures how hard your blood is pushing against the walls of your arteries at two key moments — when your heart is pumping out blood and when it’s at rest. That’s why there are two numbers that make up your blood pressure reading:
There are two main ways your healthcare provider can measure your blood pressure:
To get the most accurate blood pressure reading:
You may also want to wear short sleeves. This will make it easier for your provider to put the cuff on your arm.
A blood pressure check is fast and noninvasive. Nothing goes into your body. Your provider wraps a cuff around your upper arm. The cuff squeezes and then releases over the course of about a minute. During this time, your provider records your blood pressure numbers.
The cuff gets very tight around your arm when it’s inflated. This might feel uncomfortable, but it’s only for a few seconds.
Your provider will help you sit in a position that allows the best reading. For example, you should:
Your provider may check your blood pressure more than once during your appointment. This can help them get the most accurate reading, especially if you’re nervous.
Your provider will check your blood pressure manually or automatically — or both.
Advertisement
Your provider will follow these steps to manually measure your blood pressure:
Advertisement
Another option is to measure your blood pressure using an automatic device. It’s similar to what you might use at home. But providers test these devices often to make sure they’re accurate.
Your experience won’t be much different from a manual reading. A cuff will still squeeze your arm. But your provider won’t use a stethoscope or look at a gauge. Instead, they’ll check the device’s digital read-out screen to see your blood pressure numbers.
Once your provider measures your blood pressure, they’ll continue with the rest of the physical exam. They may talk with you about your blood pressure numbers.
You’ll know your blood pressure reading right away. But if your numbers are high, you may need to come back for another appointment. This is because your provider needs two or more readings, on different days, to diagnose high blood pressure (hypertension). They take an average of these readings.
If you’re diagnosed with hypertension, your provider will talk with you about treatment options. Medicine can lower your blood pressure and help protect you from serious complications down the road. If you’re diagnosed with low blood pressure, your provider will find the underlying cause and treat it.
Advertisement
Healthcare providers generally use the following categories to describe your blood pressure (these apply to all adults, regardless of sex):
| Blood pressure category | Top number (systolic) | Bottom number (diastolic) | |
|---|---|---|---|
| Low | Below 90 | OR | Below 60 |
| Normal | Below 120 | AND | Below 80 |
| Elevated | 120 to 129 | AND | Below 80 |
| Stage 1 hypertension | 130 to 139 | OR | 80 to 89 |
| Stage 2 hypertension | 140 or higher | OR | 90 or higher |
| Hypertensive crisis (urgency or emergency) | 180 or higher | AND/OR | 120 or higher |
| Blood pressure category | |||
| Low | |||
| Top number (systolic) | |||
| Below 90 | |||
| OR | |||
| Bottom number (diastolic) | |||
| Below 60 | |||
| Normal | |||
| Top number (systolic) | |||
| Below 120 | |||
| AND | |||
| Bottom number (diastolic) | |||
| Below 80 | |||
| Elevated | |||
| Top number (systolic) | |||
| 120 to 129 | |||
| AND | |||
| Bottom number (diastolic) | |||
| Below 80 | |||
| Stage 1 hypertension | |||
| Top number (systolic) | |||
| 130 to 139 | |||
| OR | |||
| Bottom number (diastolic) | |||
| 80 to 89 | |||
| Stage 2 hypertension | |||
| Top number (systolic) | |||
| 140 or higher | |||
| OR | |||
| Bottom number (diastolic) | |||
| 90 or higher | |||
| Hypertensive crisis (urgency or emergency) | |||
| Top number (systolic) | |||
| 180 or higher | |||
| AND/OR | |||
| Bottom number (diastolic) | |||
| 120 or higher |
If your top number and bottom number fall into two different categories, your provider will use the higher category. For example, if your blood pressure is 132/78, your reading would fall into the stage 1 hypertension category.
An ideal blood pressure for most adults is lower than 120/80 mm Hg (millimeters of mercury). This means your systolic (top) number is below 120 and your diastolic (bottom) number is below 80. But blood pressure that’s too low may be a cause for concern. Hypotension is blood pressure below 90/60 mm Hg.
Keep in mind that what’s ideal or even normal can vary from person to person. For example, certain medical conditions or medicines could affect what your personal blood pressure goal should be. Be sure to ask your provider what that number is and how you can reach it.
Contact your healthcare provider if:
Call 911 or your local emergency services number if:
Your blood pressure is an important number that your healthcare provider tracks over the years. You could feel totally fine yet still have high blood pressure. Checking your numbers regularly is the only way to know if you’re in the healthy range.
If needed, your provider will recommend treatment to manage your blood pressure. And they’ll let you know when to come back for follow-up appointments. When it comes to protecting your heart, you and your provider are a team. Together, you can manage your blood pressure and lower your risk for cardiovascular disease.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
