A thyroid nodule is an unusual lump (growth) of cells on your thyroid gland. They’re common, almost always noncancerous (benign) and usually don't cause symptoms. In rare cases, they're cancerous.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
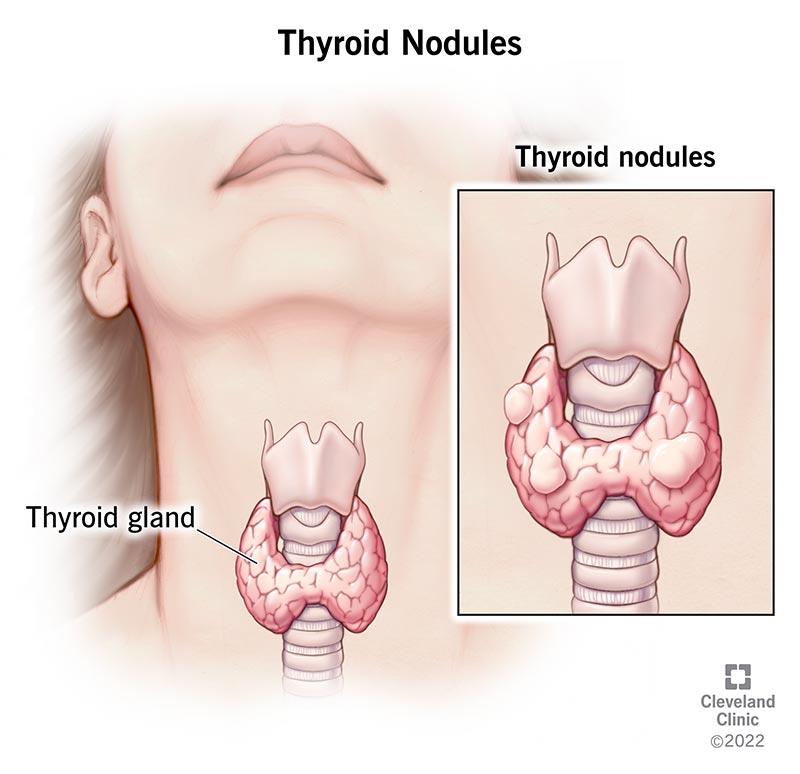
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/13121-thyroid-nodules-illustration)
A thyroid nodule is an unusual lump (growth) of cells on your thyroid gland.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your thyroid gland is a small, butterfly-shaped endocrine gland located in your neck, below your Adam's apple. It produces the hormones thyroxine (also called T4) and triiodothyronine (also called T3). These hormones play a role in certain bodily functions, including:
Thyroid nodules are classified as:
More than 90% of detected nodules in adults are noncancerous (benign), but they may represent thyroid cancer in approximately 4.0% to 6.5% of cases. Even though most thyroid nodules aren’t cancer, they can sometimes be a sign of and/or cause of thyroid disease.
Anyone can have a thyroid nodule, including children and adults. However, they’re about four times more common in females than males.
They also occur more often in people who live in countries where food isn’t fortified with iodine. (Iodine is necessary for your thyroid gland to make hormones.)
Other factors that lead to an increased risk of thyroid nodules include:
Advertisement
Thyroid nodules are common. Healthcare providers detect them in approximately 5% to 7% of adults during a physical examination. Ultrasound imaging reveals that 20% to 76% of adults have thyroid nodules.
Thyroid nodules are less common in children.
In most cases, thyroid nodules aren’t a cause for concern. But even though the vast majority of thyroid nodules are benign, some thyroid nodules do contain thyroid cancer.
For this reason, you should see your healthcare provider so they can evaluate the nodule to be sure it’s benign. As with all cancer, the earlier it can be diagnosed and treated, the better.
Most thyroid nodules don’t cause symptoms. However, if you have several nodules or large nodules, you may be able to see them.
In rare cases, nodules can grow big enough to cause symptoms like:
Hyperfunctioning thyroid nodules can lead to overproduction of thyroid hormones, also known as hyperthyroidism. Symptoms of hyperthyroidism include:
Thyroid nodules may also be associated with low thyroid hormone levels (hypothyroidism). Symptoms of hypothyroidism include:
Researchers don’t know why most thyroid nodules form. Nodules can form for various reasons, and there are different types, including:
Advertisement
Sometimes you can feel or see a thyroid nodule yourself, or your healthcare provider may discover it during a physical exam. Your provider may also discover a nodule with an imaging test done for another reason.
Even though thyroid nodules are almost always noncancerous (benign), the small chance that it could be cancer means that most thyroid nodules need some type of evaluation.
Your healthcare provider may order any of the following tests to help diagnose and evaluate a thyroid nodule:
Advertisement
Treatment depends on the type of thyroid nodule. Treatment options include:
The prognosis for noncancerous (benign) thyroid nodules is great. They often don’t need treatment, and only about 1% of benign thyroid nodules cause thyroid disease, which is treatable.
The prognosis for cancerous (malignant) thyroid nodules varies greatly depending on several factors, including:
Advertisement
If you have thyroid cancer, your healthcare provider will be able to give you a more accurate prognosis.
Since researchers don’t know what causes the majority of thyroid nodules, you can’t prevent them in most cases.
You can, however, try to decrease your risk of developing them by managing certain risk factors. For example, if you have obesity, talk to your healthcare provider about attaining a healthy weight for you. If you smoke cigarettes, try to quit. It’s also important to make sure you get enough iodine in your diet. If you use iodized table salt, you’re likely consuming enough.
Studies have shown that people who take oral birth control and/or statins may have a reduced risk of developing thyroid nodules.
If you notice a bump on your thyroid, it’s important to see your healthcare provider. Even though the majority of thyroid nodules are benign and cause no other symptoms, it’s still important to have the nodule evaluated in the small chance that it’s cancer.
If you’ve been diagnosed with a thyroid nodule and are taking the “watch and wait” approach, you’ll need to see your provider regularly so that they can monitor the nodule for any changes.
Thyroid nodules are much less common in children than in adults, but researchers aren’t sure of the exact numbers.
There’s an increased risk of thyroid cancer in nodules found in children and adolescents compared to adults. However, over 75% of nodules found in children and adolescents are noncancerous (benign).
The symptoms, diagnosis and treatment of thyroid nodules for children are the same as for adults (as detailed in the above sections).
Thyroid nodules are very common, and they’re usually not a cause for concern. However, it’s still important to see your healthcare provider if you notice a lump on your thyroid (in the front of your neck). They may run some tests to make sure it’s benign. If you have any questions about your risk of developing thyroid cancer or thyroid disease, talk to your provider. They’re available to help you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you have thyroid nodules, you’ll want the best care. Cleveland Clinic’s healthcare providers are here to craft a personalized treatment plan for you.
