A bicuspid aortic valve is an aortic valve that has two cusps (flaps) instead of the usual three. It’s the most common congenital heart defect and affects up to 2% of the population. A bicuspid aortic valve can cause serious complications like heart failure. But with treatment, it won’t affect your life expectancy and you can lead a healthy life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
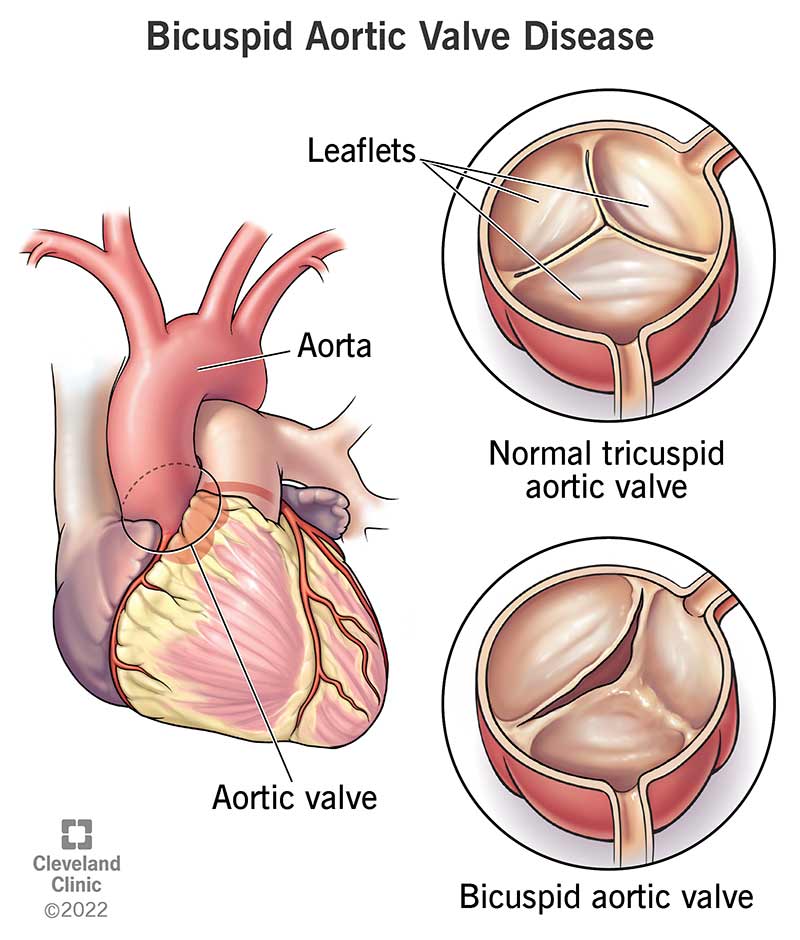
Bicuspid aortic valve disease is a congenital (present at birth) heart condition. It means your aortic valve (between your heart and your aorta) only has two flaps or cusps instead of the typical three. With only two flaps, your aortic valve may have trouble closing and opening properly.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Your aortic valve cusps or leaflets open and shut to regulate blood flow between your heart and your aorta. These flaps make sure your oxygen-rich blood flows out of your heart and into your aorta. They prevent blood from flowing backward into your heart. The flaps should open widely to let blood flow out of your heart and then close securely.
If your aortic valve doesn’t close tightly enough, blood leaks backward from your aorta into your heart. This is aortic regurgitation.
If your aortic valve doesn’t open wide enough, less blood can flow from your heart to nourish the rest of your body. This is aortic stenosis (narrowing).
You might have aortic regurgitation or stenosis for years and not even realize it. You may not feel any symptoms. Your aortic valve does its best to keep getting the job done. It’s just not as efficient as a valve with three flaps.
Over time, though, your bicuspid aortic valve makes your heart work harder, and this can lead to serious complications. While it can be difficult to accept this reality, learning about your condition can help you understand it better.
About 1 in 3 people with a bicuspid aortic valve develop complications. They can be very serious or even fatal. That’s why people with a bicuspid aortic valve disease diagnosis need ongoing medical checkups and testing.
Advertisement
About 1% to 2% of the general population has a bicuspid aortic valve. It’s twice as common in men than it is in women.
People with Turner syndrome have an increased risk of heart problems, including a bicuspid aortic valve.
You might not feel any symptoms until the disease has progressed a lot or you have a medical emergency. But imaging tests can catch subtle changes before you even notice symptoms. And advances in treatment can help you live a long and healthy life.
You may not have any bicuspid aortic valve symptoms. You could live many years without even knowing your anatomy is different. But over time, you may develop symptoms of aortic regurgitation or stenosis. If your child has a bicuspid aortic valve, you may spot symptoms soon after birth (in severe cases). But it’s more likely that you won’t notice them until later. Children and infants may have pale or bluish skin (cyanosis) or trouble with feeding or gaining weight.
Bicuspid aortic valve symptoms in adults include:
Many people don’t realize they have a bicuspid aortic valve until medical tests diagnose it. That’s because symptoms are easy to miss. Your family or friends may notice a change before you do. One helpful tip is to think about how much activity you can do in a typical day. Compare it with one year ago, or even six months ago. Do you get tired more easily? Do you need more time to rest? If so, that may signal your heart is working harder to keep up.
That’s why it’s so important to keep up with your medical appointments. Talk with your healthcare provider about any changes you notice in your daily life.
Researchers don’t know what causes a bicuspid aortic valve to form. It’s the most common congenital (present at birth) heart condition. It develops early in pregnancy.
It seems to be, but researchers don’t yet fully understand the details.
A bicuspid aortic valve can run in families. If a close biological family member (parent, child or sibling) has this heart issue, talk with your healthcare provider. They may want to run some tests to check your heart anatomy and function.
If you have a bicuspid aortic valve and are planning a pregnancy, talk with your provider. You can’t prevent this problem from happening, but you can monitor your pregnancy and try to diagnose any problems early.
Without treatment, bicuspid aortic valve disease can lead to serious complications. These include:
Advertisement
A healthcare provider may diagnose a bicuspid aortic valve with a cardiac prenatal ultrasound during pregnancy. Other times, providers diagnose it when a child has other heart problems that cause symptoms. Testing then reveals the bicuspid aortic valve.
But other people go many years without knowing they have this condition. The first sign may be a heart murmur that your provider hears through a stethoscope. After that, your provider may run imaging tests to check your heart’s structure and function.
Your provider may run the following tests to check your heart and diagnose a bicuspid aortic valve:
They may also refer you for genetic testing.
Medications like beta-blockers or diuretics can help with symptoms. But they won’t fix this condition. Bicuspid aortic valve disease treatment involves surgery for about 4 out of 5 people with this problem. Your surgeon will either repair or replace your aortic valve. Your surgeon may also fix other issues (like an aneurysm) at the same time.
Your provider will evaluate your situation, run some tests and talk with you about your treatment options. Your treatment will depend on the condition of your aortic valve and aorta. But your provider will also consider your overall heart health, age and other medical conditions.
Advertisement
It’s important to have surgery early enough to prevent permanent damage to your heart. Even if you don’t have symptoms, your provider may want to fix the problem now to avoid complications down the road. The best timing is different for everyone. Your medical care team will discuss your options with you.
New technology continues to improve outcomes and reduce complications. Many people can have minimally invasive techniques instead of traditional open-heart surgery.
Traditional (open-heart) aortic valve surgery involves a 6- to 8-inch incision down the middle of your sternum (breastbone). A surgeon divides your sternum so they can access your heart directly.
Minimally invasive aortic valve surgery involves a smaller “J” incision (2 to 4 inches). The incision will be at the top of your sternum or between your ribs. Your surgeon doesn’t need to open your whole chest. This procedure reduces blood loss and allows you to leave the hospital sooner. You may also recover more quickly.
Aortic valve repair fixes your valve without replacing it. It can be a good option for aortic regurgitation (leaky valve). But it can’t treat aortic stenosis (narrowing). Surgeons can often perform an aortic valve repair through a minimally invasive surgery with the “J” incision. Your surgeon will reshape your aortic valve cusps to help them open and close more completely.
Advertisement
Aortic valve replacement involves removing your unrepairable valve and giving you a new one. Surgeons can replace your valve with traditional open surgery or the minimally invasive transcatheter aortic valve replacement (TAVR) method.
Your new valve will be biological or mechanical.
Many people prefer a biological valve so they don’t have to take blood thinners. But it depends on your age, other medical conditions and personal preferences. Your provider will discuss your options and help you decide what’s best for you.
Another option for valve replacement is the Ross procedure (switch procedure). It involves using your pulmonary valve to replace your aortic valve. This procedure can be a good option if you’re under 50 and want to avoid long-term use of blood thinners.
Generally, valve surgeries have a low risk of complications. But possible risks include:
It can take two to three months to recover completely from an aortic valve replacement. You may only need one to two months to recover from an aortic valve repair.
About 98% of people who have valve surgery survive without it affecting their life expectancy. If you have a bicuspid aortic valve, you can live just as long as someone without this condition. But you need regular follow-ups and testing with your healthcare provider. Your provider will check your valve and make sure you get treatment when needed. Treatment is essential to avoiding complications.
There’s no way to prevent a bicuspid aortic valve. It’s congenital (something you’re born with). But you can make lifestyle changes that reduce your risk of other heart problems like atherosclerosis and coronary artery disease. If you have a bicuspid aortic valve, talk with your provider about managing heart disease risk factors, including:
With a bicuspid aortic valve, you can do most of the things you love. You may need to make some lifestyle changes to help keep your heart healthy and reduce stress on your heart. These include:
You’ll need regular appointments with your provider to check your heart function. If you have valve surgery, you’ll have follow-ups after two weeks, three months and six months. You’ll then have an appointment every year. These appointments are essential for keeping you healthy and checking your valve to catch problems before they become severe.
A bicuspid aortic valve is a concern when it starts interfering with your heart function. Bicuspid aortic valve disease can cause aortic stenosis and regurgitation. Over time, these problems can lead to permanent heart damage.
Your provider will let you know how often you need to come in for appointments. If you had surgery, you’ll have several follow-ups within the first year and then one each year.
If you have a biological family history of heart valve problems but haven’t been diagnosed, your provider may refer you to a cardiologist (heart doctor). Your cardiologist can screen you for heart problems and offer guidance.
Call 911 immediately if you have symptoms of an aneurysm rupture or dissection:
If you or your child have a bicuspid aortic valve diagnosis, talk with your provider about the condition of your heart and whether you need treatment. Some questions include:
Dealing with a bicuspid aortic valve can be overwhelming and raise a lot of questions. Keep in mind that doctors and surgeons are prepared to help you or your child stay healthy and strong. If you or your child was recently diagnosed, take some time to learn more about the condition. Talk with your provider and get the information you need to help you feel like you can manage the situation. And remember that they have the technology in place to catch problems early and treat them.
You might be shocked to find out you were born with a bicuspid aortic valve. The heart experts at Cleveland Clinic are ready to help you manage this condition.

Last reviewed on 08/12/2024.
Learn more about the Health Library and our editorial process.