The aorta is a large, cane-shaped vessel that delivers oxygen-rich blood to your body. It starts in the lower-left part of the heart and passes through the chest and abdomen. Along the way, blood vessels branch off the aorta, extending to organs and supporting tissue.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
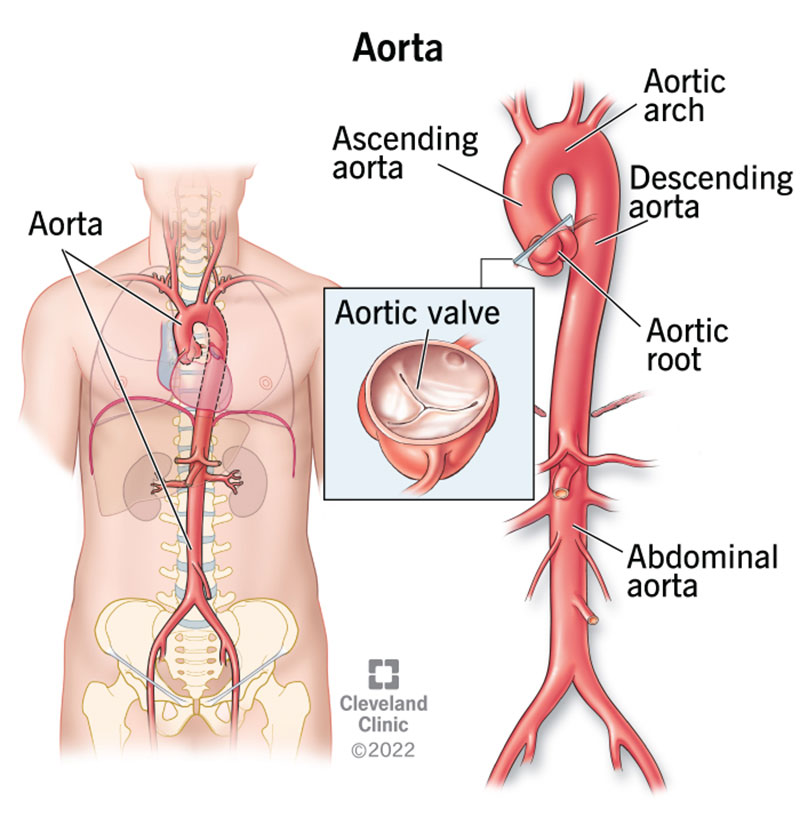
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17058-aorta-anatomy)
The aorta is a cane-shaped artery. It starts in the lower-left chamber of your heart (ventricle). From there, it extends up toward your head a short distance before curving down. The aorta passes through your chest and abdominal cavities and ends at your pelvis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pairs of smaller blood vessels branch off from various points of the aorta. These branches extend the reach of the aorta to muscles, nerves and organs throughout your body.
The aorta is the largest blood vessel in your body. It’s more than 1 foot long and an inch in diameter at its widest point. As the aorta makes its way toward your pelvis, its diameter narrows to two centimeters.
It’s a complex structure that has three layers of tissue. These include:
The aorta is the main vessel through which oxygen-rich blood travels from the heart to the rest of the body. It also delivers nutrients and hormones. The aorta’s branches ensure these substances reach internal organs and nearby supporting tissue.
Advertisement
The aorta is the primary source of oxygen and essential nutrients for many organs. If disease or injury affects blood flow through this vessel, life-threatening complications can occur in minutes.
These include:
The aorta has many sections, including the:
Many smaller blood vessels branch off from the aorta, including:
Diseases, defects and injuries can affect the aorta’s ability to do its job. These conditions include:
Diseases of the aortic valve include:
Advertisement
Some of the more common issues affecting the aorta include:
Some congenital heart diseases affect the aorta, including:
Advertisement
Additional aortic conditions, some of which are rare, include:
Advertisement
Certain aortic diseases, including aneurysms and dissections, can run in families.
Genetic conditions, especially ones affecting the connective tissue, can also lead to aortic disease. These include:
Your risk of aortic aneurysm, rupture or dissection increases with age. These issues are more likely to happen in older adults.
The risk of certain aortic diseases also increases when you have a chronic condition that damages blood vessels. These include:
Additional risk factors include:
Not always. Conditions such as small aneurysms sometimes do not worsen. Others have symptoms that come on gradually.
If aortic disease symptoms are progressing, healthcare providers may recommend preventive therapies. For example, endovascular aneurysm repair is a non-surgical procedure that reinforces blood vessels to prevent rupture or dissection. This is one of many options that protect you against complications.
Some conditions, including congenital defects, genetic diseases and trauma, are difficult to prevent. But there are steps you can take to avoid other types of aortic disease.
Prevention may include:
If you are at risk for aortic disease or healthcare providers detect a minor issue, regular monitoring can help.
Services may include imaging studies and assessments from a vascular disease specialist. Sophisticated software, along with the specialist’s expertise, helps determine the likelihood of complications. The specialist can also let you know whether preventive treatment is necessary.
Imaging studies may include:
Your aorta is a long blood vessel that’s essential to your well-being. It provides a steady supply of oxygen and nutrients to your organs. There are many conditions that can affect aorta functioning. Some can put you at risk for life-threatening complications. But having aortic disease or being at risk doesn’t always mean your health is in danger. Taking good care of yourself and seeing a specialist, when necessary, helps many people avoid complications.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you come to Cleveland Clinic for aortic disease treatment, you’ll get industry-leading care and support from our heart and vascular specialists.
