Open-heart surgery can treat heart problems like heart failure, arrhythmias, aneurysms and coronary artery disease. Open-heart surgery procedures may include CABG (bypass surgery), heart transplant, valve replacement and surgeries to fix issues present at birth.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
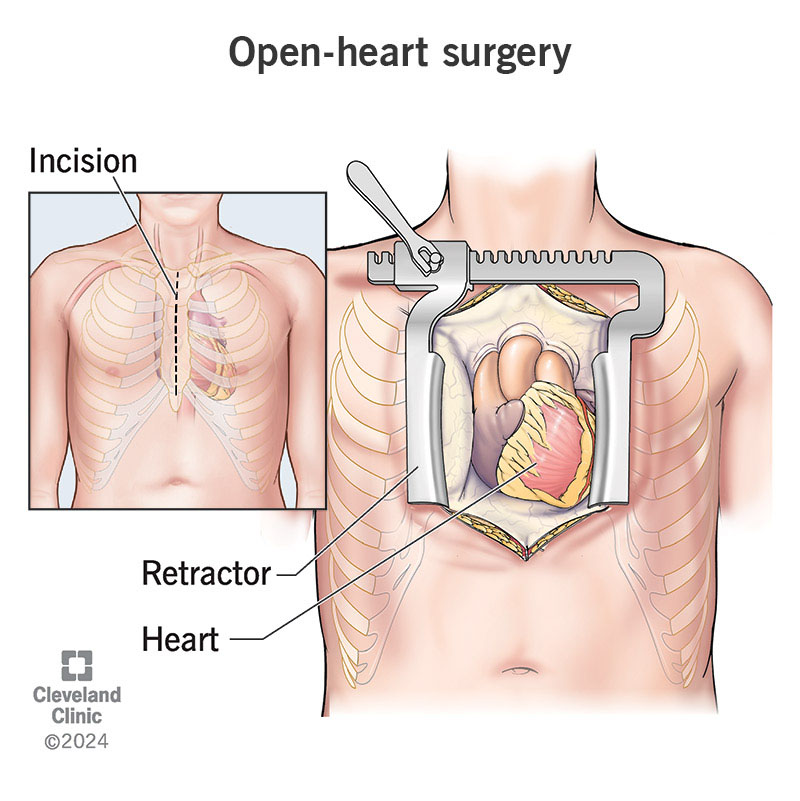
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21502-open-heart-surgery)
Open-heart surgery is a type of heart surgery that involves opening your chest wall so a surgeon can reach your heart more easily. It’s a way surgeons can reach your heart directly and treat the heart issue you have.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
To access your heart, surgeons cut through your sternum (breastbone) and spread your ribs. Sometimes, people call this cracking your chest. Your surgeon may recommend an open procedure if you’re strong enough to tolerate it.
If open-heart surgery isn’t right for you, your surgeon can do many kinds of heart surgery through smaller, less invasive incisions. This includes small incisions between the ribs on the right side of your chest.
Every year, about 2 million people worldwide have open-heart surgery.
Surgeons need direct access to your heart and surrounding blood vessels for certain procedures. Sometimes, surgeons can use less invasive techniques for these procedures. Your surgeon will assess your health to choose the best treatment approach.
These procedures may take place during open-heart surgery:
Advertisement
Sometimes, surgeons place pacemakers or implantable cardioverter defibrillators (ICDs) during open-heart surgery while performing other procedures. They may also perform ablation procedures to treat arrhythmias in the same procedure.
To prepare for open-heart surgery, you should follow your healthcare provider’s recommendations about:
Before open-heart surgery, you can expect a provider to:
There are two ways to perform open-heart surgery:
Heart surgery is complex. Surgery steps vary depending on your heart condition and the procedure you’re having. In general, your surgeon:
Advertisement
The time it takes for open-heart surgery depends on which procedure you’re having. Some surgeries may take six hours or longer. You’ll receive anesthesia and be asleep during the procedure.
Depending on the procedure, you may stay in the hospital intensive care unit (ICU) for a day or longer. When you’re ready, you’ll move to a regular hospital room.
You can expect to spend several days of recovery time in the hospital after open-heart surgery. During this time, providers may perform tests like the ones you had before surgery. They’ll want to see how well your heart is working. They’ll also encourage you to walk around your room and hallway to help you heal.
Your heart care team will explain how to care for your incision. You may have a special firm pillow to protect your chest when you cough, sneeze or get out of bed.
After surgery, you may experience:
Open-heart surgery is a traditional, reliable approach to heart surgery. It can be a life-saving operation for some. For others, open-heart surgery improves their symptoms, making it easier for them to do everyday tasks. This can give them a better quality of life.
Advertisement
Open-heart surgery risks include:
The risk of complications is greater if you have emergency surgery or if you have health issues like:
People who smoke or use tobacco products are more likely to have surgical and postsurgical issues.
You may be able to make your recovery easier by improving your health before surgery. This includes being physically active, losing weight and quitting smoking.
Usually, people don’t have long-term pain after open-heart surgery. But anxiety and depression can continue. Talk to your provider if your depression lasts more than one or two months. Rarely, people can have numbness, tingling or pain in their hands or arms from a stretched or pinched nerve. This often goes away in three to six months.
Open-heart surgery is a major surgery. It’s serious because you rely on your heart to keep blood moving through your body all the time. This is why it’s important to choose a surgeon who has a lot of experience performing open-heart surgery. Knowing that cardiac surgeons do this type of surgery regularly can provide peace of mind.
Advertisement
Open-heart surgery recovery time varies depending on the surgery type, complications and your overall health before surgery. It can take six to 12 weeks (and sometimes longer) for open-heart surgery recovery.
You’ll probably need pain medication for a few days after surgery. Some people need to take blood thinners for a few months after heart surgery to prevent blood clots. Your healthcare provider may also recommend cardiac rehab. This medically supervised program can help you regain strength and stamina and improve your overall heart health.
A couple of weeks after surgery, you’ll have a follow-up appointment with your provider. They’ll check to see how well you’re healing and how well your heart is working.
Your surgeon will let you know when you can return to work and other activities. Typically, you shouldn’t drive or lift anything heavy for the first six weeks after surgery.
You should call your healthcare provider if you experience:
Yes. Thanks to medical advances, surgeons can now use minimally invasive heart surgery or small incisions to perform many procedures that once required them to open your chest. The surgeon sometimes still needs to cut through part of your breastbone.
Depending on your situation, your surgeon may be able to use these methods:
It’s normal to have concerns before having major surgery like open-heart surgery. But your surgeon has a plan and a team of people to help them carry it out. Don’t hesitate to share questions and concerns with your healthcare provider. They want you to understand how you can prepare and make this experience the best it can be for yourself.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you need heart surgery, you want the most experienced team on your side. Cleveland Clinic offers expert cardiology care and heart surgery.
