Pulmonary hypertension is high blood pressure in your pulmonary arteries, which carry oxygen-poor blood from your heart to your lungs. The earliest symptom is shortness of breath during your usual routine. The most common causes are heart disease, lung disease and hypoxia. Early diagnosis and treatment can help you enjoy a better quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
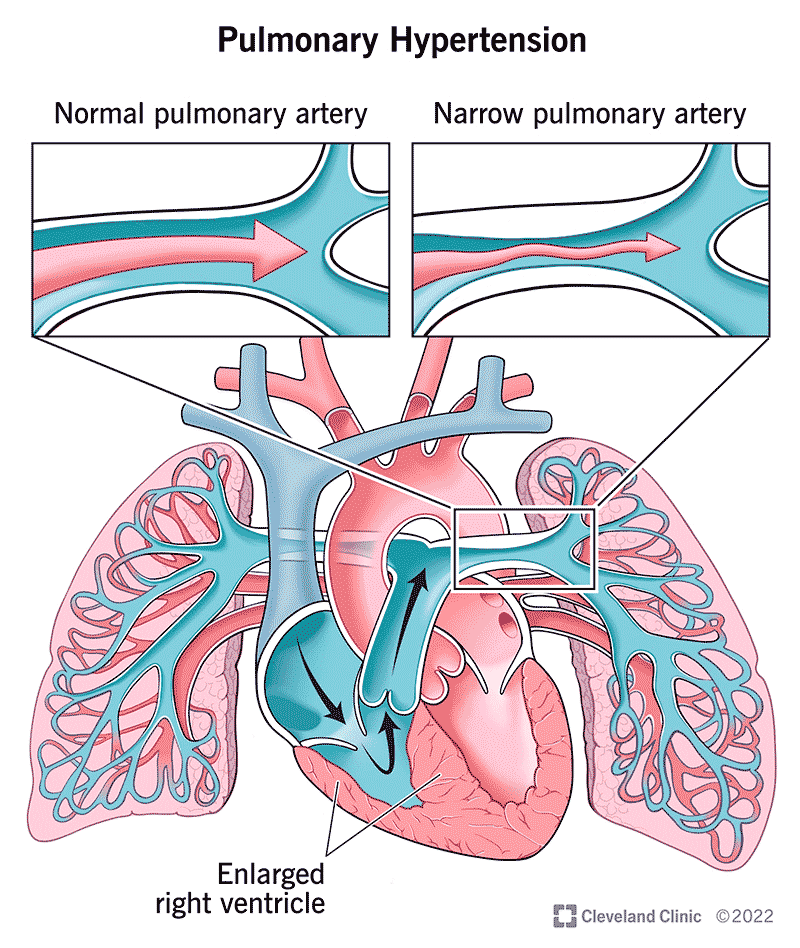
Pulmonary hypertension (PH) is a general diagnosis that means you have high blood pressure in your pulmonary arteries. These are the blood vessels that carry oxygen-poor blood from your heart to your lungs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pulmonary hypertension has many different causes. It’s usually a complication of heart disease or lung disease. But many other diseases and environmental factors can raise your risk for PH.
Pulmonary hypertension is dangerous because it disrupts the flow of blood through your heart and lungs. High blood pressure in your pulmonary arteries causes these arteries to become narrow. As a result, your heart must work harder to pump oxygen-poor blood to your lungs.
Over time, PH damages your heart and causes problems throughout your body. It can be fatal without treatment.
Pulmonary hypertension can cause serious problems in your body, including:
PH is dangerous if you're pregnant. It can cause complications for both the mother and fetus.
Without treatment, pulmonary hypertension can overtax your heart and eventually be fatal. High blood pressure in your pulmonary arteries forces your heart to work harder to send oxygen-poor blood to your lungs. Your right ventricle (lower right chamber) is responsible for pumping this blood to your lungs. So, over time, PH causes your right ventricle to get bigger due to the extra work. This condition (right ventricular hypertrophy) can lead to right-sided heart failure.
Advertisement
Right-sided heart failure has a ripple effect throughout your body. It can disrupt the normal workings of many organs and systems.
Because pulmonary hypertension can affect your entire body, it’s essential that you’re diagnosed and treated as early as possible. Your provider will prescribe treatment based on what’s causing your PH. No matter the cause, untreated PH is life-threatening.
The World Health Organization (WHO) divides pulmonary hypertension into five groups based on its cause.
Pulmonary hypertension can affect adults at any age. It commonly affects people who have heart or lung conditions. It’s also more common among people with other medical conditions. PH affects:
PH usually affects adults. But rarely, it can affect newborns. This is called persistent pulmonary hypertension of the newborn (PPHN). Infants with this condition may need treatment in the intensive care unit.
Some types of PH are rare, such as pulmonary arterial hypertension (PAH) and PH caused by blood clots. But other types are much more common, especially PH caused by heart or lung problems.
We don’t know exactly how many people around the world have pulmonary hypertension. But some estimates show PH may affect 1 in 100 people. This means 50 million to 70 million people are living with PH.
PH is even more common among older adults. Around the world, about 1 in 10 adults over age 65 have PH.
Researchers believe the number of people diagnosed with PH will rise in the next few decades.
Advertisement
The first symptom of pulmonary hypertension is shortness of breath during your daily activities. These may include climbing stairs or grocery shopping. You may also feel short of breath when you exercise.
At the start of pulmonary hypertension, you may not have any symptoms. When you do start to notice symptoms, they may be mild. But PH symptoms get worse over time, making it harder for you to do your usual activities.
As PH progresses, you’ll feel shortness of breath even when you’re not moving around. Other symptoms include:
PH symptoms make it hard for you to exercise or carry out your normal daily routine.
There are four main stages of pulmonary hypertension. The World Health Organization (WHO) calls these “functional classes.” They’re based on the symptoms you feel and refer to how well you can carry out your daily activities. As PH gets worse, the symptoms become more noticeable and more disruptive to your daily life.
Advertisement
Causes of pulmonary hypertension vary widely depending on the type of PH you have. They include a range of diseases and underlying conditions as well as environmental exposures (toxins and drugs).
There are many causes of pulmonary arterial hypertension. They include:
Some people develop PAH without any clear cause. These cases are known as “idiopathic.”
Heart problems are a common cause of pulmonary hypertension. Because the left and right sides of your heart work together, a problem with the left side also affects the right side. The right side of your heart is responsible for pumping blood into your pulmonary arteries. So, left-sided heart problems cause a chain reaction that affects the rest of your heart, your pulmonary arteries and your lungs.
Left-sided heart problems that can cause pulmonary hypertension include:
Advertisement
Lung problems are another common cause of pulmonary hypertension. Some people with left-sided heart disease also have lung disease or a lack of oxygen (hypoxia).
Lung issues that can cause pulmonary hypertension include:
This form of PH is usually caused by chronic thromboembolic pulmonary hypertension (CTEPH). CTEPH is a condition that involves blood clots and scarring in the arteries in your lungs.
A pulmonary embolism is a blood clot that travels from somewhere else in your body and gets stuck in a blood vessel in your lungs. These blood clots are often treatable, but they may leave behind scar tissue.
These scars can make it harder for blood to flow through your pulmonary arteries. As a result, the blood pressure in your pulmonary arteries goes up.
Many other conditions cause pulmonary hypertension in ways that scientists don’t yet understand. Scientists don’t know the exact mechanisms that cause these conditions to trigger PH. What they do know is that there’s an association between these conditions and PH. That means people with these conditions may face a higher risk of developing PH. Such conditions include:
Your provider will perform a physical exam and run tests to reach a pulmonary hypertension diagnosis.
First, you’ll have a physical exam to check for signs of pulmonary hypertension as well as other heart or lung issues. During this exam, your provider will:
Pulmonary hypertension can be difficult to diagnose since many signs of PH are similar to those of other conditions. So, after your physical exam, your provider may run some tests to get more information.
Your provider may also refer you to a pulmonologist or cardiologist.
Your provider may use several different tests for different purposes.
These tests measure the blood pressure in your pulmonary arteries:
These tests look for the underlying cause of pulmonary hypertension:
Your provider may also perform a six-minute walk test. This test shows how much exercise you can handle and how much oxygen is circulating in your blood as you exercise. The results indicate if your pulmonary hypertension is mild or severe.
Pulmonary hypertension treatment depends on the type of PH you have and your other medical conditions. Your healthcare team will tailor treatment to your individual needs.
Right now, only two types of PH can be treated directly:
Treatment for other types of PH involves managing the underlying medical conditions.
Treatment for pulmonary arterial hypertension (PAH) includes:
Treatment for CTEPH includes:
Treatment for PH caused by heart or lung problems focuses on managing the underlying conditions. Because so many different heart and lung conditions cause PH, treatment plans can be vastly different from person to person. Talk with your provider about what’s best for you. In general, your provider may recommend:
Treatments for PH caused by other medical conditions (WHO Group 5) are still evolving. Your provider will work with you to determine the best care plan.
A last resort option for some people with severe pulmonary hypertension is a lung transplant.
Pulmonary vasodilators are medications that treat PAH and CTEPH. They can’t be used for other types of PH, including those caused by underlying heart or lung issues.
Pulmonary vasodilators help your pulmonary arteries relax. This lowers blood pressure and eases the load on the right side of your heart.
People with PH may take a variety of other medications based on their underlying conditions.
You may be taking many different medications to treat PH and other medical conditions. It can be a lot to keep track of. Here’s some advice.
Risk factors for developing pulmonary hypertension include:
Certain medical conditions also raise your risk. These include:
Talk with your provider about your risk factors and what you can do to lower your risk.
It’s not always possible to prevent pulmonary hypertension. Some risk factors are out of your control. If you have risk factors, your provider may recommend preventive screenings to check your heart and lung function.
Doing whatever you can to prevent or manage other medical conditions can help lower your risk of pulmonary hypertension. Steps you can take include:
The outlook for people with pulmonary hypertension depends on:
The outlook for each person is different. Talk with your provider to learn more about your prognosis and how to manage your condition.
Most cases of pulmonary hypertension can’t be cured. Your provider may prescribe medications to:
Your provider may also recommend lifestyle changes.
However, surgery can cure some people with chronic thromboembolic pulmonary hypertension (CTEPH).
The life expectancy varies from person to person. It depends how quickly you’re diagnosed and what other medical conditions you have. Talk with your provider about what you can expect in your individual situation.
Pulmonary hypertension is a progressive disease. That means it gets worse over time. It progresses more quickly in some people than in others. Treatment can improve your chances of surviving pulmonary hypertension for many years.
Without treatment, pulmonary hypertension leads to right-sided heart failure and, ultimately, death. Treatment can help you live longer and give you a better quality of life.
Talk with your provider about how to manage and monitor your condition. Your provider will tell you when you need to come in for checkups and tests. Be sure to tell your provider about any new or changing symptoms.
Also, talk with your provider about:
Your provider will give you specific recommendations. One key step involves reducing your sodium intake. This means:
Other dietary changes include:
Call your provider if you’re having problems with:
Go to the emergency department or call your local emergency number if you have:
A pulmonary hypertension diagnosis can cause a range of emotions. It takes time to process the diagnosis, learn what’s going on inside your body and figure out how to move forward. Work with your provider to get the resources you need. Involve your family and friends in your lifestyle changes. Educate them on your condition. And most of all, know it’s OK to ask for help and lean on others as you adjust to your new normal.
When your child is diagnosed with pulmonary hypertension, you may have a lot of concerns and questions. Cleveland Clinic Children’s has the answers.

Last reviewed on 06/02/2022.
Learn more about the Health Library and our editorial process.