Blood clots in your leg veins can travel through your bloodstream to your lungs, leading to a sudden blockage called a pulmonary embolism (PE). This may happen if you have deep vein thrombosis or risk factors like bed rest or blood clotting disorders. Seek care immediately if you have sharp chest pain, trouble breathing or other PE symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
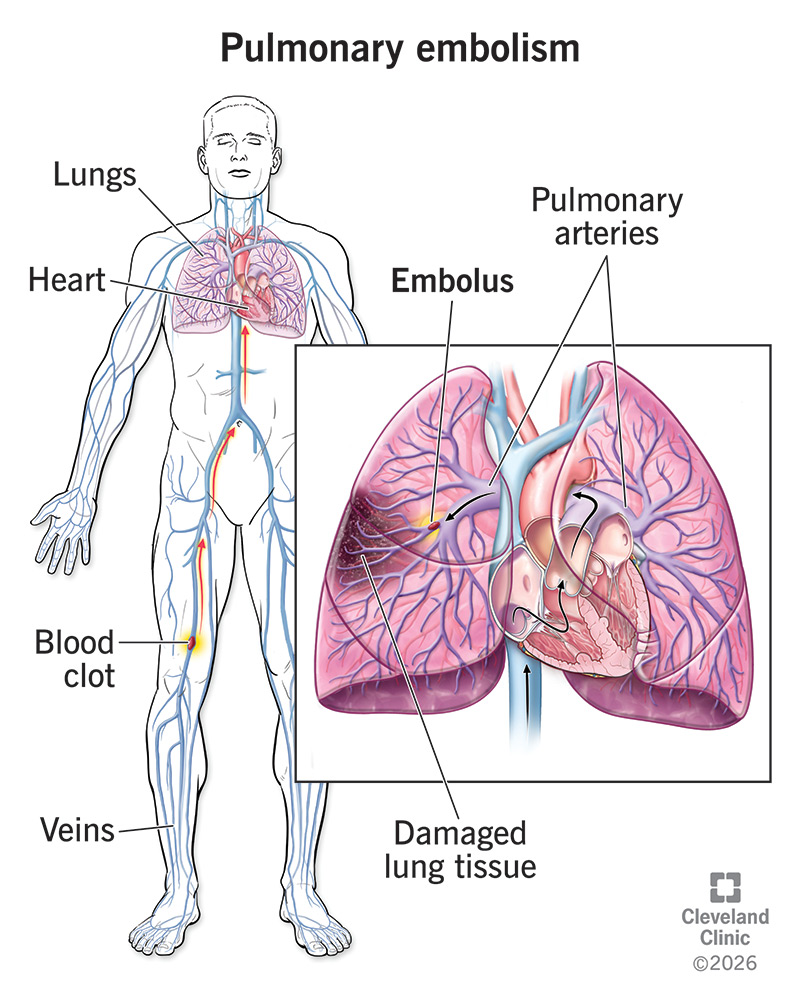
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17400-pulmonary-embolism-illustration)
A pulmonary embolism (PE) is a blood clot that travels to your lungs from somewhere else in your body and blocks blood flow. Usually, the clot starts in a vein in your leg or pelvis. It breaks free and moves through your bloodstream until it reaches your lungs, where it gets stuck in a blood vessel and obstructs the passage of blood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Pulmonary embolisms are common. Experts estimate they lead to at least 100,000 deaths per year in the U.S.
Seek medical care immediately if you think you have a PE. Quick treatment can save your life. About 1 in 3 people with a PE die within a few hours of when symptoms begin — often before they can get a diagnosis or treatment.
The most common treatment for a PE is blood thinner medication to get rid of the clot and prevent new ones from forming. In severe cases, you may have a procedure or surgery. You may need to take medication for months or years to prevent future clots. Your healthcare provider will explain the plan that’s best for you.
PE symptoms range from mild to severe and may include:
Call 911 or your local emergency number if you have these symptoms.
PE symptoms usually come on suddenly. However, symptoms of a blood clot waiting to dislodge and travel to the lungs may include leg pain, swelling and warmth. Take those signs just as seriously and seek medical care right away.
Advertisement
A pulmonary embolism happens when a blood clot travels to your lungs. In most cases, the clot starts as deep vein thrombosis (DVT). This is when you have a blood clot in a vein that’s deep inside your body, typically in your leg.
About half of all DVT or PE episodes happen after surgery or a hospital stay. These are times when you can’t move around for several days. So, blood can “pool” in your blood vessels. This makes it more likely to form abnormal clots.
Many conditions and situations raise your risk for a pulmonary embolism. What they share in common is that they make your blood more likely to clot when it shouldn’t. Examples include:
A pulmonary embolism disrupts normal blood flow through your lungs. It’s a medical emergency because it can lead to:
PE is more likely to cause death if you don’t get treatment soon enough. But it can also be fatal despite treatment.
A healthcare provider will look at your symptoms and medical history. They’ll run tests to diagnose or rule out PE, including:
You may also need other tests, like a chest X-ray or echocardiogram. These can rule out other conditions and diagnose complications.
The goal of treatment is to get rid of the blood clot in your lungs and prevent new ones. This involves medications and, in some cases, a procedure. You may need to stay in the hospital so healthcare providers can keep a close eye on your condition.
Advertisement
Possible treatments include:
Your provider will tell you when to come back for follow-up visits. These are crucial for making sure the treatment is working and that you don’t have more blood clots.
Seek medical care right away if you have any signs of internal bleeding (a risk of taking blood thinners). These include:
Advertisement
Treatment doesn’t stop when you leave the hospital. You’ll need to take blood thinners for at least three months. Some people need to take them for many months or years to prevent another PE. Your healthcare provider will tell you what’s best based on your risk factors and overall health.
A pulmonary embolism is a major life event. Recovery can take a while. Even after treatment, it’s possible to develop long-term issues like:
It’s important to tell your healthcare provider about any new or changing symptoms as you recover.
It’s hard to say how long you might live after a pulmonary embolism. Research shows that about 1 in 20 people die within 30 days of a PE diagnosis. About 4 in 20 people die within six months. Survival at one year varies greatly based on what caused the PE.
Advertisement
Remember, these numbers don’t predict your future. They simply show how serious a pulmonary embolism can be. Your healthcare provider will give you the most accurate sense of what to expect. Following your treatment plan and going to all of your follow-up visits gives you the best possible chance of surviving and regaining your strength.
It’s not always possible to prevent PE. But there’s a lot you can do to lower your risk:
A pulmonary embolism (PE) can be a scary and life-changing event. Even after successful treatment, you might worry you’ll have another one. Others may not understand what you’re going through — and you might be tired of explaining it. You might miss how things were before. Connecting with a support group or counselor can help you make sense of all these feelings and find a path forward.
As you recover, stay in contact with your healthcare provider. Follow the treatment plan they give you. It might feel like there’s a lot that’s out of your control. But each time you take your medicine or go to a check-up, you’re doing something to protect your health. You’re not powerless, and you’re not alone.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A blood clot in your lungs is serious. But Cleveland Clinic has the expert pulmonary embolism treatment you need.
