Tetralogy of Fallot is a congenital heart condition, which means it’s present at birth. ToF makes it hard to get enough oxygen to your body because of four issues in your heart’s structure. Surgery in infancy repairs the problems and helps blood flow better, but you’ll need lifelong follow-ups with a provider.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
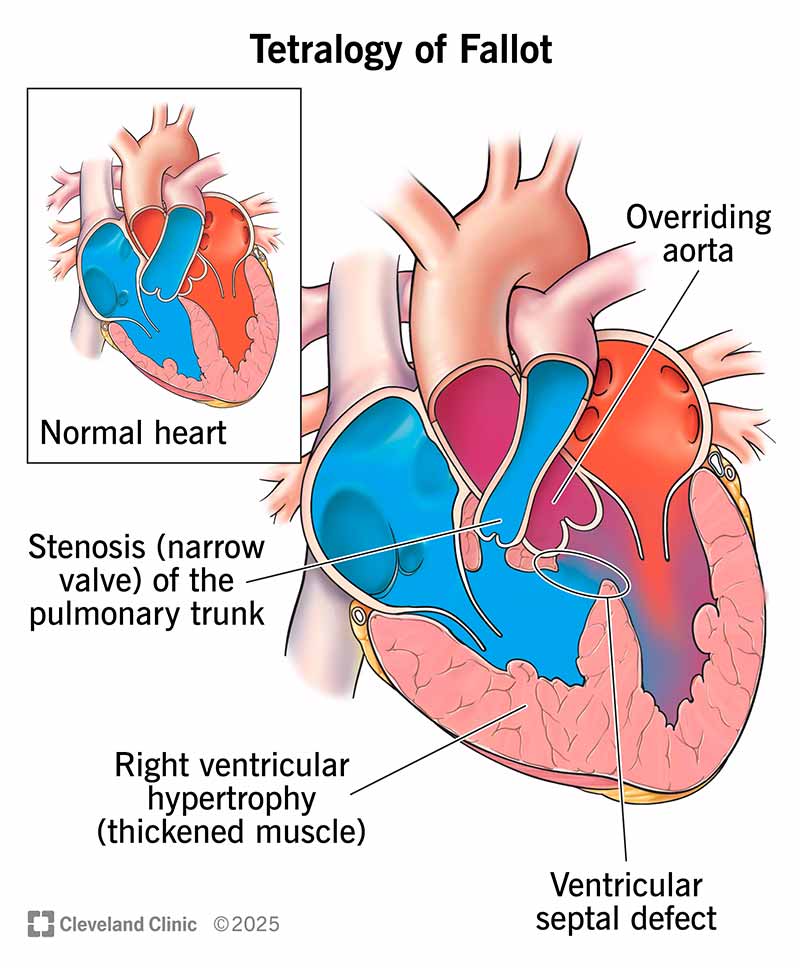
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22343-tetralogy-of-fallot-illustration)
Tetralogy of Fallot (ToF) is a condition in which a baby has four abnormalities in their heart at birth. These issues make it hard for your baby’s heart to send enough oxygen to their entire body. This matters because your body needs oxygen to function.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Normally, your blood travels a specific route through your heart with every heartbeat. Because of the structural problems in a heart with ToF, some blood that doesn’t have oxygen in it can go out to your baby’s body. Medicines and procedures can help your child get relief during infancy.
Babies have these four issues with tetralogy of Fallot:
This condition is rare. One out of 2,077 babies born in the U.S. each year has tetralogy of Fallot. But it’s one of the more common congenital heart disorders. Tetralogy of Fallot tends to happen more often in male babies. Healthcare providers also see ToF often in babies who have Down syndrome or other chromosome disorders.
Advertisement
Rarely, some people don’t get treatment in childhood and may develop issues in adulthood.
ToF symptoms can be mild, moderate or severe. They usually get worse over time without treatment.
Tetralogy of Fallot symptoms in children include:
If you didn’t get a diagnosis as a child, you may develop ToF symptoms as an adult. A lack of oxygen may give your skin a bluish tint (cyanosis). It also can make you likely to faint or have an inability to exercise (exercise intolerance). Some adults with tetralogy of Fallot experience chest pain or heart palpitations.
Babies who haven’t gotten treatment for tetralogy of Fallot can get “tet spells.” This happens when their oxygen level drops without warning while or after feeding, crying or pooping. Tet spells can be as short as a few minutes to as long as several hours. Your baby may sleep a lot after a tet spell.
Signs of a tet spell include:
Healthcare providers aren’t sure what causes tetralogy of Fallot.
Something in your child’s DNA may have changed, and that change rarely comes from a biological parent. A parent who’s had a heart abnormality since birth doesn’t normally pass it to their child. But the risk may be higher if both parents have the heart issue.
Risk factors in the expectant mother that increase risk for tetralogy of Fallot in the baby may include:
Although healthcare providers don’t know the cause of tetralogy of Fallot, you may be able to reduce a fetus’s risk of ToF in these ways:
Without tetralogy of Fallot surgery, symptoms usually get worse. Also, other health issues can happen with a ToF heart defect, like:
Advertisement
Your healthcare provider can diagnose tetralogy of Fallot during pregnancy or after your baby is born. They usually find ToF in the first few weeks or months of life. During prenatal tests, your healthcare provider may use a fetal echocardiogram to look at the fetal heart’s structure if the initial ultrasound looks suspicious.
During a physical exam, a healthcare provider will listen to your child’s heart. If they have ToF, their provider will most likely hear a heart murmur.
Tests a provider may use to diagnose tetralogy of Fallot may include:
Tetralogy of Fallot treatment includes medicine to ease symptoms and surgery to fix the issues. As a first step in tetralogy of Fallot treatment, your child’s provider can give them beta-blockers (to improve blood flow) and extra oxygen. Three to six months after birth, your baby can have surgery to make blood move through their heart the way it should.
Repair options vary depending on your child’s condition. If your baby is too small or weak for a full repair, their provider can do a simpler procedure until they can do the complete ToF repair. These techniques can relieve symptoms for a number of years — well into adulthood — until a provider can do a more complete repair surgery.
Advertisement
Tetralogy of Fallot repair procedures include:
Occasionally, a person reaches adulthood without having had any surgical repair. This isn’t common. Specialists recommend they have a complete surgical repair to prevent future complications or sudden death.
To perform a complete repair, a surgeon who specializes in adult congenital heart disease closes the ventricular septal defect with a patch. They open the passageway out of the right ventricle and repair or replace the pulmonary valve. They enlarge the pulmonary arteries to both lungs. Sometimes, they place a tube between the right ventricle and the pulmonary artery to improve blood flow.
Many adults who undergo repair for a ToF heart defect don’t need further surgical treatment. But they should continue to follow up with an adult congenital heart disease specialist for regular monitoring.
Advertisement
Complications of tetralogy of Fallot surgery (some of which may show up later) may include:
Surgery for tetralogy of Fallot creates a normal blood flow path. But you or your child can still have other issues, including:
With medical advances, the outlook for babies with tetralogy of Fallot is better than it was in the past. Surgical treatment is very effective in correcting structural defects and blood flow through the heart. With an experienced congenital heart disease surgeon, surgical repair of the defect in adults has a very high success rate.
Most babies who have surgery today to fix tetralogy of Fallot will have active lives. But people with repaired ToF typically have some restrictions on certain strenuous activities, like competitive sports. Long-term survival after ToF repair is very good. Most people who undergo repair are alive 30 years later. Without a repair, 1 out of 3 people with tetralogy of Fallot live to age 10.
Some adults who had tetralogy of Fallot surgery as infants may develop issues that require medicines, medical care or surgery in adulthood. Adults should consult with their cardiologist before having surgery on a different part of their body.
Until your baby has surgery, you can help them through tet spells. When your baby has trouble breathing, put them into a squatting position. (Push their knees to their chest.) Squatting helps move more blood to their lungs.
It’s also helpful to make sure your child is drinking enough fluids and isn’t exerting themselves too much.
If your baby is having a severe tet spell, take them to the closest emergency room. If you’ve passed out, are dizzy, are short of breath or have chest pain, you should also go to the emergency room.
Adults who’ve had initial surgery for ToF as a child should have thorough cardiac evaluations every year or two. You may need various tests to check cardiac function, like:
Also, your provider will need to monitor the size and function of the right side of your heart.
After tetralogy of Fallot repair, your child will need regular visits with a provider who specializes in children’s hearts (pediatric cardiologist). Regular care will continue into adulthood.
Questions to ask your provider include:
Learning that your newborn child has a heart problem can feel like a heavy weight to bear. But your healthcare team has helped other parents in this situation and they can help you, too. Don’t be afraid to talk to a therapist if you feel stressed about caring for a child with tetralogy of Fallot. A counselor can also help kids and teens who may feel like their classmates are ahead of them in development.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Your baby needs lifelong care for congenital heart disorders like tetralogy of Fallot. Cleveland Clinic Children's compassionate providers offer personalized treatment.
