Hemolytic uremic syndrome (HUS) is a condition that damages blood vessels in your kidneys. E. coli infection is the most common cause of HUS. In most cases, symptoms include diarrhea, abdominal pain, high blood pressure and peeing less than usual. Treatment includes transfusions and medications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
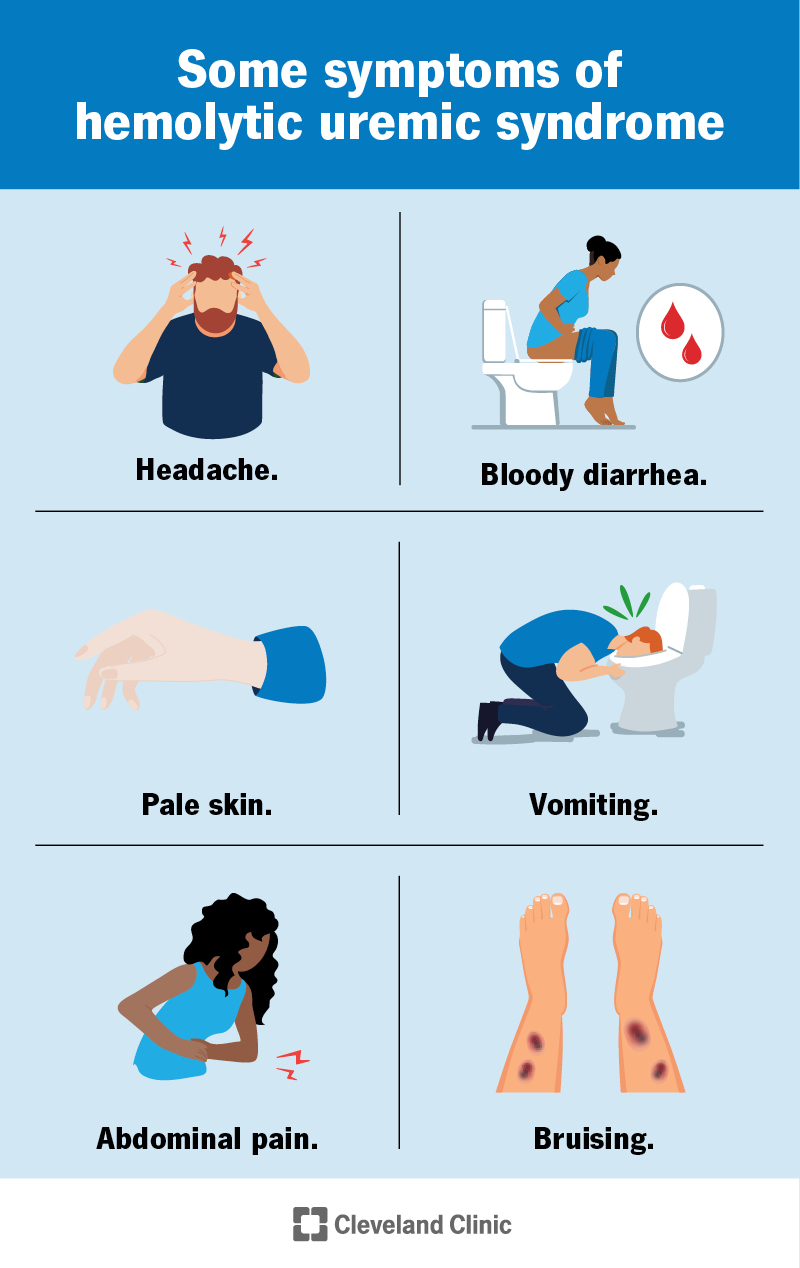
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/hemolytic-uremic-syndrome)
Hemolytic uremic syndrome (hee-mah-lit-ick yer-ee-mik sin-drohm) is a condition that blocks the small blood vessels in your kidneys. The blockage destroys your red blood cells (hemolytic anemia) and reduces the number of platelets (thrombocytopenia) in your blood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Hemolytic uremic syndrome (HUS) can affect anyone. But you’re more likely to get it from a bacterial infection that causes loose poop (diarrhea), especially Escherichia coli (E. coli). However, a syndrome is a group of symptoms that may have different causes. So,even though you’re more likely to get HUS from E. coli, you could get it from something else.
HUS can affect other organs in your body, including your heart and brain. But it most commonly affects your kidneys.
Contact a healthcare provider if you have bloody diarrhea or diarrhea that lasts longer than three days. Without treatment, a severe case of HUS can be deadly.
Types of hemolytic uremic syndrome include:
Atypical hemolytic uremic syndrome (aHUS) is a rare type of HUS. Common symptoms include:
Advertisement
Atypical hemolytic uremic syndrome is usually a genetic disorder. That means biological parents pass it down to their children. Genetic mutations in some of your genes that encode proteins can cause aHUS. An illness, infection or an environmental factor triggers the mutation to activate.
Hemolytic uremic syndrome affects between 5% and 15% of people who have E. coli diarrhea. aHUS is very rare, occurring in less than 1 person in 1 million people.
The most common symptoms of hemolytic uremic syndrome include:
Other common symptoms may include:
In severe cases of HUS, damaged red blood cells can cause blood clots that damage your organs, especially your kidneys. This affects how well your kidneys can filter and eliminate waste from your body. If your kidneys can’t filter and eliminate waste, it can lead to acute kidney injury (AKI). AKI symptoms include:
Certain strains of the bacteria E. coli cause most cases of hemolytic uremic syndrome. These strains produce the toxin Shiga. Shiga damages the lining of your small intestine and causes diarrhea. It can also enter your bloodstream, destroy red blood cells and damage your kidneys. You’re more likely to get an E. coli infection when you eat spoiled, undercooked or poorly processed foods or drinks, such as:
Another name for these strains is Shiga toxin-producing E. coli (STEC). The most common STEC in North America is E. coli O157:H7, or E. coli O157.
In rare cases, certain medications and substances may cause secondary HUS as a side effect. These may include:
Advertisement
No, hemolytic uremic syndrome isn’t contagious. You can’t get HUS from person-to-person contact.
But E. coli is contagious. You can get it after consuming contaminated foods or drinks or coming into contact with a contaminated person’s or animal’s poop.
Anyone can develop HUS. But you’re more likely to develop it if you:
A healthcare provider will diagnose hemolytic uremic syndrome by:
If they suspect you have HUS, they’ll also order tests.
A healthcare provider may order the following tests to diagnose hemolytic uremic syndrome:
Advertisement
Tests look for the presence of different things that indicate hemolytic uremic syndrome:
You must get hemolytic uremic syndrome treatment at a hospital. Treatment may include:
Advertisement
If you have severe kidney damage, you may need dialysis to clean your blood while your kidneys heal. If HUS causes kidney failure, you may need a kidney transplant.
Yes, you can recover from hemolytic uremic syndrome without permanent damage to your health.
About 20% to 50% of children have mild chronic kidney disease (CKD) and 3% to 5% develop kidney failure (end-stage kidney disease). In adults, research estimates about 45% had CKD.
More than 85% of people with HUS recover complete kidney function. But, even if you make a full recovery, you may have high blood pressure or other kidney problems in the future.
With proper diagnosis and care, many people with HUS make a full recovery without any permanent damage to their health. But you have an increased chance of developing high blood pressure or other conditions that may affect your kidneys in the future.
Severe cases of HUS can be fatal without treatment, especially if HUS affects other organs like your brain.
With proper diagnosis and treatment, more than 90% of people survive hemolytic uremic syndrome.
You can help prevent an E. coli infection that causes hemolytic uremic syndrome by:
If you or your child has severe diarrhea, it’s important to try to rehydrate. Rehydration drinks help replace lost electrolytes. Babies and younger children may need breast (chest) milk or formula to rehydrate. Call a healthcare provider to help you determine the best way to keep your child hydrated
Contact a healthcare provider if you have:
Questions you may want to ask a healthcare provider include:
A triad is a group of three signs that indicate a medical condition.
The hemolytic uremic syndrome triad includes:
If you have diarrhea, it doesn’t mean you have hemolytic uremic syndrome. But see a healthcare provider if you have bloody diarrhea or severe diarrhea in which you can’t stay hydrated or it lasts longer than three days.
Hemolytic uremic syndrome and thrombotic thrombocytopenic purpura (TTP) are similar disorders — TTP also causes blood clots to form in your small blood vessels. Previously, healthcare providers grouped HUS and TTP together. But they now recognize them as separate conditions.
Diarrhea is usually a short-term, but uncomfortable and annoying, condition that gets better after a day or two. But if you have bloody diarrhea or diarrhea that lasts for longer than three days and you feel tired, look pale and don’t pee a lot when you use the bathroom, it’s time to see a healthcare provider. Hemolytic uremic syndrome can severely damage your kidneys and affect other organs. The sooner you treat it, the less risk you have of developing lasting harm to your kidneys.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have a condition that’s affecting your kidneys, you want experts by your side. At Cleveland Clinic, we’ll work with you to craft a personalized treatment plan.
