Tube feeding (enteral nutrition) delivers liquid nutrition through a flexible tube that goes in through your nose or directly into your stomach or small intestine. You may need a feeding tube if you can’t chew or swallow. Your healthcare provider will teach you how to care for your feeding tube before you leave the hospital.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
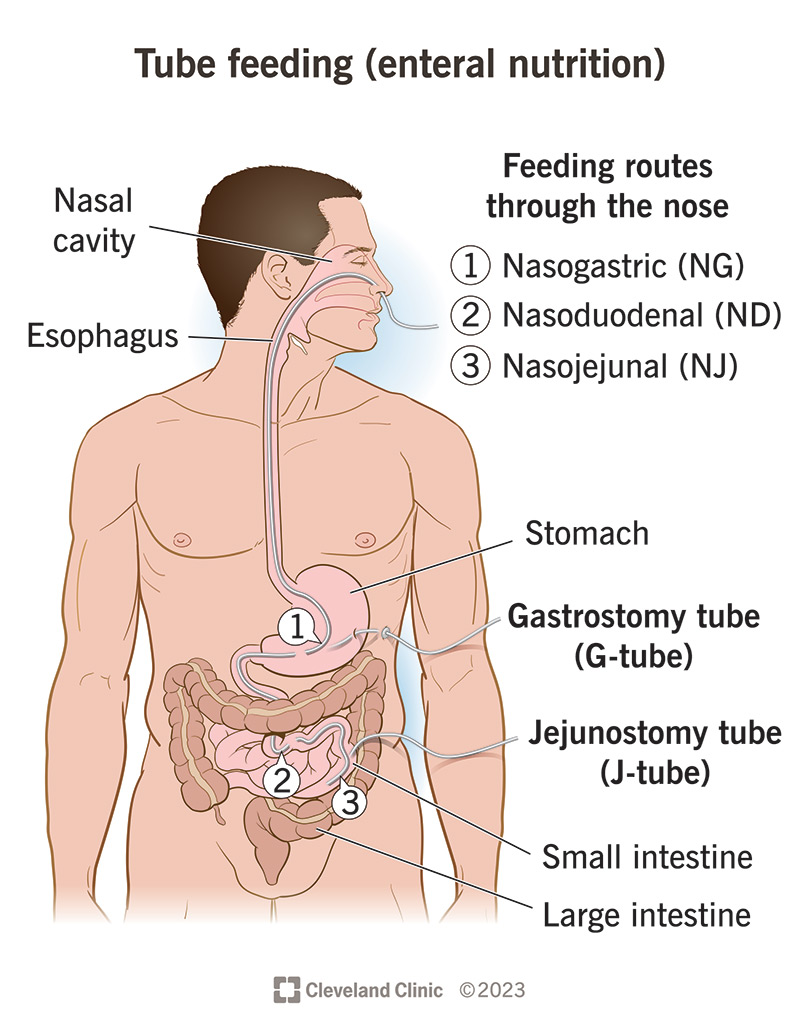
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/21098-tube-feeding-enteral-nutrition.jpg)
Tube feeding (enteral nutrition) uses a feeding tube to supply nutrients and fluids to your body if you can’t safely chew or swallow. Feeding tubes are soft, flexible plastic tubes through which liquid nutrition travels through your gastrointestinal (GI) tract. Healthcare providers also sometimes administer medicines through feeding tubes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Think of a feeding tube as providing added access to your digestive system. If you have a condition that prevents food from traveling the traditional route through your GI tract — from mouth to esophagus (food tube) to stomach to small intestine — a feeding tube can help. Depending on where the tube ends, it delivers nutrition directly to your stomach (which stores and digests food) or small intestine (which absorbs nutrients).
Healthcare providers usually recommend feeding tubes that go in through your nose and down into your stomach or small intestine if you’ll need one for less than four to six weeks. Or, they may recommend a tube that goes in through your nose to see if your body can tolerate the feeding tube formulas. Types include:
Healthcare providers may recommend a more semi-permanent placement of tubes through your abdominal wall to access your stomach or small intestine directly. This is usually if you’ll need tube feeding longer than four to six weeks. Types include:
Advertisement
Your healthcare provider may recommend enteral nutrition if you aren’t getting the nutrition you need by mouth. You may need enteral nutrition if you have limited ability to chew or swallow (dysphagia).
Feeding tubes help support your metabolism and your overall digestive health.
Conditions that may cause you to need a feeding tube include:
Healthcare providers sometimes recommend tube feeding as a part of hospice care to help people at the end of life stay more comfortable. Some people (or their families) decide against tube feeding. In this instance, tube feeding is a highly personal decision that you should discuss with your healthcare provider.
Your experience will depend on the type of feeding tube you get and why you need it. Your care team may take total responsibility for feedings and cleaning your feeding tube while you’re in the hospital. If you go home with it, you (or your caregivers) may need training on how to use and care for it. You may also need help setting up the equipment to use the tube at home.
Healthcare providers usually insert feeding tubes while you’re in the hospital, but you may continue to use one at home. Tube feeding provided at home is called home enteral nutrition (HEN).
Some placement procedures can happen at your bedside. But if you’ll need a feeding tube for more than a month or so, you’ll need an in-hospital procedure to insert the tube. For these procedures, plan to fast (no eating or drinking) for at least eight hours. You’ll also need to stop blood-thinning medications (anticoagulants), like aspirin, for a while before the procedure. You’ll receive anesthesia and sedation, so you won’t feel pain. Procedures usually take half an hour.
Advertisement
Healthcare providers may insert the tube:
Advertisement
Ask your healthcare provider about the method they’ll use to insert the feeding tube, so you know how to prepare and what to expect.
Some feeding tubes use a syringe or pump to send liquid nutrition from a bag into your body. Other feeding tubes connect to bags that are raised on a pole or hook. Gravity sends the liquid nutrition down through the tube when it’s time to eat.
When you eat depends on various factors, including the type of feeding tube you have. Tube feedings may be:
Your healthcare provider will help you determine the type of formula and how much you need to ensure you’re getting the right amounts of fluids, vitamins, minerals and calories.
Advertisement
Many formulas are available with different concentrations of calories and specific nutrients, like proteins, fats and carbohydrates. Some formulas are specific for certain diseases, such as kidney diseases. Your provider may change the formula based on your tolerance and nutrition needs over time.
They can also advise you on how to receive enteral nutrition safely. For example, they may advise you to sit at a 45-degree angle during feedings and a few hours afterward to prevent complications, like aspiration pneumonia. With aspiration pneumonia, the formula slips into your windpipe and lungs, causing an infection. The way you position your body can prevent this.
Never insert any carbonated beverages into your feeding tube.
You’ll need to care for the feeding tube to prevent clogs and clean the skin around the feeding tube to prevent infections.
To care for the insertion site:
To care for the tube:
After surgery to insert a tube, your belly may feel sore for a few days. You may notice drainage for a day or two. This is normal. It’s also common to experience certain side effects at first, like diarrhea, as your body adjusts to receiving nutrition in new ways.
Your provider can prescribe medications that can help with the pain. They can adjust your formula or feeding frequency to go easy on your digestive system as it adjusts.
Other issues can happen, but the risk of complications is small. Complications include:
How long you’ll need a feeding tube varies from person to person. Depending on the reason for the tube, you may use a feeding tube for a few weeks, several months or years. You may need a feeding tube long-term form to receive nutrition, medication or hydration (water).
It’s important to care for your feeding tube as your provider instructs and keep your insertion site clean. If you have pain, redness, swelling or excessive leaking or itching, call your provider immediately.
If your tube is clogged, you can try gently flushing it with warm water. If that doesn’t work, call your provider.
Never attempt to loosen a clog by inserting wires into the tube.
If the tube comes out, get to an ER right away.
Tube feeding doesn’t provide the same satisfaction that goes along with tasting delicious foods. But the work it does is vital. Tube feeding provides your body with the nutrition it wouldn’t otherwise get if you were relying on chewing and swallowing alone. This nutrition can buy you time as your body heals and regains strength. It may become a necessary part of your survival if you have a condition that keeps you from eating without a feeding tube. Your healthcare provider can walk you through what to expect if you need one, including how to adjust to one briefly or for longer.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
If you have issues with your digestive system, you need a team of experts you can trust. Our gastroenterology specialists at Cleveland Clinic can help.
