Thrombocytopenia occurs when your bone marrow doesn’t make enough platelets. Platelets are blood cells that form blood clots to help stop bleeding. People with this condition may bleed a lot and the bleeding may be hard to stop. Thrombocytopenia affects people with certain medical conditions like autoimmune disease or who take certain medications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
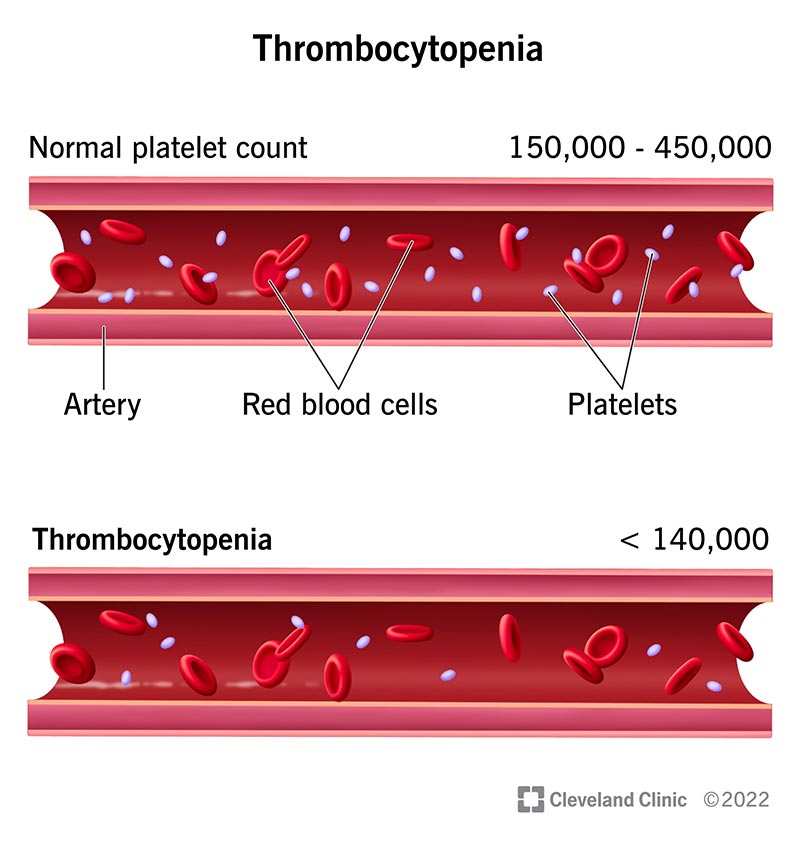
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/14430-thrombocytopenia)
Thrombocytopenia (pronounced “THROM-bo-sigh-toe-PEE-ne-ah”) occurs when your bone marrow doesn’t make enough platelets. Platelets are blood cells that form blood clots to help stop bleeding. If you have thrombocytopenia, you may bleed a lot, and the bleeding may be hard to stop.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Thrombocytopenia often affects people with certain medical conditions, like autoimmune disease or who take certain medications. Healthcare providers typically treat thrombocytopenia by treating the underlying condition and/or changing the medication that caused the issue.
People may have thrombocytopenia and not realize it because their symptoms are so mild. That’s why healthcare providers aren’t sure exactly how many people have this condition. They do know a related condition, immune thrombocytopenia, affects 3 to 4 in 100,000 children and adults. About 5% of pregnant women develop mild thrombocytopenia just before giving birth.
People with severe thrombocytopenia may have an increased risk of developing the following conditions:
What are normal platelet levels?
A normal platelet count or level in adults ranges from 150,000 to 450,000 platelets per microliter of blood. Thrombocytopenia levels are:
Advertisement
Some people with mild cases of thrombocytopenia don’t have symptoms. When they do, one of the first symptoms is a cut or nosebleed that won’t stop bleeding. Other symptoms include:
Thrombocytopenia causes fall into one of three categories:
Specific factors affecting platelet supply include:
Advertisement
Healthcare providers will do a physical examination. They’ll check for bruises, rashes and other thrombocytopenia symptoms. They’ll ask about your medical history, including any medications you take. They may do tests including:
You might not need treatment if a low platelet count isn’t causing significant issues. Often, healthcare providers can improve platelet counts by treating the underlying cause. This approach may involve changing your medications. Other treatments include:
Advertisement
Many things can cause your platelet levels to drop so you develop thrombocytopenia. For example, you may have an autoimmune disease that affects your platelet levels. You may have low platelet levels because you drink lots of alcohol or are exposed to certain toxic chemicals.
Bottom line — once your healthcare provider finds out why your platelet levels are low, they’ll take steps to help you. If you have thrombocytopenia, ask your healthcare provider what caused the issue and what treatment or lifestyle changes they recommend.
If your provider recommends treatment, you may need ongoing treatment to maintain a normal platelet level. Your provider will monitor your overall health and platelet levels.
The most important thing is to understand if you have medical conditions or take medication that increases your risk of developing thrombocytopenia. If you do, ask your healthcare provider if there are medications or activities you should avoid.
If you have thrombocytopenia, here are some suggested ways to take care of yourself:
Advertisement
Thrombocytopenia symptoms can develop very quickly or over time. It may also cause bleeding in many parts of your body. Seek medical care if:
You may want to ask your healthcare provider:
Thrombocytopenia — low platelet levels — may increase your risk of issues like excessive bleeding and bruising. Severe thrombocytopenia increases your risk of internal bleeding or heart attack. If you have this condition, it’s important to understand why you have low platelet levels. Your healthcare provider can explain what’s causing the low platelet count and discuss treatment options. They’ll also discuss lifestyle changes that may boost your platelet levels.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you hear a rare diagnosis like bone marrow failure and cytopenias, you want the best possible care. At Cleveland Clinic we’re experts in these rare conditions.
