Malaria is a potentially life-threatening illness caused by parasites. You get it through the bite of an infected mosquito. It’s most common in parts of the world that are hot and humid, like Africa and parts of Asia. It can cause flu-like symptoms that can progress to severe illness if not treated.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
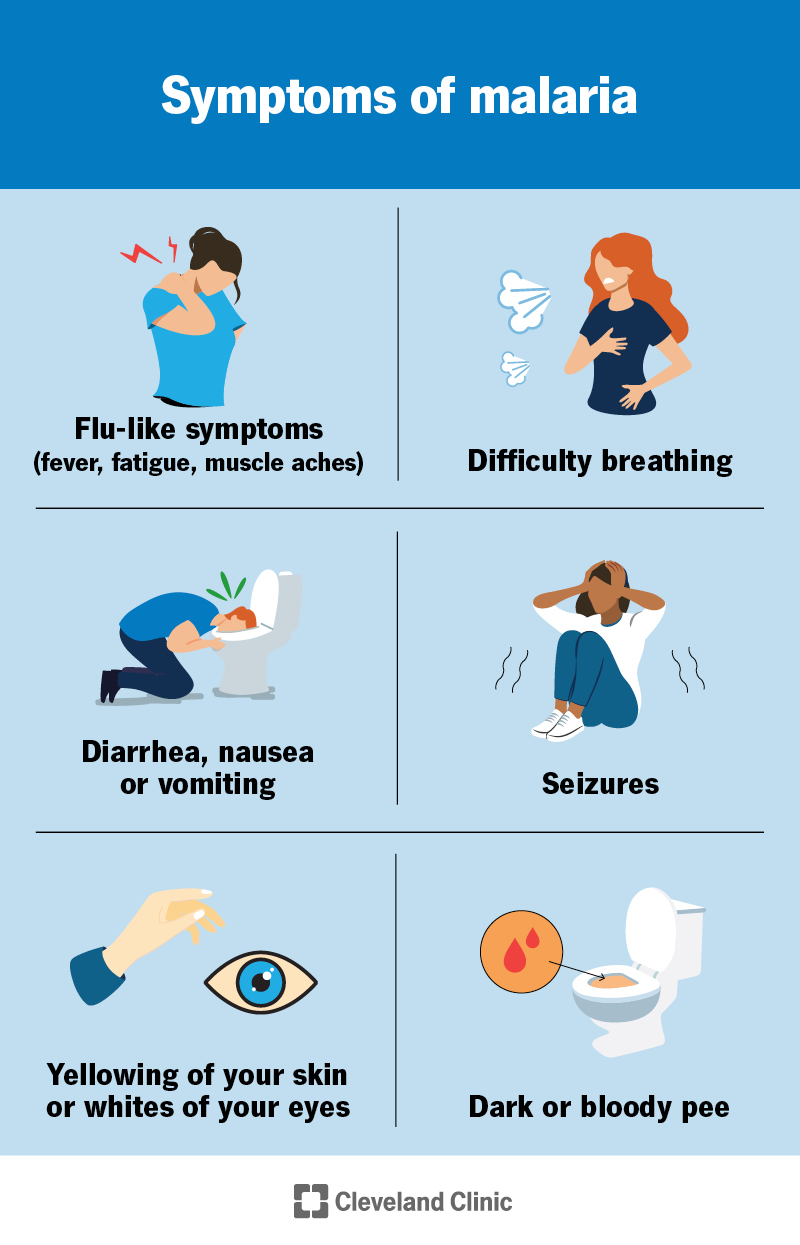
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/malaria)
Malaria is a disease you get from being bitten by a mosquito. Some mosquitoes carry tiny parasites. They can infect you with the parasites when they bite you. Malaria can cause severe illness and death if left untreated. Kids under 5 are more likely to get life-threatening illness. Malaria is most common in tropical areas where it’s hot and humid. Most cases happen in Africa. It’s rare in the U.S. See a healthcare provider right away if you live in or have traveled to an area where malaria spreads and you have symptoms. This is true even if you’ve taken medications to prevent malaria during your trip.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Symptoms of malaria can be mild to severe. They often start as flu-like symptoms and can get worse. They include:
Malaria symptoms usually appear several days to a month after you’re infected. Some people don’t feel sick for a year or longer after the mosquito bite.
Plasmodium parasites cause malaria. There are five types that can infect humans. Plasmodium falciparum (P. falciparum) and Plasmodium vivax (P. vivax) are the most common. P. falciparum often causes severe illness.
A mosquito gets the parasitic infection when it bites someone who’s infected. The mosquito then bites you and spreads the infection. The parasite multiplies in your liver and spreads to your bloodstream. There, it can spread to other people if a mosquito bites you. Rarely, malaria can also spread through:
You’re at a higher risk of getting malaria if you live in or travel to areas where it spreads, like parts of Africa. You’re at a higher risk of serious illness and death if you:
Advertisement
Malaria is most common in areas with warm temperatures and high humidity, including:
If left untreated, malaria can cause severe complications. These include:
These complications can be fatal.
Healthcare providers test a sample of your blood to diagnose malaria. They’ll look for Plasmodium parasites and identify what type of infection you have. Your provider will use this information to determine the right treatment. It’s important to tell your provider if you’ve traveled within the past year so they know to test for malaria.
Healthcare providers treat malaria with medications that kill the parasite (antimalarial medications). The type of antimalarial medication your provider treats you with depends on:
Medications can cure malaria, but it’s important to start treating it as soon as possible.
Antimalarial medications kill the Plasmodium parasites. You might receive them in an IV or take them by mouth. They include:
You might receive one or a combination of these. Take all medications as prescribed, even if you start to feel better.
See a healthcare provider right away if you’ve traveled to or live in a country where malaria is common and you have symptoms. Early diagnosis gives you the best chance for a full recovery.
Antimalarial medications can cure malaria, especially if started early. You might need to stay at the hospital, at least to start your treatment. Treatment can last for about two weeks, but you might start feeling better in a few days. Let your provider know if you aren’t feeling better or if your symptoms get worse. Sometimes, even after treatment, malaria infections can come back (recur). This happens when the parasite isn’t completely killed by treatment. It can stay in your body without causing symptoms. You can start having symptoms again years after your initial infection and treatment. Medications like primaquine and tafenoquine make this less likely to happen. You can get malaria again, even if you’ve had it before.
Advertisement
There are a few ways to reduce your risk of getting and spreading malaria:
Malaria is a serious illness. But you can take steps to prevent it, and with early treatment, you can make a full recovery. It’s important to protect yourself from mosquito bites, especially if you’re traveling where malaria is common. Talk to your provider several weeks before traveling to see if they recommend antimalarial medications. This is especially important if you’re pregnant or traveling with young children. Let your provider know right away if you’ve traveled to an area where malaria is common and you have symptoms.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a virus, fungus or bacteria? Some of these “bugs” won’t go away on their own. Cleveland Clinic’s infectious disease experts are here to help.
