E. coli is a group of bacteria that can cause infections in your gut (GI tract), urinary tract and other parts of your body. Most of the time, it can live in your gut without hurting you. But some strains can make you sick with watery diarrhea, vomiting and a fever. Shiga toxin-producing E. coli (STEC) is most likely to cause severe illness.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
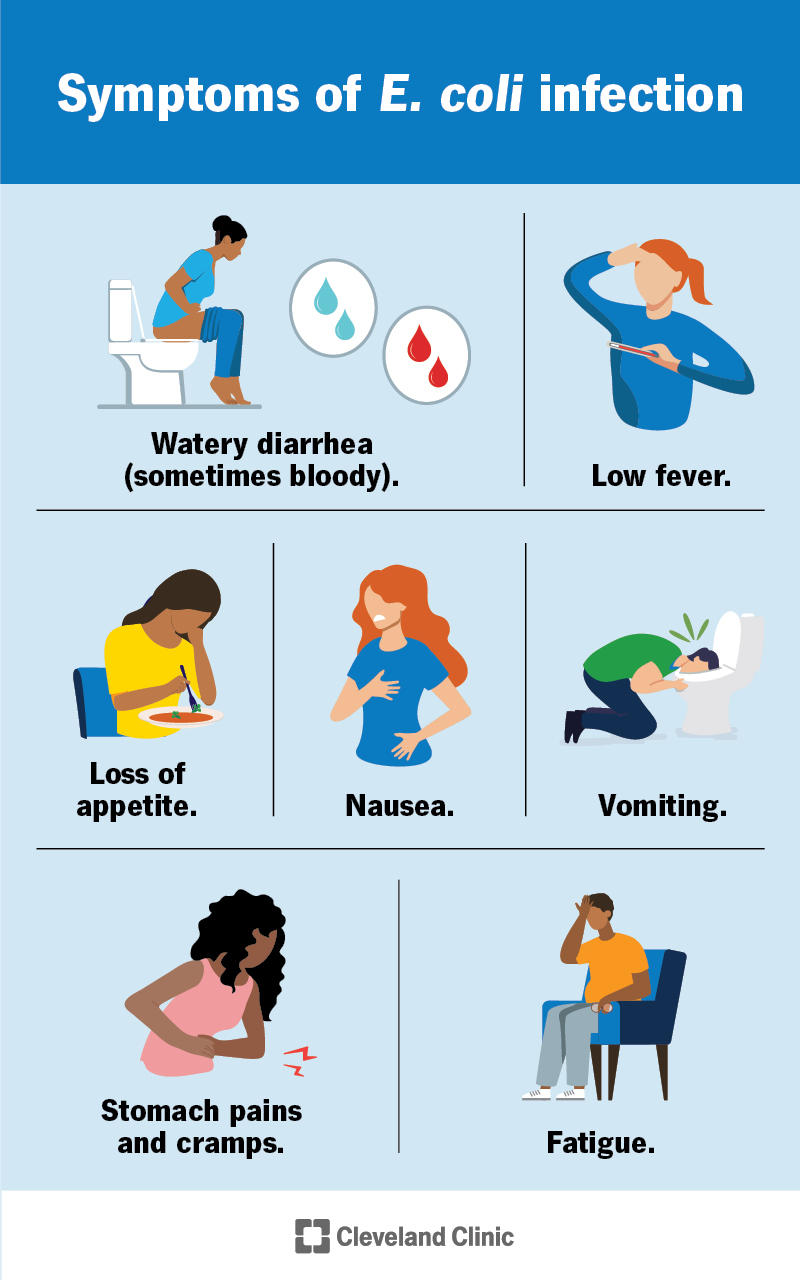
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/e-coli-infection)
Escherichia coli (E. coli) is a group of bacteria that normally lives in the gut (gastrointestinal/GI tract) of healthy people and animals. The type that lives in your GI tract usually doesn’t hurt you — it even helps you digest your food. But under certain circumstances, many strains (types) of E. coli can make you sick. Many of the strains that cause infection can adhere (stick) to your cells and release toxins.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
An E. coli infection is any illness you get from strains of E. coli bacteria. For instance, there are harmful strains of E. coli that cause watery diarrhea, stomach pain and other digestive symptoms (gastroenteritis) if you accidentally ingest them. These are sometimes called diarrheagenic E. coli, and they’re often what people mean when they talk about E. coli infections. But the E. coli that usually live in your gut can also get in places they’re not supposed to be (like your urinary tract). This causes an E. coli infection there.
Many strains of E. coli cause mild infections. But some strains, like those that produce Shiga toxin, can cause serious illness, including kidney damage.
Common types of E. coli infection include gastrointestinal and urinary tract infections (UTIs). Other types of E. coli infections include:
There are about 265,000 Shiga toxin-producing E. coli (STEC) infections each year in the U.S. STEC is the most common cause of E. coli outbreaks and serious illness from E. coli in the U.S.
Advertisement
Symptoms of E. coli gastroenteritis include:
Watery diarrhea is usually the first symptom of an E. coli infection in your GI tract. You can also have different symptoms depending on where in your body you’re infected.
If E. coli infects parts of your urinary tract, you might have:
You usually develop symptoms of an STEC infection within three to five days after drinking or eating foods contaminated with this E. coli bacteria. Other strains can make you sick within hours. Sometimes, symptoms start up to 10 days after exposure.
Many strains of E. coli can cause diarrheagenic infections in your GI tract. Most cause similar symptoms, like watery diarrhea, but some are more serious than others. Scientists categorize them by how they attach to your cells and the types of toxins they release.
Types of diarrheagenic E. coli include:
Other notable types of E. coli include uropathogenic E. coli (UPEC), which can cause UTIs, and E. coli K1, which can cause meningitis in newborns.
STEC is a strain of E. coli that releases a toxin (Shiga toxin) that damages your cells. These are the same toxins released by Shigella bacteria. STEC is known for causing severe outbreaks of E. coli (where many people get sick), often from contaminated food.
STEC is also called enterohemorrhagic E. coli (EHEC) because it can lead to bleeding in your intestines, causing bloody diarrhea (hemorrhagic colitis). About 5% to 10% of people with STEC develop hemolytic uremic syndrome (HUS), a condition that causes blood clots and damages your kidneys. The subtype E. coli O157:H7 is the most likely to cause severe illness.
Enterotoxigenic E. coli (ETEC) is a type of E. coli that causes infections known as traveler’s diarrhea. Symptoms start quickly after exposure — sometimes within just a few hours. ETEC is common in warm climates.
Most diarrheagenic E. coli strains spread through fecal-oral transmission. This happens when bacteria from poop that’s too small to see make their way into your mouth and digestive tract. Some forms, like STEC, can also transmit through undercooked meat and unpasteurized beverages.
Advertisement
Specifically, you can get E. coli from:
Babies sometimes get E. coli infections during birth.
Yes, E. coli can be contagious (spread from person to person). While you don’t get it from sneezing or coughing, you can get it from caring for someone with an E. coli infection, especially if you come in contact with their poop. You can also get it from objects, surfaces or food someone with an E. coli infection has touched if they don’t wash their hands well enough.
Advertisement
Anyone who comes into contact with a disease-causing strain of E. coli can get infected. People who are at greatest risk include:
E. coli sometimes causes life-threatening complications, including:
How your provider diagnoses E. coli depends on what your symptoms are. If you have diarrhea or other digestive symptoms, your provider will test a stool (poop) sample for E. coli. If you have other symptoms, they might test your urine (pee), blood or cerebrospinal fluid (CSF).
Specific tests for E. coli include:
You often don’t need to treat E. coli infections that cause digestive symptoms. Healthcare providers specifically don’t treat STEC with antibiotics or antidiarrheal medicines. These medications can increase your risk of HUS if you have STEC. Instead, they’ll monitor your condition and give you fluids to prevent dehydration if needed.
Advertisement
But if you have another type of E. coli infection — like a UTI, meningitis or sepsis — or if your symptoms are severe, your provider will treat you with antibiotics.
Some antibiotics providers use to treat E. coli infections include:
E. coli infections can cause everything from brief bouts of diarrhea to life-threatening illness. Most people recover on their own or with antibiotic treatment. Providers usually don’t treat STEC infections, but you might need supportive care, like supplemental fluids or nutrition. You might also be hospitalized and isolated to keep STEC from spreading.
Depending on the type of E. coli infection you have, your symptoms can last from two days to two weeks. STEC infections usually last five to seven days.
Mild E. coli gastroenteritis and some UTIs caused by E. coli can go away on their own. Recovery can take about a week without any treatment. But you should always check with a provider if you have severe or long-lasting diarrhea, abdominal pain, pain when you pee, or are peeing very little.
Yes, E. coli infections can be deadly. Studies suggest the mortality (death) rate for E. coli infections is around 17%. But the results of these studies vary widely (from 8% to 35%). In general, E. coli UTIs are less likely to be fatal than other kinds of E. coli infections.
Sepsis is the most common cause of death in people with E. coli infections. People who are younger than 1 or older than 44, who have a respiratory infection, or who have an infection that doesn’t respond to antibiotics have higher mortality rates.
The most important thing you can do to protect against E. coli infections is to wash your hands. It’s particularly important to wash them thoroughly with warm water and soap:
You can also reduce your risk of an E. coli infection by following safe food preparation procedures:
Don’t eat or drink anything that makes diarrhea worse, like caffeine or alcohol. Drink plenty of fluids to stay hydrated. If a provider has diagnosed you with STEC (especially E. coli O157:H7), don’t take anti-diarrheal medications like bismuth subsalicylate (Pepto-Bismol®, Kaopectate®) or loperamide (Imodium®). These medications can increase your risk of HUS.
See a healthcare provider if you have diarrhea for more than three days, symptoms of a UTI or other health concerns.
Go to the nearest emergency room or seek immediate medical care if you:
It might be helpful to ask a healthcare provider:
E. coli is one of the many bacteria that can live in our bodies without harming us. But some strains can make us sick, especially if they get into places they aren’t supposed to be. Many E. coli infections can go away on their own. See your provider if your symptoms last more than a few days or are severe.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
