Meningococcal disease is a serious bacterial infection. It’s contagious between people, usually from infected spit or mucus. It shares many of the same symptoms as a cold or the flu. But a common symptom of meningococcal disease is a stiff neck. Treatment includes antibiotics. The sooner you get treatment, the better your chances of recovery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
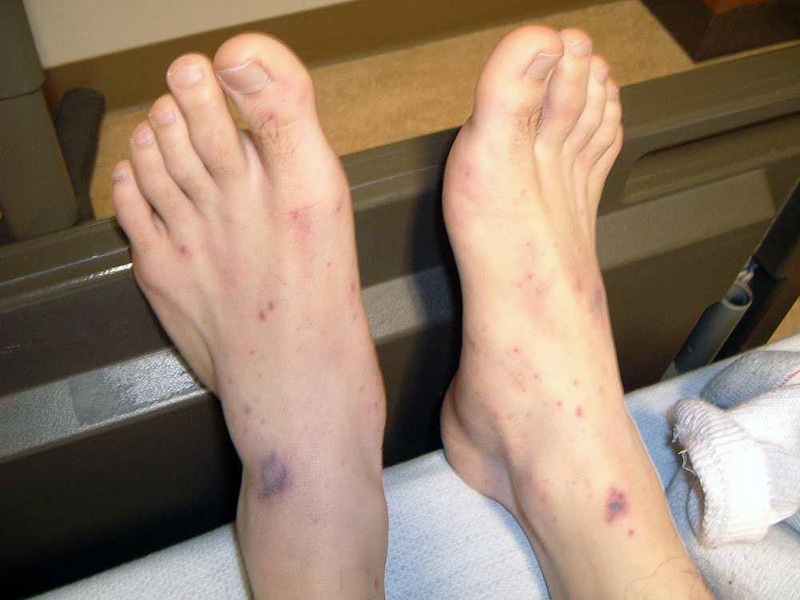
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22442-meningococcal-disease-1)
Meningococcal disease (meh-ning-goh-KOK-uhl deh-ZEEZ) is a rare infection that Neisseria meningitidis (N. meningitidis) bacteria cause. Another name for N. meningitidis is meningococcus (meh-ning-goh-KOK-uhs).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
N. meningitidis can infect your meninges and blood. Your meninges are the three membranes that cover your brain and spinal cord. Membranes are thin layers of tissue that protect what they surround, like the skin around an orange or grapefruit.
In 2023, there were around 400 cases of meningococcal disease in the U.S.
Meningococcal disease is serious. It can be fatal without treatment. Get medical help immediately if you have symptoms of the disease.
Common symptoms of meningococcal disease include:
Other signs that you may have meningococcal disease include:
It can be difficult to notice meningococcal disease symptoms in babies and young children. They may even be different from symptoms in older children or adults. Common symptoms include:
Meningococcal disease spreads from person to person, usually through close contact with someone who has it. It spreads through spit or mucus through activities like:
Advertisement
N. meningitidis doesn’t live long outside of your body. It can’t survive on surfaces.
Anyone can get meningococcal disease. But you’re at a greater risk of developing it if you:
Meningococcal disease is serious. About 10 to 15 out of every 100 people who have meningococcal disease die, even with treatment.
About 1 in 5 people who survive have long-term complications, including:
Meningococcal disease can be challenging for healthcare providers to diagnose because it shares many of the same symptoms as the common cold or flu. If a provider suspects you have meningococcal disease, they’ll recommend blood tests and a spinal tap to collect spinal fluid.
They’ll send your samples to a lab to look for bacteria and see if they grow. If N. meningitidis grows in your samples, that means you have meningococcal disease.
If providers can’t tell if you have meningococcal disease from your samples, they may order a PCR test.
Healthcare providers treat meningococcal disease with antibiotics like ceftriaxone (Ceftrisol Plus®, Rocephin®) or penicillin. They usually give them to you through an intravenous (IV) tube they inject into a vein. If they think you have meningococcal disease, they’ll start you on antibiotics even before an official diagnosis. It’s very important to start treatment as soon as possible.
In addition to antibiotics, you may need treatments such as:
Contact a healthcare provider immediately if you or your child has symptoms of meningococcal disease. If you have any reactions to your treatments, or if you find your symptoms getting worse, reach out again.
During your appointment, you may wish to ask the following questions:
Advertisement
Meningococcal disease is very serious. It can even be fatal. Getting treatment right away is very important. But even with early treatment, it’s still possible to have complications, including permanent damage to your skin or loss of limbs. A complete recovery can take weeks or months. You’ll receive antibiotics over seven to 10 days. But it may take longer to feel better.
Unlike other types of infections, you can get meningococcal disease more than once. Healthcare providers might test your immune system if you get it again.
Yes, you can help prevent meningococcal disease in a few different ways. They’re similar to how you might prevent other bacterial infections.
Avoid close contact with people who are sick. Don’t share food or drinks. If you have to spend time around people who are sick, it’s a good idea to wear a mask over your nose and mouth. You should also wash your hands and avoid touching your eyes, nose or mouth with unclean hands.
There are three vaccines in the U.S. that help prevent meningococcal disease:
If you take complement inhibitors or are in close contact with someone who has meningococcal disease, healthcare providers may suggest you also take antibiotics.
Advertisement
Even though they sound the same, meningococcal disease and meningitis are different issues. N. meningitidis causes meningococcal disease. Meningitis refers to inflammation of your meninges. It can happen if you have meningococcal disease. But it can happen if you have other conditions, too. N. meningitidis doesn’t cause all cases of meningitis.
Meningococcemia is another condition N. meningitidis causes. It happens when the bacteria get into your bloodstream and cause an infection. It can destroy your blood vessels and keep the tissues in your body from getting oxygen.
With symptoms like a fever and body aches, meningococcal disease can look like other less serious diseases. But it’s also rare. So how should you know when to see a healthcare provider? If you have flu-like symptoms along with a stiff neck, skin rash and/or light sensitivity, it’s time to make an appointment. The disease gets worse quickly, and getting treatment as quickly as possible is important to your recovery. You can also give yourself some peace of mind by talking to a healthcare provider about meningococcal disease vaccines. Shots aren’t fun. But some temporary discomfort is better than the serious meningococcal disease complications.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a virus, fungus or bacteria? Some of these “bugs” won’t go away on their own. Cleveland Clinic’s infectious disease experts are here to help.
