Occasional indigestion (dyspepsia) is common and not serious. If you get a stomachache after a large meal, you can usually relieve it with an antacid. But if you have indigestion often, there might be more going on. Sometimes, it means you have a treatable condition, like acid reflux or peptic ulcer disease. Other times, it’s more complex.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
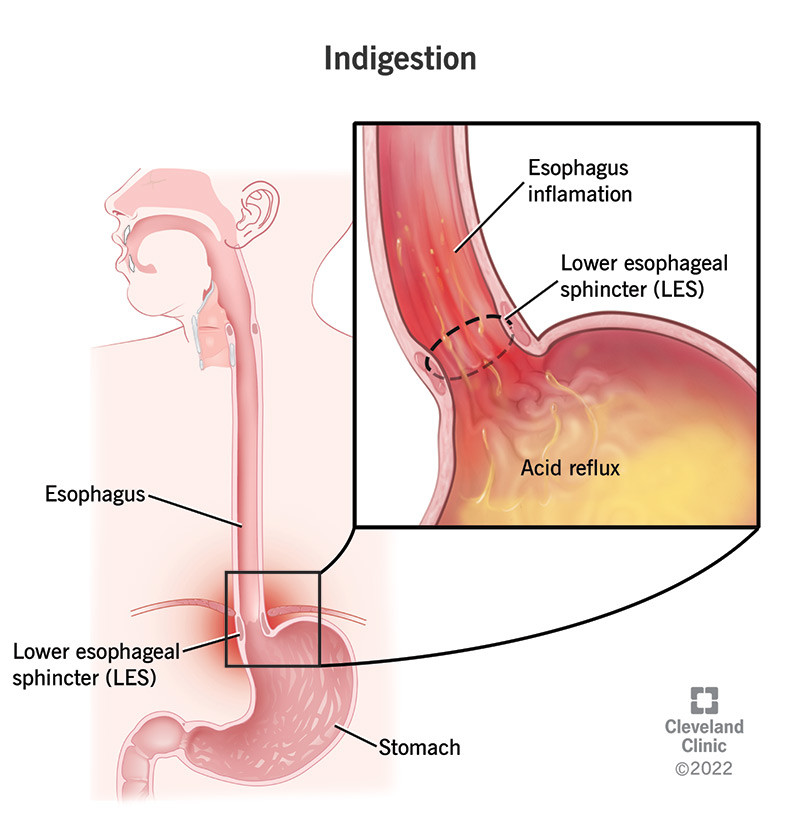
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/7316-indigestion-dyspepsia.jpg)
Indigestion is pain or discomfort that happens while your stomach digests food. It’s also called dyspepsia, which means impaired digestion. If you often get a stomachache after eating, something in your digestion may not be working as it should.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Indigestion isn’t usually serious — small changes in your eating habits can help. But how often it happens and how severe it feels matter.
Most people have occasional indigestion. For others, it happens often enough to affect daily life. If that’s the case, you may want to see a healthcare provider. Sometimes, indigestion is a sign of an underlying digestive condition. Other times, there’s no clear cause.
Healthcare providers define indigestion (dyspepsia) by the following three symptoms:
Symptoms often show up within minutes to a few hours after a meal. It normally takes three to five hours for your stomach to digest food before passing it to your small intestine. During this time, your pancreas and gallbladder release enzymes and bile to help break food down — right in the same area where indigestion pain tends to show up.
Advertisement
Many people who experience indigestion also report additional symptoms, including:
These symptoms can overlap with dyspepsia, or they may occur on their own.
Sometimes, a heart attack can feel like indigestion — called a silent heart attack.
Seek emergency care if you have indigestion along with:
The most common cause of indigestion is stomach acid — especially when there’s too much of it or when it gets where it doesn’t belong. Acid can irritate the lining of your stomach, esophagus or small intestine, causing that familiar burning or painful sensation.
This extra acid often results from underlying conditions like GERD (acid reflux) or peptic ulcer disease, which are among the most common causes of chronic indigestion.
But indigestion can also stem from what and how you eat, how well your digestive system functions and how your nerves interpret discomfort in your gut.
Occasional indigestion
Sometimes, indigestion is simply due to overeating or eating rich, fatty foods. These meals require more digestive effort, which means more acid and stronger contractions from your stomach, gallbladder and pancreas. This extra activity can irritate your digestive tract and cause temporary discomfort.
Chronic indigestion
When indigestion happens regularly, it may be linked to a digestive condition — or it may have no identifiable cause.
These acid-related conditions are among the few clear “organic” causes of indigestion. When symptoms like heartburn, regurgitation or belching appear alongside dyspepsia, GERD is often the reason. If nausea, early fullness or bloating are present, peptic ulcer disease may be the cause.
When testing rules out acid-related disease, the diagnosis is often functional dyspepsia — a condition where overly sensitive gut nerves misinterpret normal digestion as pain or discomfort.
You’re more likely to experience indigestion if you have certain conditions or lifestyle factors that affect your digestive system or increase acid production:
Health conditions linked to dyspepsia include:
Advertisement
Lifestyle factors that may raise your risk include:
Specific food triggers include:
If your indigestion is mild or only happens once in a while, you probably don’t need a formal diagnosis. But if it’s frequent, severe or interfering with your daily life, your provider will start by asking about your symptoms.
They’ll likely begin with:
In some cases, your provider may prescribe acid-blocking medication first to see if it helps. If it does, your symptoms are likely related to stomach acid. If it doesn’t — or if you have other concerning symptoms — your provider may recommend further testing to check for an underlying condition.
Tests might include:
If tests don’t show any clear cause and acid-reducing medications don’t help, your provider may diagnose functional dyspepsia.
Advertisement
If your symptoms are mild or occasional, you can often manage them with simple changes:
If you have traditional acid-related indigestion, your provider may prescribe medications to reduce or manage stomach acid. These can include:
Advertisement
If you have functional dyspepsia, treatment may involve a combination of:
It may take some trial and error to find what works best for you.
See a healthcare provider if your symptoms are frequent, if antacids don’t help or if you’re relying on antacids too often and need a longer-term plan. You should also seek care if your current treatment stops working or if you develop new or concerning symptoms.
Red-flag symptoms include:
Not all causes of indigestion are curable, but most are treatable. Depending on the underlying issue, you may need occasional or daily treatment — sometimes long-term.
Medications that reduce stomach acid are often effective, but they can have side effects. You may need to work with your provider to find the right balance.
Functional dyspepsia can be harder to treat, and not everyone finds lasting relief.
Indigestion is common and usually not serious. But when it happens often, it can interfere with your eating, sleeping and overall quality of life. It may be a sign of an underlying condition — and in rare cases, a serious one.
Your digestive system is complex. An experienced healthcare provider can help you figure out what’s going on and guide you toward relief.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Chronic indigestion can affect your daily routine or make you feel worried and anxious about eating. We can help with treatments to bring relief.
