Angina is chest pain or discomfort that comes and goes. Angina may be a sign of a heart attack, and you should seek medical care if you’re experiencing angina. Your provider will work to treat your symptoms and the underlying cause.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
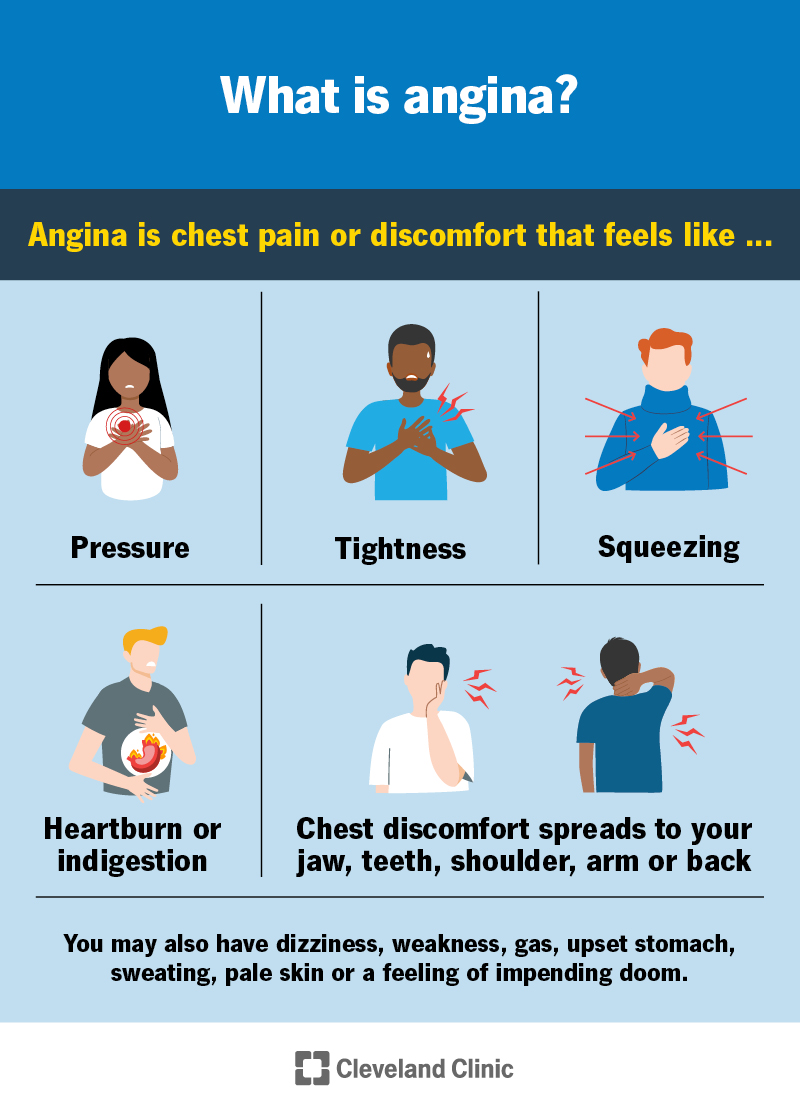
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21489-angina.jpg)
Angina (commonly pronounced an-JY-nuh) is chest pain or discomfort that happens when your heart isn’t receiving enough blood. Angina is a symptom of heart disease — most commonly plaque buildup or a blockage in your coronary arteries. Without treatment, dangerous complications like a heart attack or cardiac arrest could occur.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
About 11 million people in the U.S. experience angina. It’s common and generally treatable. The most important thing you can do is tell your provider about any chest discomfort you feel. This is true even if you think it’s minor. Don’t ignore any new or changing symptoms. Angina can range in severity from a vague ache in your chest to crushing pressure.
Angina can be a warning sign of a heart attack — sometimes days or weeks in advance. If you have unexpected, severe or worsening chest pain, call 911 (or your local emergency services number).
Angina pectoris is another name for this same symptom. But providers usually just call it angina.
Most people with angina describe having chest pressure or pain. It can be mild or more severe. It’s common to feel vague discomfort, rather than actual pain. Angina might feel like:
This discomfort may spread to your jaw, teeth, shoulders, arm or back.
Angina can happen alongside other symptoms, like:
There are four main types of angina:
Advertisement
Healthcare providers consider your triggers when describing the severity of your angina. They may use a scale of 1 to 4. The higher the number, the more severe the angina:
Reduced blood flow to your heart causes angina. Your heart may not get enough blood due to:
You’re more likely to develop angina if you:
Medications can stop angina episodes and reduce how often you have them. But your provider will also treat the condition that’s causing your angina. This means you may need a combination of medicines, procedures and changes to your daily habits. The goals of treatment are to improve blood flow to your heart and lower your risk of a heart attack.
Your provider may recommend:
No. You usually need treatment for angina. An episode of stable angina attack may go away within five minutes of rest. But it will likely reoccur without medical evaluation and treatment.
Advertisement
Unstable angina is a warning sign of a heart attack. Don’t wait to seek medical care.
Your provider may prescribe medicines that prevent angina episodes. Follow your provider’s guidance on how to take these medicines.
You can lower your risk of developing conditions that cause angina by:
Call 911 or your local emergency number if:
Call your healthcare provider if you have:
Your provider will help you learn how to manage angina in your daily life. For example, they may ask you to keep a log of your angina episodes. Include the date and time, what it felt like, what you were doing and possible triggers. Your provider will also tell you if there are any limits on what you should do from day to day.
If your provider prescribes nitroglycerin, be sure to keep it with you at all times.
You’ve probably seen enough movies to know what chest pain looks like. But angina may not make you clutch your chest or collapse. It might not even feel like pain. It may be more subtle. And it may come and go so quickly that you question if it’s even a big deal.
Advertisement
But angina is always worth taking seriously. It’s your heart telling you that something isn’t right. And you should seek medical care. The conditions that cause angina are treatable. The sooner you start treating them, the better.
If you’ve been diagnosed with angina, talk with your provider about what’s “normal” for you. Ask your provider what’s out of the ordinary for you and when you should call 911.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
