Rectal bleeding can be a symptom of many different conditions, like hemorrhoids, inflammatory bowel disease (IBD) and colorectal cancer. You may notice blood on the toilet paper when you wipe or when you look at your poop. It’s important to contact a healthcare provider about blood in your stool. Not all causes are serious, but some of them are.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_qladieqd/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Rectal Bleeding
Rectal bleeding is when blood comes out of your anus. You might see this as blood in your stool (poop), blood on toilet paper when you wipe or blood in the toilet bowl. Seeing blood can be alarming, and your mind may race as you start to worry that something is wrong.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Blood in your poop can come from different areas of your digestive system. Sometimes, it comes from your anus (butthole), like with hemorrhoids. Sometimes, it comes from higher up, like from an issue with your stomach.
Blood in your poop can look a few different ways. You may only notice it when you wipe. You may have bright red streaks of blood on your poop. You may even see blood that contains mucus. Your poop could also look dark, black and tarry instead of bright red.
The color of the blood you see may be a clue to where it’s coming from:
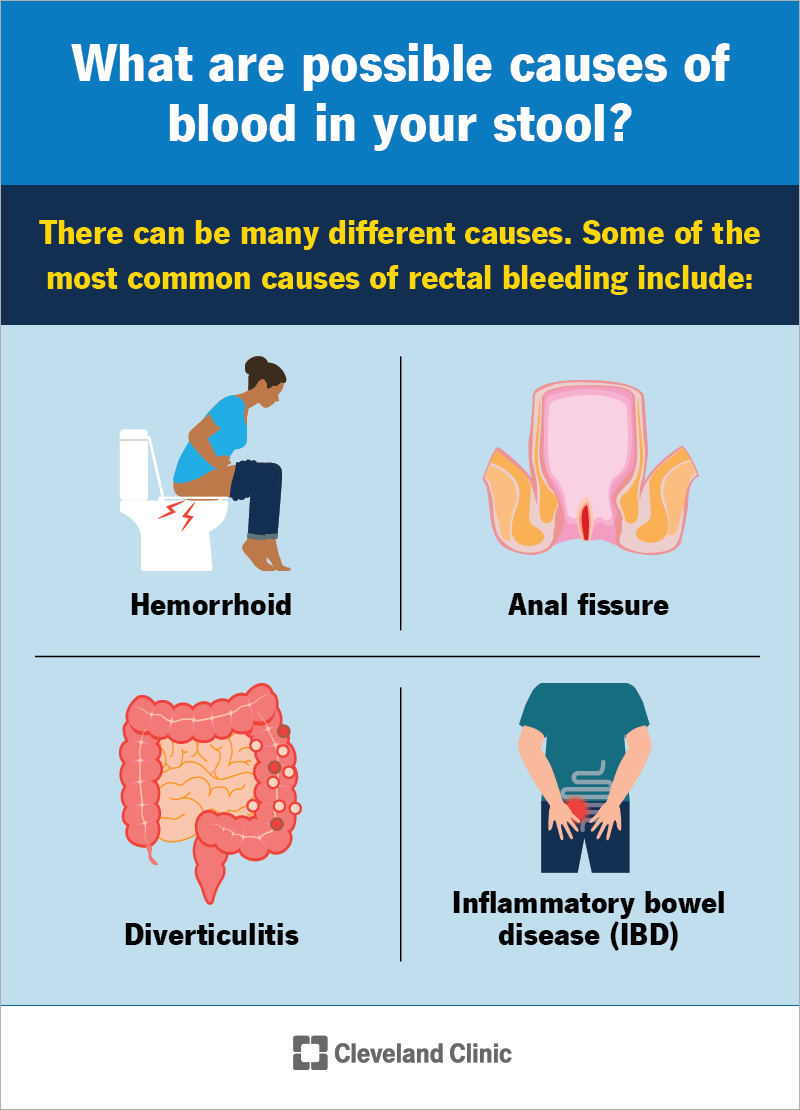
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/14612-rectal-bleeding.jpg)
There can be many different causes. Some of the most common causes of rectal bleeding include:
Advertisement
Other possible causes include:
Blood in your poop can come with other symptoms. Depending on the exact cause, you may also have:
There are many ways your provider can figure out the cause. They might start by asking questions about your pooping habits. They’ll also ask about other symptoms or health conditions you have. Your answers can help them determine which tests you may need.
They may start with a digital rectal exam to check for hemorrhoids or issues in your rectum. Then, your provider may order one of the following tests:
You probably won’t need all these tests. Your provider will decide which one is best based on your symptoms.
In most cases, rectal bleeding treatment involves treating an underlying cause.
If hemorrhoids are the cause, you may be able to treat them at home with medicated creams, warm baths or by adding more fiber to your diet to ease constipation. If bleeding is due to an infection, you may need antibiotics. More serious causes may require surgery.
Sometimes, the bleeding stops quickly. Other times, you need ongoing treatment from a healthcare provider.
Contact a healthcare provider if you notice blood in your poop or in the toilet bowl. There can be many causes of blood in your stool. Even if you think you know the cause, seeing a healthcare provider is the best way to get answers and make sure it’s nothing serious.
Advertisement
Seek immediate medical care if the bleeding is heavy or doesn’t stop, or if you have symptoms like severe pain or dizziness with it.
Bleeding can be worrisome, especially when you can’t see where it’s coming from. It might feel hard to wait for a medical appointment to find out what your rectal bleeding means. But keep in mind, while there are many possible causes, the most common ones are easy to find and fix.
Don’t be embarrassed to talk to a healthcare provider about blood in your stool. These are important symptoms, and healthcare providers will want to know all about them. Answering their questions will help them determine the type of care you need.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
