Low testosterone (male hypogonadism) is a condition in which your testicles don’t produce enough testosterone. It has several possible causes, including conditions or injuries affecting your testicles, pituitary gland or hypothalamus. It’s treatable with testosterone replacement therapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
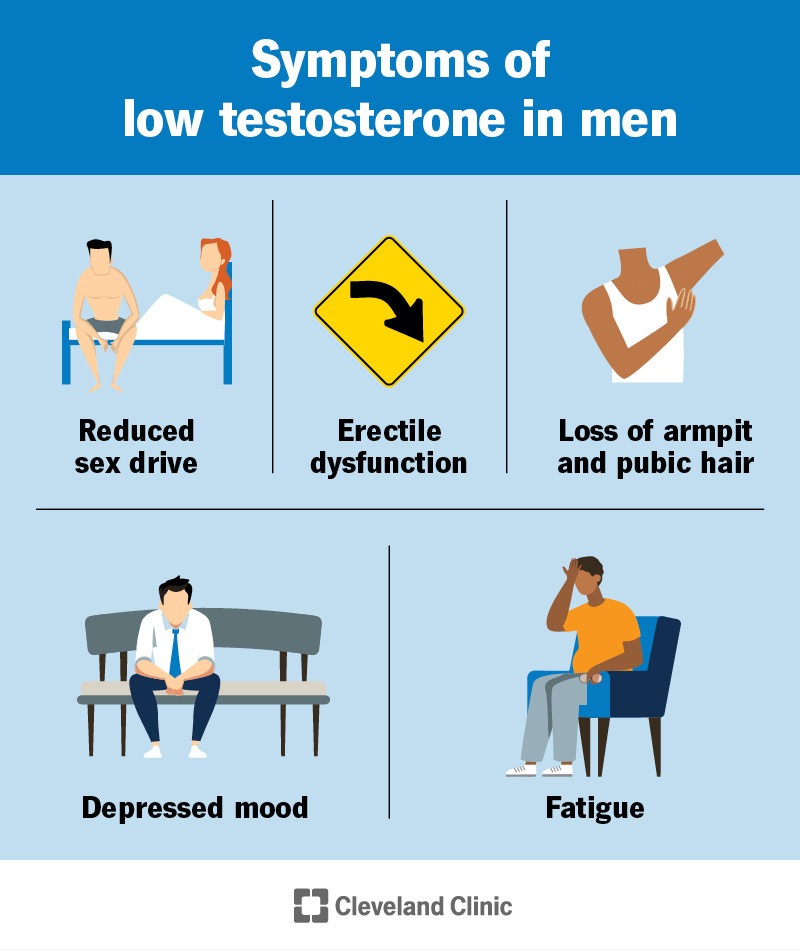
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15603-low-testosterone-male-hypogonadism)
Low testosterone means you don’t make enough of the hormone testosterone. Special cells (called Leydig cells) in your testicles make this hormone.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Testosterone levels naturally drop in men, so this is a common condition. Levels can drop 1% per year starting in your late 30s. Healthcare providers consider testosterone levels below 300 nanograms per deciliter (ng/dL) as low in adults. Providers call it male hypogonadism when you have symptoms along with these low levels. You can have different symptoms depending on your age.
You might also hear low testosterone called:
Testosterone is the main male sex hormone. It helps male features like a deepening voice and body hair growth develop. It’s much higher in men than in women.
In men, testosterone helps:
Low testosterone symptoms (low T symptoms) can vary a lot. Sexual symptoms of low testosterone are the most specific. They include:
Other symptoms that highly suggest hypogonadism in men include:
Advertisement
Other signs and symptoms include:
Boys with low testosterone before or during puberty may have:
There are several possible causes of low testosterone. Any issue with your testicles, hypothalamus or pituitary gland can cause low testosterone. This is because your hypothalamus and pituitary gland release hormones that lead to the production and release of testosterone. These signals from your brain normally control how much testosterone your testicles make and release.
A testicular disorder causes primary hypogonadism. This means it’s a problem with the testicles. Another name for it is hypergonadotropic hypogonadism.
A problem with your pituitary gland or hypothalamus causes secondary hypogonadism. This means it happens for reasons other than the testicles.
You can be born with this condition (congenital) or develop it as a child or adult (acquired).
Primary hypogonadism happens when your testicles aren’t making normal levels of testosterone. If you have damaged or missing testicles, they can’t respond to increased levels of hormones from your pituitary gland.
As a result, your testicles make too little or no testosterone and sperm.
Conditions present at birth that affect your testicles and can lead to primary hypogonadism include:
Other issues that affect your testicles and can lead to primary hypogonadism include:
Conditions that affect how your hypothalamus and/or pituitary gland work cause secondary hypogonadism. This is known as hypogonadotropic hypogonadism because there are low levels of hormones. Those low levels cause decreased testosterone and sperm production.
Advertisement
Congenital conditions that can lead to secondary hypogonadism include:
Most males with symptoms of low testosterone don’t have a problem with their pituitary glands or testicles. They usually have an issue from having obesity or diabetes. Also, being sick briefly stops testosterone production.
Other acquired conditions that can lead to secondary hypogonadism include:
Late-onset hypogonadism (LOH) is a type of secondary male hypogonadism. LOH and low testosterone are more common in those who have Type 2 diabetes, overweight and/or obesity.
Advertisement
Male hypogonadism can affect you at any age. Low testosterone is more likely to affect you if you:
Lifestyle habits that may help keep testosterone levels normal include:
If you have signs and symptoms of low testosterone, a healthcare provider will give you a physical exam. They’ll also ask questions about your medical history, medicines you take, substance use and any symptoms you have.
To make a diagnosis, a provider will consider your signs and symptoms. If you have symptoms, they’ll order blood tests.
The following tests can help confirm low testosterone and find the cause:
Advertisement
Eating nutritious foods and getting physical activity are the first treatments for low testosterone. If that doesn’t help after six to 12 months, or you have severe symptoms, you may get other treatment.
This may include medicine to help you produce testosterone or long-term testosterone therapy. This has several different forms, like:
You may not be able to receive this treatment if you have a history of:
Other treatments, like clomiphene citrate, are available for those who want to be able to have children.
If you have symptoms of low testosterone, talk to a healthcare provider. They’ll assess you and may order blood tests. If your child isn’t showing signs of puberty by the age of 14, talk to their provider.
If you’re taking hormone replacement therapy, you’ll need regular follow-up visits with a healthcare provider. These may be once or twice a year.
Questions you may want to ask your provider include:
There’s no one-time fix for low testosterone in men. But hormone replacement therapy helps improve sex drive, symptoms of depression and energy levels. Treatment may also boost muscle mass and bone density. Low testosterone may lead to weak bones (osteoporosis) or heart and blood vessel disorders.
For congenital hypogonadism, testosterone replacement therapy often helps prevent problems linked to delayed puberty.
Many people shrug off the symptoms linked with low testosterone as an unpleasant part of getting older. But you should address symptoms that interfere with your quality of life. If you have bothersome signs of low testosterone, avoid over-the-counter supplements. See a provider and discuss your options for treatment.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Have a low sex drive or trouble with erections? Low testosterone might be the cause. Cleveland Clinic’s experts can help balance your hormones.
