Radiation therapy treats cancer by killing cancer cells. It’s one of the most powerful cancer treatments. External beam radiation therapy (EBRT) is the most common type. This type may also treat noncancerous conditions. The other type is internal radiation therapy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
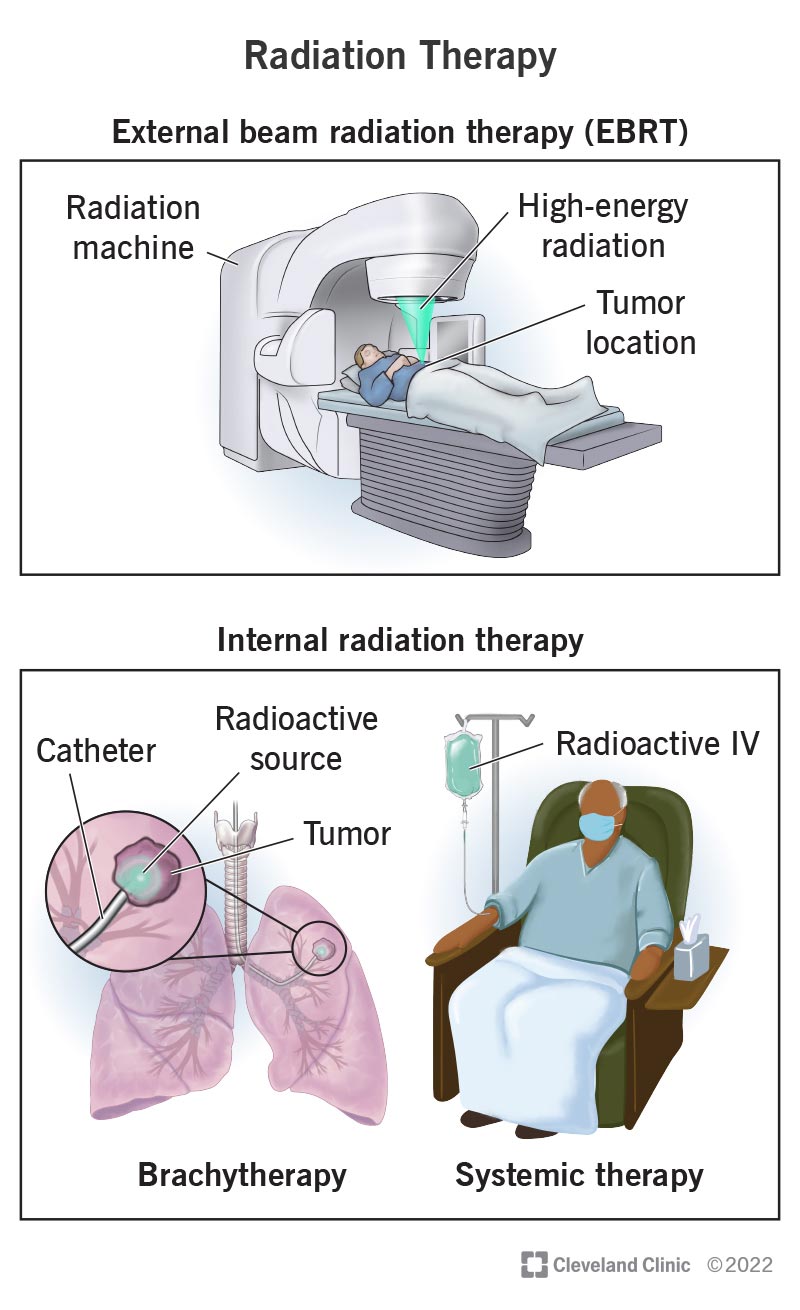
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17637-radiation-therapy)
Radiation therapy — or radiotherapy — is a common treatment that uses radiation (usually high-powered X-rays) to kill cancer cells and shrink cancerous tumors. It can also ease cancer symptoms. You may have it alone or with surgery or chemotherapy. Radiation therapy is also treatment for some noncancerous conditions.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are two types: external beam radiation therapy (EBRT) and internal radiation therapy. Both types treat cancer by destroying cancer cells’ DNA. The cells need DNA instructions to grow and multiply. Without them, cancer cells die, and tumors shrink. Healthcare providers may use low-dose EBRT to treat noncancerous conditions.
This is the most common type of radiation therapy. In EBRT, a machine directs beams of high-energy radiation toward the tumor. The energy may be X-rays (most common), electrons or protons. The machine may move around your body, but it never touches you. There are many forms of EBRT:
Advertisement
Internal radiation therapy works by placing radioactive materials inside your body. It’s a treatment for smaller tumors in your head, neck, breast, cervix, uterus or prostate. There are two types of this treatment:
A team of specialists will manage your treatment. The team will develop a treatment plan that uses radiation dosages to destroy cancer cells without harming nearby healthy tissue. The team will include your:
You’ll have a physical exam, and your team will do imaging tests like a CT scan. They’ll explain how you can prepare for the day of the procedure based on how you’ll receive the radiation.
EBRT involves planning sessions (simulations). These sessions are how your team creates the best treatment setup. The goal is treatment that’s best for your situation. Simulation involves:
EBRT and internal radiation therapy involve different steps.
With EBRT, you lie on a treatment table in the same position you were in during the simulation. The machine moves around you but never touches you. You won’t feel anything during treatment.
Your treatment may take place in a special outpatient room or in a hospital. You’ll receive anesthesia so you don’t feel pain or discomfort during your treatment. Your radiation oncologist uses a small, flexible tube to insert the seed or implant. You’ll receive radioactive fluid through an IV (in your vein) or take pills if you have systemic treatment.
Advertisement
This radiation type focuses directly on cancer cells. Your body will be radioactive for a certain time. Your radiation care team will explain how long radiation will remain in your body. They’ll also explain any steps you should take to avoid affecting others.
You should be able to continue your daily routine after EBRT. Your situation may be different if you have internal radiation therapy:
In general, external beam radiation therapy lasts up to six weeks. The different forms of internal radiation therapy may take a single day or several weeks.
Radiation therapy is one of the most powerful cancer treatments. But just like cancer isn’t a single disease, there’s no single success rate. As you think about your options, ask your team about the success rates for the treatment they recommend.
This treatment may cure some kinds of cancer. It can help other treatments work better. And radiation therapy can ease some cancer symptoms. But it may increase the chance you’ll develop a different cancer. For many people, the benefits of radiation therapy are worth the risk. Your radiation oncologist will discuss this risk with you before you start your treatment.
Advertisement
Everyone’s situation is a bit different. Some people can go back to their daily routines without any issue. Others experience side effects like fatigue or changes in their skin. Your care team will discuss any potential side effects and how they’ll help you to manage them.
Let your care team know about side effects that are more severe than you expect. They can prescribe medication to ease side effects. They may be able to adjust your dosage, change your treatment or try a different one.
Radiation therapy is a powerful, precise treatment for many kinds of cancer. Various forms of radiation therapy target specific cancers and tumor types. If you have cancer and radiation therapy is an option, don’t hesitate to ask how a specific treatment will work to kill cancer cells.
Your radiation care team will take time to explain the process from start to finish. They’ll also discuss any side effects and steps they’ll take to help you manage side effects.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic offers expert radiation oncology with advanced technology, personalized care and virtual visits to support you every step of the way.
