Celiac disease (celiac sprue) causes problems in your digestive system when you eat gluten, a protein found in wheat and other grains. It’s more serious than a normal food intolerance, though. Celiac disease causes your immune system to attack gluten in your small intestine. The attack damages your small intestine and stops it from working properly.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Celiac disease is an inherited autoimmune disorder that causes a reaction in your body to the protein, gluten. Gluten in your digestive system triggers your immune system to produce antibodies against it. These antibodies damage the lining of your small intestine (the mucosa). Damage to the mucosa in your small intestine impairs its ability to absorb nutrients from your food, causing nutritional deficiencies.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Gluten is a protein found in grains — particularly wheat, barley and rye. These grains, especially wheat, make up many of the staple foods of the standard Western diet, from breads and cereals to pasta and baked goods. Besides that, gluten often appears as an additive in food products where you wouldn’t expect to find it, such as sauces, soups and packaged foods. Beer is usually made from barley or rye.
Celiac disease affects your small intestine. This is where most of the nutrients from your food are absorbed, including proteins like gluten. But when you have celiac disease, gluten in your small intestine triggers an immune response. Your immune system sends inflammatory cells and antibodies to destroy the gluten molecules. These cells damage the mucous membrane lining your small intestine.
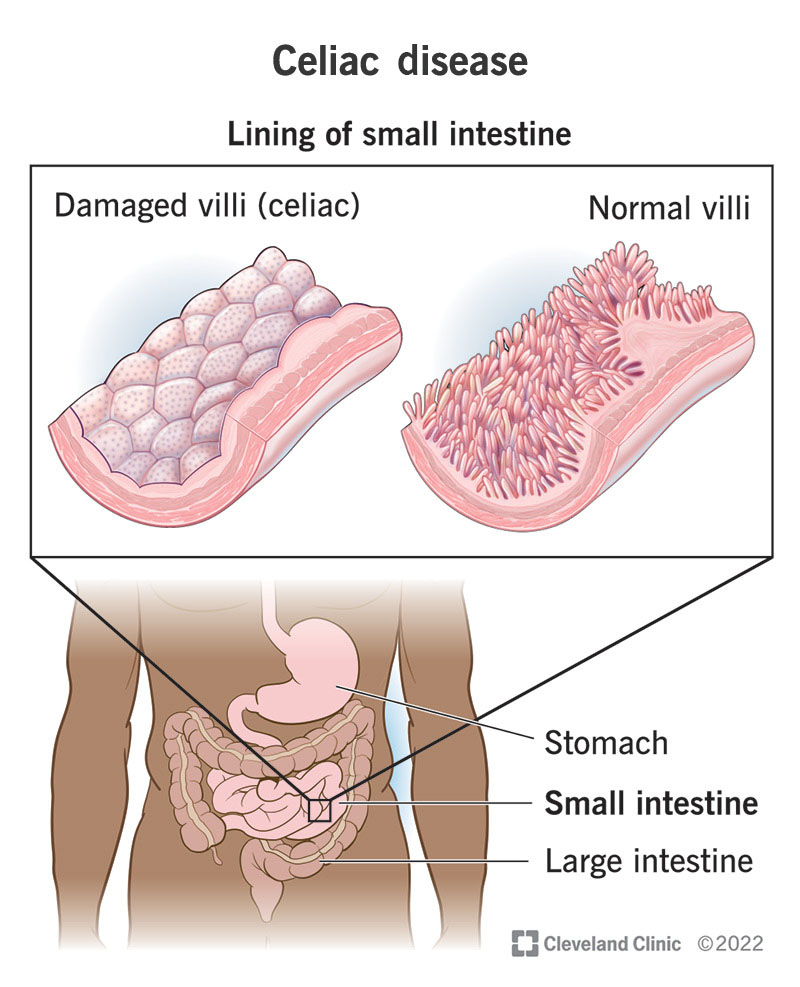
The mucosa that lines your small intestine is vast but is scrunched up into many folds and fingerlike projections, called villi. If you stretched it all out, it would cover a tennis court. These folds and projections increase the surface area in order to absorb as many nutrients as possible during digestion. But immune cells triggered by celiac disease erode and flatten these projections, diminishing the surface area.
Advertisement
Damage to your small intestine can have serious consequences. Your small intestine absorbs nutrients from your food through the mucosa. If the mucosa is damaged, it won’t be able to absorb nutrients as it should. This is called malabsorption. It can lead to malnutrition and to many other conditions that follow from the lack of different nutrients. In children, it can cause stunted growth and development.
Celiac disease is most commonly found in people of Northern European descent. It’s estimated to affect 1% of the populations of Europe and North America. You have a 10% chance of developing the disease if you have a first-degree relative, such as a parent or child, who has it. About 97% of people diagnosed with celiac disease have a recognizable gene variant associated with it (HLA-DQ2 or HLA-DQ8).
Celiac disease is more common in people with certain inherited chromosomal disorders, such as Down syndrome. It’s also more common in people with certain other autoimmune diseases. These diseases often share common genes, and they also have a way of triggering each other. Like other autoimmune diseases, celiac disease is more common in females than males. The ratio is at least 2:1.
Many autoimmune diseases, like celiac disease, are at least partly inherited (genetic disorders). That means a particular gene variant that’s passed down through family lines makes you more susceptible to developing it. But not everyone with the gene variant develops the disease, and not everyone who develops it has one of the known variants. Other factors appear to be involved in triggering it.
One theory is that it’s triggered by some type of significant physical stress that overextends your immune system. Healthcare providers have observed that the disease often shows up after a physical event such as surgery, illness or pregnancy, or a severe emotional event. Another theory is that microorganisms living in your gut are involved. More research is needed to explore these theories.
Celiac disease can appear at any age after you or your child has begun eating gluten. Healthcare providers most commonly see it appear during two distinct age windows: early childhood, between 8 and 12 months old, and mid-life, between the ages of 40 and 60. The window in early childhood is typically when children begin eating solid foods that may include biscuits or cereals with gluten in them.
Advertisement
Symptoms of celiac disease vary widely among people, which can make it hard to recognize. Some people don’t notice any symptoms at all. Some experience indigestion and other gastrointestinal (GI) symptoms after eating gluten. Some only have vague symptoms of nutritional deficiencies later on, when real damage has been done. In these people, symptoms of anemia may be the first to present.
You might have:
Gastrointestinal symptoms, such as:
Symptoms of iron-deficiency anemia, such as:
Other symptoms of malnutrition, such as:
Dermatitis herpetiformis: About 15% of people with celiac disease develop this chronic skin condition as a side effect. It's also called the “gluten rash” or “celiac rash”. The same gluten antibodies that damage your small intestine in celiac disease cause this condition. Dermatitis herpetiformis manifests as an itchy rash that looks like clusters of bumps or blisters. It typically affects your elbows, knees, buttocks or scalp.
Advertisement
You might suspect you have celiac disease if you have gastrointestinal symptoms after eating gluten. Many people appear to have a sensitivity to gluten or wheat products in their diet. Food intolerances can cause uncomfortable symptoms after eating, but they don’t damage your intestines the way celiac disease does. To diagnose celiac disease, healthcare providers will look for evidence of this damage.
It’s important to get tested for celiac disease before you try a gluten-free diet, so the tests can reveal how gluten actually affects your body. Once you begin avoiding gluten, your gut will begin to heal. Healing is good, but it’ll erase the evidence of celiac disease. You and your healthcare provider need to know for sure if you have it in order to know what kind of care you’ll need going forward.
Healthcare providers use two methods of testing for celiac disease. They prefer to use both together to confirm the diagnosis. The first is a blood test. Providers test your blood for antibodies to gluten. Then, they’ll look for the damage itself. This requires taking a small tissue sample from your small intestine (biopsy) to examine under a microscope.
To take the sample, a gastroenterologist will perform an endoscopic exam of your small intestine. Endoscopy involves passing a tiny camera through your body on the end of a long, thin tube. An upper endoscopy passes the endoscope down your throat to reach the top part of your small intestine (duodenum). Guided by the camera, the endoscopist can pass tools through the catheter to take a biopsy.
Advertisement
After confirming celiac disease, your provider will want to test your blood for specific vitamin and mineral deficiencies. Severe deficiencies can have wide-ranging effects on your body and may need to be treated directly with supplements. Common findings include iron-deficiency anemia, vitamin-deficiency anemia and vitamin D deficiency. You may also be low in electrolytes, such as calcium.
The first and most important step in treating celiac disease is to stop eating gluten. You can’t change the way your body reacts to gluten, but you can prevent gluten from triggering that reaction. When you stop eating gluten, your small intestine will begin to heal and will soon be able to absorb nutrients again. You have to maintain a strict gluten-free diet for life, though, to avoid hurting your small intestine again.
Additional treatment may include:
Most people find their symptoms begin to improve almost immediately after starting a gluten-free diet. It may take several weeks to replace your nutritional deficiencies and several months for your gut to fully heal. It can take longer in some cases, depending on the extent of the damage and how long it’s been going on. You can also delay healing if you aren’t strict with your diet.
Most people who’ve been diagnosed and have stopped eating gluten have an excellent prognosis. Most of the damage done by celiac disease can be undone. If you continue to have symptoms, it may be that you’re consuming small amounts of gluten without realizing it, or you may have a secondary condition. Only 5% of people have truly refractory celiac disease that doesn’t respond to diet.
If you go many years before being diagnosed or you don’t succeed in avoiding gluten afterward, the effects of celiac disease can be more severe and long-lasting. Malnutrition can affect your nervous system and skeletal system and some of these effects are hard to reverse, especially when they occur during childhood development. Chronic inflammation (enteritis) can also lead to other problems in your intestine.
Complications of chronic malnutrition can include:
Complications of chronic inflammation can include:
Avoiding gluten in all its forms can be daunting at first. You’ll have to learn to read labels carefully and watch out for accidental contamination. The good news is that there’s an abundance of resources available to help you navigate your new diet. Your healthcare provider will refer you to a registered dietitian to get you started. There are also many dedicated support groups and references online.
Gluten is found naturally in certain grains and products made from grains, including:
These grains are used to make:
It’s also added to many processed food products, such as:
Make sure to check labels for hidden gluten before eating processed foods.
A celiac disease diagnosis will change your diet and lifestyle forever. It’ll also change your life for the better. Before diagnosis, you were almost certainly eating gluten and doing progressive damage to your small intestine. You may have had strange and uncomfortable symptoms for years without knowing why. Now that you know, the power’s in your hands to restore your health.
If celiac disease gets in the way of your everyday life, Cleveland Clinic’s experts can help. We can craft a treatment plan that’s specific to you.

Last reviewed on 12/01/2022.
Learn more about the Health Library and our editorial process.