An endoscopy uses a scope that goes inside your body to take pictures or videos of organs and other structures. Healthcare providers use them to screen, diagnose and treat conditions. There are many types of endoscopy that view different organs. The most common types of endoscopy include colonoscopy, upper endoscopy and laparoscopy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
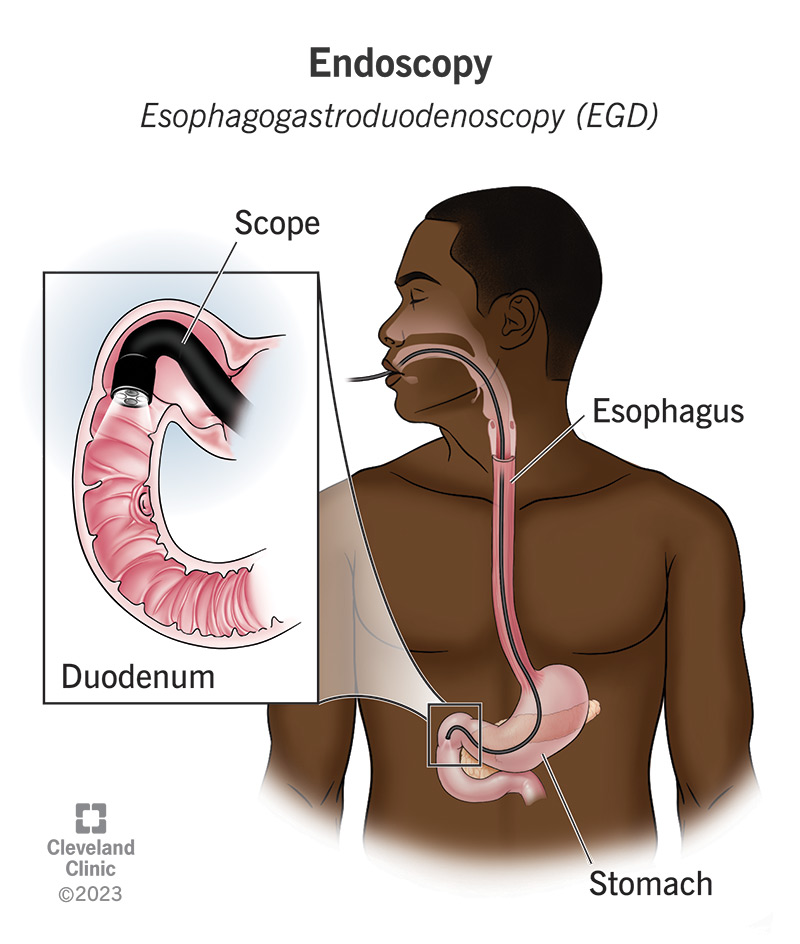
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/25126-endoscopy)
An endoscopy is a procedure done to examine structures inside your body up close. During an endoscopy, a healthcare provider places a long, thin tube (endoscope) inside your body until it reaches the organ or area they need to check. Most endoscopes have a light and special camera at the end. The scope captures images or videos of organs or other body parts. It displays them on a screen your provider sees.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Many endoscopes have special channels inside. Providers can insert operating instruments to remove tissue or perform surgery during an endoscopy.
There are many types of endoscopy procedures. But they all work in the same basic way. A healthcare provider gently inserts a scope into a body opening or small incision. The scope allows them direct access to parts of your body they need to examine or treat.
Key differences include:
The procedure specifics, including the body parts your provider is examining and where the scope goes in, are different, too.
Advertisement
Researchers and scientists continually develop new technologies to make endoscopies even less invasive. For example, a capsule endoscopy shows your organs up close without a scope. Instead, you swallow a vitamin-sized capsule with a camera inside. As the capsule travels through your esophagus, stomach and small intestine, it takes pictures that can help diagnose bleeding and tumors in your digestive system.
Healthcare providers use endoscopies to screen for conditions and diagnose diseases. A colonoscopy is probably the most well-known endoscopy used to screen for diseases. It’s used to detect colon cancer. One of the most well-known diagnostic uses of endoscopy is that it allows providers to remove abnormal tissue for lab testing. This is called a biopsy. Biopsies can show if growths are cancerous or noncancerous.
When providers first used endoscopy, they primarily used it to examine organs. Now, they can use endoscopy for many different treatments, such as fixing a bleeding stomach ulcer. In the past, a problem like this could’ve required surgery.
An endoscopy can detect diseases that affect your:
Some endoscopes can be used with instruments that allow providers to:
During a laparoscopy, providers operate on organs through tiny incisions instead of a large opening. This is sometimes called keyhole surgery. It’s much less invasive than traditional surgery. It’s the preferred technique for treating many conditions.
You’ll receive instructions based on the type of endoscopy. You may be asked to:
Advertisement
An endoscopy typically takes 30 minutes to two hours, depending on the procedure type. Most people go home on the day of their endoscopy, but some endoscopies require an overnight hospital stay.
Providers use moderate sedation for most endoscopies so that you’re asleep and pain-free during the procedure. General anesthesia (which involves intubation, or placement of a breathing tube) is necessary in a small percentage of cases. Some people may instead get local anesthesia and a sedative. Local anesthesia numbs a particular area instead of putting you to sleep completely. Sedatives help you relax.
Once you’re completely relaxed or asleep, the provider gently inserts the scope until it reaches the area they want to examine. They’ll adjust the scope to display the correct organs or structures on the screen. They’ll note irregular areas and remove tissue or provide treatment if needed.
They’ll close any incisions.
The anesthesia and sedatives prevent you from experiencing pain during the procedure. With some procedures, like a colonoscopy, you may feel pressure when the scope goes in, but the feeling passes quickly.
Your care team will monitor your vitals. You’ll likely feel groggy from the anesthesia, but most people go home on the day of their procedure. You may need to take it easy the rest of the day and avoid using any heavy machinery.
Advertisement
Ask your healthcare provider what to expect during recovery, depending on the endoscopy procedure.
Most side effects improve within the first two days. They depend on the type of procedure and where the scope went. For example, you may feel hoarse or have a mild sore throat if the scope was in your throat. You may notice cramps, bloating or nausea if the scope was in your intestines.
Your healthcare provider will recommend ways to manage the discomfort. They’ll prescribe pain medicine as needed.
Your healthcare provider will let you know when to expect results. They may discuss findings with you the same day, or they may schedule a follow-up appointment to review results with you.
An endoscopy is a common procedure that’s considered safe. Still, complications, like tears and infections, can happen. Contact your healthcare provider if you notice:
It depends. You may be asleep during some endoscopy procedures, including those involving your GI (gastrointestinal) tract. For other types, you may be awake but with medicines that prevent you from feeling any pain.
Advertisement
Your healthcare provider can explain whether you’ll be asleep or awake for your procedure.
Even with pain meds, having a scope inside your body doesn’t exactly sound pleasant. If it helps, think of the benefits it can provide. Sometimes, it provides visual evidence of conditions that traditional imaging, like an ultrasound, can miss. In this case, an endoscopy can save you a return visit to the provider to take additional views. Certain biopsies can only be done through an endoscopy. For some conditions, endoscopies are the new standard in treatment. They make for faster surgeries with shorter healing times.
Take heart that most endoscopies are only 30 minutes. Chances are, you’ll be in and out the same day, with the peace of mind that you’re valuing your health and taking care of yourself.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Having an endoscopy can be lifesaving. Cleveland Clinic’s providers will help you feel comfortable with the process so you can get the care you need.
