Osteopenia is the medical definition for bone density loss. It can become osteoporosis if the bone density loss worsens. Some health conditions, habits and medications can increase your osteopenia risk, but it usually happens naturally as you age. Your provider will suggest treatments that slow down bone loss and improve osteopenia.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
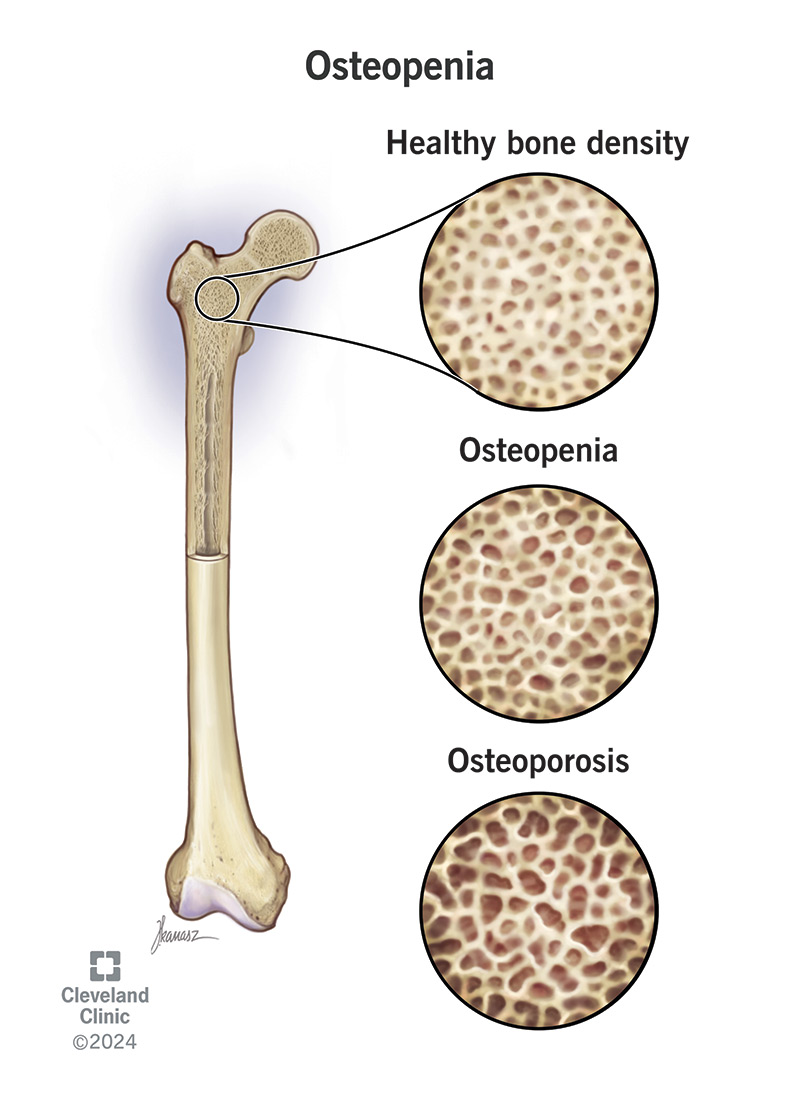
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/osteopenia)
Osteopenia is a loss of bone density. Having reduced bone density means your bones don’t have as much mineral content as they should. This can make them weaker and increase your risk of bone fractures (broken bones).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you have osteopenia, your bone density is lower than average. It can progress to osteoporosis.
Most people need their bone density checked every few years after they turn 50 or enter postmenopause, but you might need yours monitored more often. Visit a healthcare provider for regular checkups. They’ll tell you when you’ll need your bone density tested.
Osteopenia is an early sign of osteoporosis. Their names sound so similar because they’re closely related.
Osteopenia is the medical definition for having reduced bone density. Osteopenia is the warning sign that means you have an increased osteoporosis and fracture risk.
If it’s not treated, osteopenia can become osteoporosis. Osteoporosis silently weakens your bones. People with osteoporosis are much more likely to break a bone, especially from falls. If you have osteoporosis, even a minor slip that might not normally cause injuries can lead to fractures.
Experts estimate that more than 40 million Americans have osteopenia. They think around one-third of adults older than 50 have some degree of bone density loss.
Osteopenia doesn’t usually cause any symptoms you can feel or notice. That’s why healthcare providers sometimes call osteopenia and osteoporosis silent diseases.
Advertisement
Osteopenia usually happens naturally as you age. Your bones are living tissue like any other part of your body. It might not seem like it, but they’re constantly growing, changing and reshaping themselves throughout your life.
Most people lose some bone density as they get older. Your bones are densest around age 25 and start breaking down faster than your body can rebuild them after that. This natural decline doesn’t cause issues in most people. However, if you lose too much bone density, you can develop osteopenia, which may mean you’re more likely to have osteoporosis later in your life.
Anyone can develop osteopenia, but some groups of people are more likely to have it, including:
Some health conditions can lower your bone density or worsen osteopenia, including:
Medications that can increase your osteopenia risk include:
Increasing your bone fracture and osteoporosis risk are osteopenia’s main complications. Osteopenia on its own won’t cause symptoms. But having reduced bone density makes you much more likely to break a bone, even after small injuries or falls.
A healthcare provider will diagnose osteopenia with a bone density test. A bone density test is an imaging test that measures the strength of your bones. It uses X-rays to measure how much calcium and other minerals are in your bones.
Checking for changes in your bone density is the best way to catch osteopenia before it becomes osteoporosis. Your provider might suggest you get regular bone density tests if you have a family history of osteoporosis. Females usually need bone density screenings regularly after they turn 50. Males typically need them after age 70.
If you have osteopenia, you’ll probably need a bone density test every few years to see how your bones have changed.
Advertisement
Your provider will suggest osteopenia treatments that slow down your bone loss and strengthen your existing bone tissue. The most important part of treating osteopenia is preventing bone fractures and osteoporosis.
The most common osteopenia treatments include:
Advertisement
You should expect to monitor your bone density for the rest of your life if you have osteopenia. Most people with osteopenia need their bone density checked every few years. Your provider will tell you how often you’ll need bone density tests.
Osteopenia is a natural progression of bone loss. But you can slow it down to prevent osteoporosis. The sooner you know you have osteopenia, the better. Once you start treatment, you may slow down your bone loss so much that you never develop osteoporosis. Some people can reverse osteopenia and regain a typical amount of bone density.
You usually can’t prevent osteopenia. Everyone naturally loses some bone density as they age, and you can’t stop that from happening. Some of the best ways to strengthen your bones and slow bone loss are the same as the treatments for osteopenia. Talk to your provider about ways to improve your bone health if you’re worried about osteopenia or osteoporosis.
Some of the best ways to take care of your bones are great ways to support your overall health:
Visit a healthcare provider if you notice any changes in your body that make you worried about your bone health. Tell your provider about any other symptoms you’re experiencing, especially if you have bone pain or trouble moving.
Advertisement
Ask your provider how often you should have your bone density checked, especially if someone in your biological family has osteopenia or osteoporosis.
You may want to ask your healthcare provider:
Having osteopenia means you have reduced bone density. Some health conditions and medications can cause it or increase your risk, but it usually happens naturally as you age. Most people’s bone density is at its highest around age 25 and slowly decreases over time after that.
Your healthcare provider will tell you how often you’ll need bone density tests, and which treatments can slow down your bone loss. The most important part of treating osteopenia is helping you prevent osteoporosis.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Stiff, painful joints can make daily life challenging. Cleveland Clinic orthopaedic specialists can help you find relief from osteoarthritis and get you moving again.
