Peripheral artery disease, or PAD, is an accumulation of plaque (fats and cholesterol) in the arteries in your legs or arms. This makes it harder for your blood to carry oxygen and nutrients to the tissues in those areas. PAD is a long-term disease, but you can improve it by exercising, eating less fat and giving up tobacco products.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
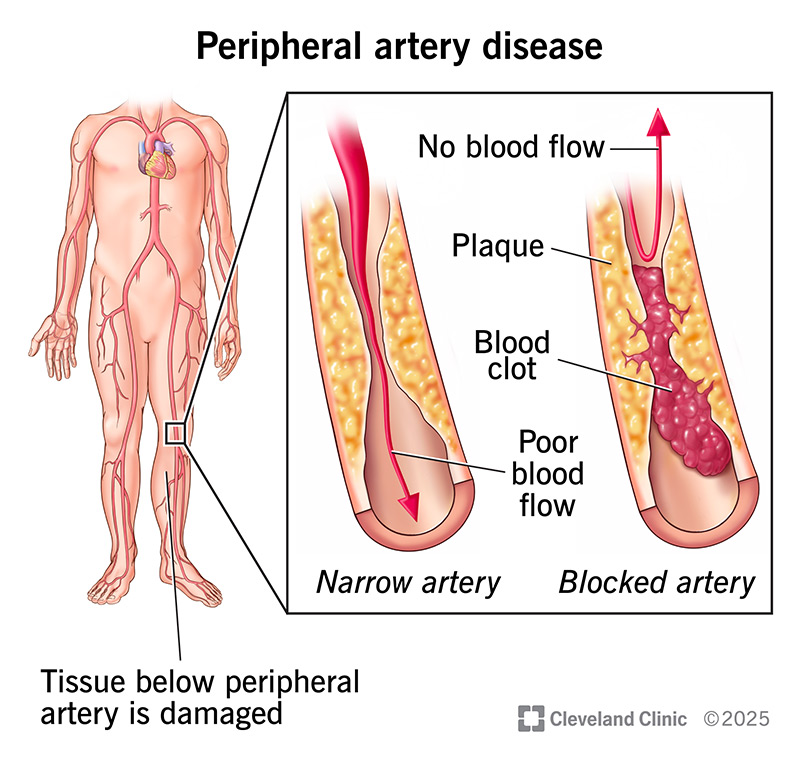
Peripheral artery disease (PAD) is plaque buildup in your leg arteries. Your leg arteries carry oxygen and nutrient-rich blood from your heart to your arms and legs. Other names for this are peripheral vascular disease or peripheral arterial disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Shaped like hollow tubes, arteries have a smooth lining that prevents blood from clotting and promotes steady blood flow. When you have peripheral artery disease, plaque (made of fat, cholesterol and other substances) forms gradually inside your artery walls. Slowly, this narrows your arteries. This is also known as atherosclerosis.
Many plaque deposits are hard on the outside and soft on the inside. The hard surface can crack or tear, allowing platelets (disc-shaped particles in your blood that help it clot) to come to the area. Blood clots can form around the plaque, making your artery even narrower.
If plaque or a blood clot narrows or blocks your arteries, blood can’t get through to nourish organs and other tissues. This causes damage ― and eventually death (gangrene) ― to the tissues below the blockage. This happens most often in your toes and feet.
PAD can get worse faster in some people more than others. Many other factors matter, including where in your body the plaque forms and your overall health.
PAD is common, affecting between 8 and 12 million Americans. However, healthcare providers sometimes don’t diagnose or treat PAD enough. Actual numbers are probably higher.
Advertisement
The typical symptom of PAD is called claudication, a medical term for pain in your leg that starts with walking or exercise and goes away with rest. The pain occurs because your leg muscles aren’t getting enough oxygen.
The dangers of PAD extend well beyond difficulties in walking. Peripheral artery disease increases the risk of getting a nonhealing sore of your legs or feet. In cases of severe PAD, these sores can turn into areas of dead tissue (gangrene) that make it necessary to remove your foot or leg.
Healthcare providers can use two different systems — Fontaine and Rutherford — to assign a stage to your PAD. The Fontaine stages, which are simpler, are:
The first symptom of PAD is usually pain, cramping or discomfort in your legs or buttocks (intermittent claudication). This happens when you’re active and goes away when you’re resting.
Symptoms of peripheral artery disease include:
Half of the people who have peripheral vascular disease don’t have any symptoms. PAD can build up over a lifetime. Symptoms may not become obvious until later in life. For many people, symptoms won’t appear until their artery narrows by 60% or more.
Talk to a healthcare provider if you’re having symptoms of PAD so they can start treatment as soon as possible. Early detection of PAD is important so you can begin the right treatments before the disease becomes severe enough to lead to complications like a heart attack or stroke.
Without treatment, people with PAD may need an amputation — the removal of part or all of your foot or leg (rarely your arm), especially in people who also have diabetes.
Because your body’s circulatory system is interconnected, the effects of PAD can extend beyond the affected limb. People with atherosclerosis of their legs often have it in other parts of their bodies.
Atherosclerosis that develops in the arteries of your legs — or, less commonly, your arms — causes peripheral arterial disease. Like atherosclerosis in your heart (coronary) arteries, a collection of fatty plaque in your blood vessel walls causes peripheral vascular disease. As plaque builds up, your blood vessels get narrower and narrower, until they’re blocked.
Advertisement
Tobacco use is the most important risk factor for PAD and its complications. In fact, 80% of people with PAD are people who currently smoke or used to smoke. Tobacco use increases the risk for PAD by 400%. It also brings on PAD symptoms almost 10 years earlier.
Compared with nonsmokers of the same age, people who smoke and have PAD are more likely to:
Regardless of your sex, you’re at risk of developing peripheral arterial disease when you have one or more of these risk factors:
Although PAD is a different condition from coronary artery disease, the two are related. People who have one are likely to have the other. A person with PAD has a higher risk of coronary artery disease, heart attack, stroke or a transient ischemic attack (mini-stroke) than someone without peripheral artery disease. A person with heart disease has a 1 in 3 chance of having peripheral artery disease in their legs.
Advertisement
Not surprisingly, the two diseases also share some common risk factors. This is because these risk factors cause the same changes in arteries in your arms and legs as they do in your heart’s arteries.
A provider will perform a physical exam and review your medical history and risk factors. They may order noninvasive tests to help diagnose PAD and determine its severity. If you have a blockage in a blood vessel, these tests can help find it:
You may also need an invasive test called an angiogram to find artery blockages.
Yes. Some studies have shown that you can reverse peripheral vascular disease symptoms with exercise and control of cholesterol and blood pressure.
With early diagnosis, lifestyle changes and treatment, you can stop PAD from getting worse. If you think you’re at risk for PAD or may already have the disease, talk to your primary care doctor, vascular medicine specialist or cardiologist so you can get started on a prevention or treatment program right away.
Lifestyle changes, medications and procedures can treat PAD.
The two main goals of peripheral artery disease treatments are:
Advertisement
Treatment of PAD starts with making lifestyle changes to reduce your risk factors. Changes you can make to manage your condition include:
Medicines can help you with conditions such as high blood pressure (antihypertensive medications), high cholesterol (statin medications) and diabetes. These medicines treat the risk factors of PAD and decrease your risk of stroke and heart attack.
Your healthcare provider may prescribe an antiplatelet medication such as aspirin or clopidogrel. They also may prescribe cilostazol to improve your walking distance. This medication helps people with intermittent claudication exercise longer before they get leg pain.
A supervised exercise program will improve the symptoms of pain in your legs with walking, allowing you to walk farther. A structured program typically includes walking on a treadmill in a supervised setting at least three times per week.
People with PAD should also walk at home for a total of at least 30 to 60 minutes every day. The usual prescription is called the “Start/Stop” exercise:
For some people with more severe PAD, leg pain may still cause problems in daily life, even after a few months of exercise and medications. In more severe cases, people need to improve their blood flow to relieve pain at rest or to heal a wound.
More advanced PAD that’s causing severe pain and limited mobility may require endovascular (minimally invasive) or surgical treatment. Some heart disease treatments also treat peripheral artery disease, including:
Complications of PAD treatment
You should contact your healthcare provider if you have these issues after your procedure. They could be signs of an infection or other complications:
How long does it take to recover from treatment for peripheral artery disease?
Depending on the treatment you received, you may spend one night or several in the hospital. You may only need a few days to recover from an atherectomy. But you’ll need a week after an angioplasty. It can take six to eight weeks to recover completely from peripheral artery bypass surgery.
Like most health conditions, PAD is more treatable when a healthcare provider finds it early. Peripheral vascular disease progresses at different rates. This depends on many factors, including where the plaque formed in your body and your overall health.
Peripheral artery disease is a condition you’ll have for the rest of your life. Although there’s no cure for PAD, you can manage it. You can help keep peripheral vascular disease from progressing in several ways:
Knowing that you have risk factors for PAD may motivate you to prevent it. The same advice for keeping your heart healthy applies to caring for your circulation, too:
If you have heart disease, you should discuss your risk factors for PAD with your healthcare provider. Report any symptoms you’re having, such as pain, weakness or numbness in your legs.
It’s important to take good care of your feet to prevent nonhealing sores. Foot care for people who have PAD includes:
In some cases, your healthcare provider may refer you to a podiatrist (foot expert) for specialized foot care ― especially if you have diabetes. A podiatrist can help you with corns, calluses or other foot problems.
Contact your healthcare provider if you:
Get immediate help if you can’t feel or move your foot or if it looks different from your other foot’s skin color. This means you’ve lost blood flow to your leg without warning.
You have the ability to prevent peripheral artery disease (PAD) or keep it from getting worse by making lifestyle changes. Keep all of your follow-up appointments with your healthcare provider and vascular specialist, and take the medicines they prescribe for all of your conditions. Knowing the warning signs of PAD complications helps you know when to ask for help, too.
Plaque in your blood vessels can cause tingling, pain and numbness. Cleveland Clinic’s experts treat circulatory problems, including peripheral artery disease.

Last reviewed on 11/24/2022.
Learn more about the Health Library and our editorial process.