Glomerulonephritis is a kind of kidney disease. It involves damage to your glomeruli, tiny filters inside your kidneys. Some people don’t show any symptoms. Infections and immune system disorders are one of the many causes. Sometimes, glomerulonephritis is mild and goes away without treatment. Other times it leads to kidney failure and other complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
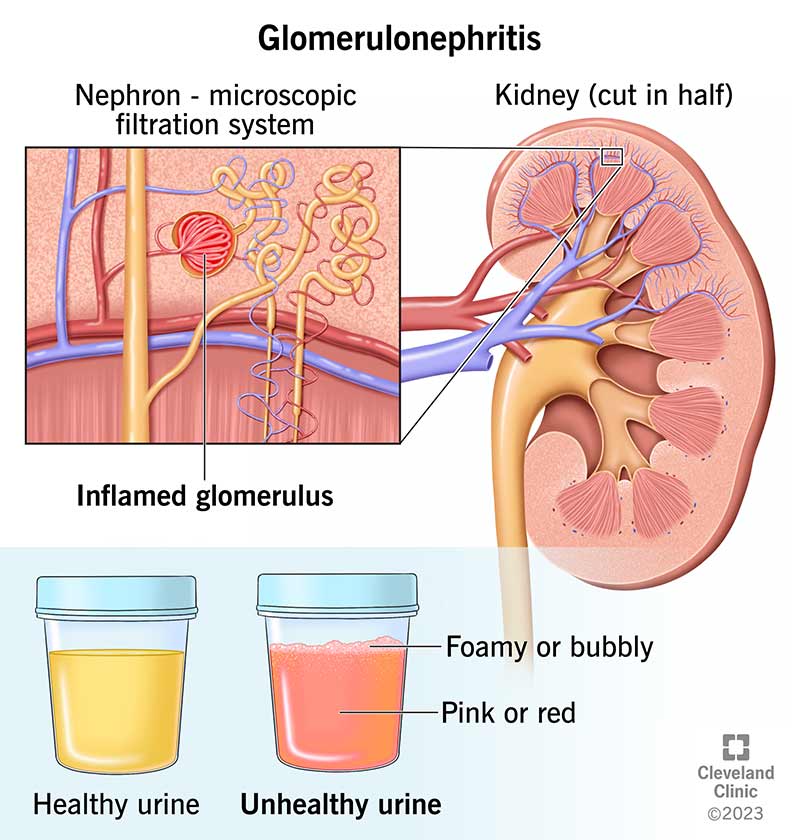
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/16167-glomerulonephritis)
Glomerulonephritis is a type of kidney disease. It involves damage to the glomeruli (tiny filters) inside your kidneys. If you have glomerulonephritis, your kidneys can have trouble removing waste and fluid from your body. Many mild cases resolve with treatment. If the condition becomes severe, it can lead to kidney failure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Glomeruli are tiny filtering units made of capillaries (tiny blood vessels) in your kidneys. You have almost a million of them. Their job is to remove waste and extra fluid from your blood. It’s the first step in the process of making pee. If something damages them, they can’t do their job. This means your kidneys may not work as well.
When glomerulonephritis starts suddenly, it’s called acute glomerulonephritis. When it happens slowly and lasts a while, it’s called chronic glomerulonephritis. Some people can have an acute attack and then a chronic condition years later.
People with glomerulonephritis often don’t experience any warning signs of the disease. But symptoms can include:
Contact a healthcare provider if you have one or more of these symptoms. Many other health conditions can cause similar symptoms. Your healthcare provider can evaluate your symptoms and tell you if glomerulonephritis is a possible diagnosis.
Advertisement
The reason glomerulonephritis appears is often unknown. But causes may include:
Not everyone with risk factors will develop glomerulonephritis. And, not everyone with the condition has a risk factor. But, the following are known risk factors:
Some people develop complications from glomerulonephritis. Glomerulonephritis affects your kidney’s ability to remove waste from your bloodstream. Specific complications include:
Glomerulonephritis may not produce symptoms. That’s why it’s often discovered during tests for another concern. If a healthcare provider suspects you have glomerulonephritis, they may refer you to a kidney specialist and/or you may have the following tests:
Advertisement
Treatment depends on what’s causing the condition and if you have kidney damage. The goal of treatment is to reduce any further damage.
Sometimes, treating the underlying cause, like taking medication to manage high blood pressure, is all that’s necessary. If the cause is due to infection, antibiotics can treat the infection.
At other times, your healthcare provider may recommend:
Different people have different outcomes with glomerulonephritis depending on what kind of glomerulonephritis you have. Some cases go away over time without any treatment. Some people have no symptoms of the disease and only find out because they have a blood or urine test for another condition. But it can cause kidney damage and lead to kidney failure without treatment.
Advertisement
There’s no proven way to prevent glomerulonephritis. Adopting a healthy lifestyle is the best approach, though some practices may help, such as:
If you have glomerulonephritis, get your kidneys checked on a regular basis. Follow medical advice and take medication as prescribed by your provider to manage the cause. You also may have to limit the amount of salt and protein you eat. These ingredients put stress on your kidneys.
It can lead to kidney disease or kidney failure in some people. Both of these conditions are serious. It’s important to see your healthcare provider each year so they can be made aware of changes in your body or health history. This can help them detect conditions like glomerulonephritis, which causes no symptoms in some people.
Contact your healthcare provider if you have symptoms like:
Advertisement
Consider asking your healthcare provider:
Many people with glomerulonephritis don’t have symptoms. That’s why it’s important to see a healthcare provider regularly. They can detect when something seems off based on doing examinations and looking at your health history. Some causes of glomerulonephritis are within your control. These include practicing safe sex and seeking medical attention if you believe you have an infection. If you receive a glomerulonephritis diagnosis, treatment depends on the cause and how severe the condition is. Certain strategies can help keep your kidneys healthy and avoid further damage. Be sure to discuss any questions or concerns you have with your provider.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you need treatment for glomerulonephritis, the kidney specialists at Cleveland Clinic are there to help guide you through every step of your journey.
