Graves’ disease is an autoimmune disease that affects your thyroid gland. The gland produces too much thyroid hormone, a condition known as hyperthyroidism. An overactive thyroid causes problems with your heart and bones. Treatments can help.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Graves’ disease is a lifelong (chronic) autoimmune disease that causes your thyroid to make too much thyroid hormone. It happens because your body makes antibodies to your thyroid gland.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s one of the most common causes of hyperthyroidism (overactive thyroid), especially if you have a family history of thyroid problems. Graves’ disease mainly affects your thyroid. But it can also affect your eyes and skin.
Graves’ disease speeds up your metabolism. This can affect several aspects of your health. You may not feel like yourself or even feel out of control of your body. It’s important to get medical treatment if you develop signs of this condition.
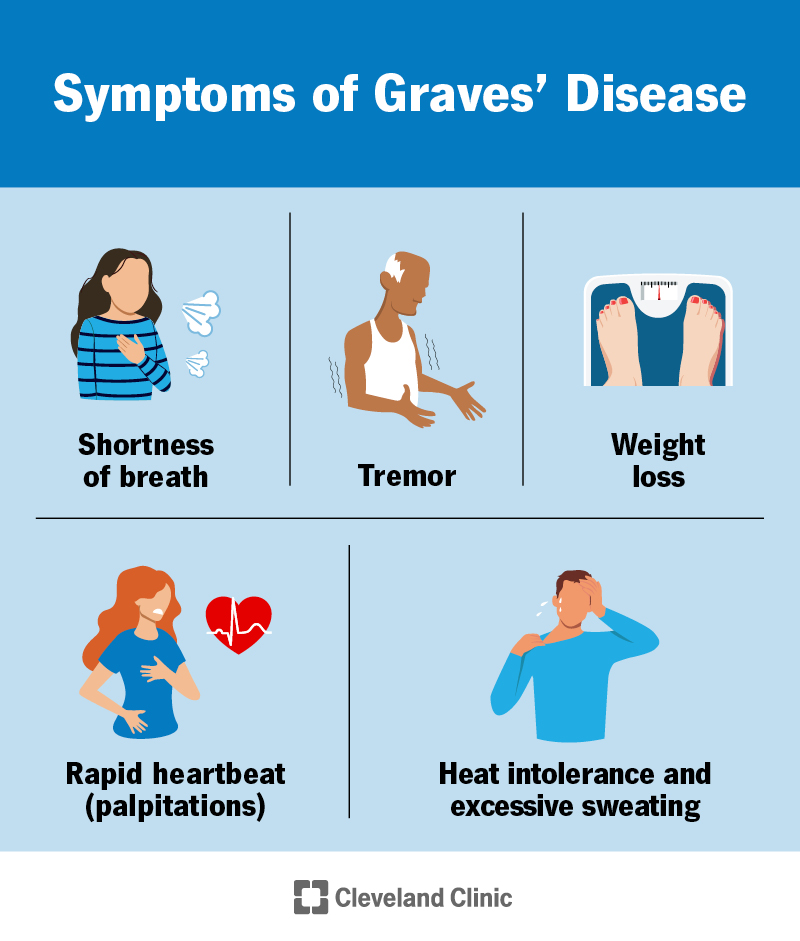
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/15244-graves-disease)
Symptoms of Graves’ disease (and hyperthyroidism) include:
The onset of Graves’ disease symptoms is usually gradual. It often takes several weeks or months to develop. But sometimes, it develops suddenly over a few days. You may experience some of these symptoms or many at the same time.
See your healthcare provider if you have symptoms. Graves’ disease needs to be treated.
Graves’ disease can also cause eye issues, like:
Advertisement
This is called Graves’ orbitopathy or thyroid eye disease. About 1 in 3 people with Graves’ disease develop it.
Up to 4% of people with Graves’ disease develop pretibial myxedema (Graves’ dermopathy). It causes a lumpy, discolored thickening of your skin — usually on your legs.
About 1% of people with Graves’ disease have thyroid acropachy. This causes clubbing of your fingers and toes.
Graves’ disease happens when something triggers your immune system to overproduce an antibody called thyroid-stimulating immunoglobulin (TSI). TSI attaches to healthy thyroid cells, causing your thyroid to overproduce thyroid hormones.
In one study, researchers estimated that your genes contribute to 79% of your risk of developing Graves’ disease. This means that Graves’ disease is partially hereditary. The remaining percentage of risk (21%) is due to environmental factors.
Scientists don’t know exactly why your immune system attacks your thyroid. But they think the trigger may happen due to environmental factors, like:
Risk factors for Graves’ disease include:
Untreated or undermanaged Graves’ disease increases your risk of the following complications:
Graves’ disease may also increase your risk of thyroid cancer.
Untreated Graves’ disease during pregnancy can be harmful to you and the fetus. It can increase the risk of:
Your healthcare provider will ask about your symptoms and medical history. This includes your family history of thyroid disease. They’ll also do a physical exam.
Advertisement
They may also recommend the following tests to confirm a Graves’ disease diagnosis:
Graves’ disease is a lifelong (chronic) condition. But treatments can keep your thyroid hormone levels in check. Medical care may even make the disease temporarily go away (remission).
Treatments for Graves’ disease include:
Advertisement
Radioiodine therapy and thyroidectomy usually lead to hypothyroidism (underactive thyroid). If you develop this condition, you’ll need to take thyroid replacement hormone medications for the rest of your life. But hypothyroidism is easier to treat than hyperthyroidism. It causes fewer long-term health problems.
All the Graves’ disease treatment options have benefits and risks. And there’s no agreement in the medical community on which treatment is the best. It’s important to discuss all the options in detail with your provider to make the best choice for you.
Researchers are currently studying antigen-specific immunotherapy as a treatment for Graves’ disease. Ask your healthcare provider if a clinical trial is an option.
You’ll need to see your healthcare provider regularly throughout your life. They’ll make sure your thyroid levels are in check and your treatment plan is working. If you develop any new symptoms, talk to your provider.
If you’re experiencing symptoms of thyroid storm, call 911 (or your local emergency service number) or get to the nearest emergency room (ER) as soon as possible. Thyroid storm is life-threatening.
If Graves’ disease is properly treated, the prognosis (outlook) is generally good. Without treatment, Graves’ disease can cause complications that can affect your overall health or life expectancy.
Advertisement
Getting a new diagnosis can be stressful. The good news is that Graves’ disease is a manageable and treatable condition. If you have symptoms or certain risk factors, like a family history of thyroid disease, contact your healthcare provider. They can recommend some simple tests to see if your thyroid is making too much thyroid hormone.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s experienced healthcare providers treat all kinds of thyroid disorders, including issues that cause hypothyroidism and hyperthyroidism.
