Bone fractures are a very common injury and can affect anyone at any age. Anyone can break a bone. But you’ll have a much higher risk if you have osteoporosis. There are lots of fracture types, and several ways to treat them. You might only need a splint or cast. More serious breaks require surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
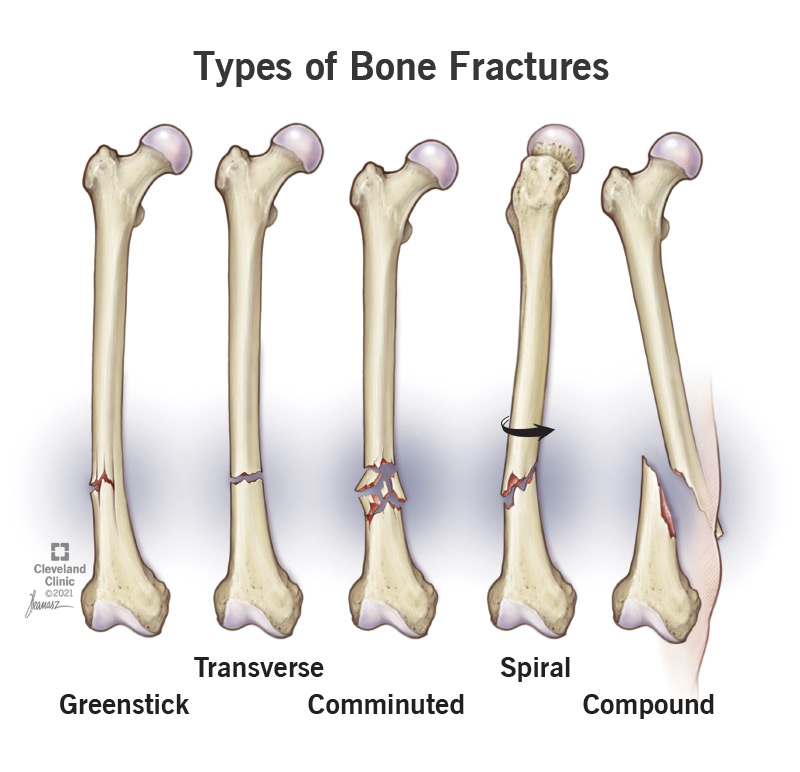
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/15241-bone-fractures-2)
A bone fracture is the medical definition of a broken bone. You might see these names used interchangeably.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Traumas like falls, car accidents and sports injuries cause most fractures. But some health conditions or repetitive motions (like running or doing physical work) can lead to broken bones, too.
You’ll need to wear a splint, cast or brace to hold your broken bone stable while it heals. Some fractures need surgery to repair them.
Go to the emergency room if you think you have a broken bone. Try to hold that part of your body stable and don’t use it. Call 911 (or your local emergency services number) if you experience a severe trauma like a car accident.
There are lots of different types of fractures. Healthcare providers classify them in a few ways.
Some fractures are named for their patterns. This means the shape of the break or what it looks like, including:
Providers classify some broken bones by how they happened, including:
Advertisement
Your provider might diagnose a fracture as open or closed, in addition to giving it a name. If you have an open fracture, your bone breaks through your skin. Open fractures are sometimes referred to as compound fractures. They usually take longer to heal. They also have an increased risk of infections and other complications. Closed fractures are still serious, but your bone doesn’t push through your skin.
Displaced or non-displaced are other words your provider will use to describe a fracture. A displaced fracture means the pieces of your bone moved so much that a gap formed around the fracture when your bone broke. Displaced fractures are much more likely to require surgery to repair. Non-displaced fractures are still broken bones. But the pieces didn’t move far enough to be out of alignment.
Symptoms of bone fractures include:
Traumas are the most common cause of broken bones. Anything that hits one of your bones with enough force can break it. Some of the most common causes include:
It’s possible to fracture a bone without experiencing trauma or a single injury. For example, repetitive forces like running or practicing a sport can put lots of pressure on your bones. Over time, this can cause stress fractures.
You’re much more likely to break a bone if you have osteoporosis. It’s especially common in females. Talk to a healthcare provider about a bone density scan if you’re over 65.
Anyone can break a bone, but your work and hobbies can increase your risk. If you repeat one movement or motion a lot, you might develop overuse syndrome. This can increase your risk of breaks in your fingers, hands and wrists. Similarly, playing contact sports can increase your overall fracture risk.
Broken bones can develop a few complications while they heal, including:
The injuries that cause broken bones can affect your other tissue, too. Muscles, nerves, tendons, ligaments and blood vessels can be damaged during an injury. The pieces of your broken bone can also damage tissue when they’re pushed out of place.
A healthcare provider will diagnose a bone fracture with a physical exam and imaging tests. In some cases, they do this in the emergency room if you’re admitted after a trauma.
If you’re taken to the ER, a team of providers will stabilize you and treat your injuries in the order of severity. Especially if some are life-threatening. After you’re stabilized, you’ll need imaging tests to confirm any fractures.
Advertisement
You’ll need at least one of a few imaging tests to take pictures of your bones:
How healthcare providers treat a fracture depends on which type it is, what caused it and how damaged your bones are. Bone fracture treatments include:
Advertisement
Most people who break a bone make a full recovery. You should be able to resume all your usual activities after your bone heals. Some fractures can have a long-term impact on your life, especially if you experienced other injuries. Talk to your surgeon or healthcare provider before resuming any physical activities or playing sports. They’ll tell you when it’s safe to start using your bone normally.
How long it takes a bone fracture to heal depends on a few factors, including:
Depending on which type of immobilization or surgery you needed to repair your fracture, you should be able to start moving again in a few weeks. More severe fractures can take a year or more to heal.
Talk to your provider or surgeon about what to expect while you’re recovering. Contact your provider right away if you experience intense pain that doesn’t get better.
Even though bone fractures are common injuries, they’re still scary. If you break a bone, talk to your provider or surgeon about what to expect. Most people make full recoveries and can return to their pre-injury routine and activities with no long-term impacts.
Advertisement
Don’t rush your recovery. Giving your body the time it needs to get better can be frustrating, but it’s the best way to make sure you don’t reinjure your bone while it heals.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Need care fast? Cleveland Clinic’s Express Care and Urgent Care locations treat everything from sprains to sinus infections — no appointment needed.
