Porphyria refers to a group of disorders (often genetic) that affect your nervous system and/or skin. Acute porphyrias cause painful attacks that can last days or weeks. Cutaneous porphyrias make your skin sensitive to light and cause symptoms like pain, swelling and blisters. Treatment can help manage and prevent symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Porphyria” (pronounced “por-FEER-ee-uh”) is an umbrella term for a group of rare diseases that affect how your body makes heme (pronounced “heem”). Heme is a building block for the hemoglobin in your blood. Heme carries oxygen to tissues throughout your body and gives red blood cells their color. Heme is also important for many other functions and processes in our cells.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Heme production is an eight-step process. It requires the right amount of eight different enzymes (one for each step), as well as chemicals called porphyrins and porphyrin precursors. When an enzyme isn’t doing what it’s supposed to, there’s a ripple effect. Porphyrins and precursors build up in your body’s cells, leading to symptoms and possible complications.
You might wonder why enzymes aren’t doing what they’re supposed to. Usually, this is due to a change in a gene that serves as a blueprint for one of the enzymes in the heme production pathway. Porphyria is often inherited. This means a gene change affecting heme production can be passed down within biological families, putting other family members at risk of also developing porphyria or being disease carriers.
Healthcare providers can help you diagnose, manage — and possibly prevent — symptoms to lessen the impact of these conditions on your life.
There are eight types of porphyria. Providers refer to these together as “the porphyrias.” Your provider will diagnose you with a specific type based on your symptoms and where in your body the excess chemicals build up.
In general, the porphyrias fall into two groups according to their symptoms:
Advertisement
These diseases cause severe attacks of abdominal pain and other symptoms. Some acute porphyrias also cause your skin to react to sunlight with blistering rashes.
Acute porphyrias include:
These diseases cause skin symptoms that can include pain, discoloration, swelling and/or blistering with sun exposure. Depending on the underlying cause, people have either a blistering or a non-blistering cutaneous porphyria.
Blistering cutaneous porphyrias include:
Non-blistering cutaneous porphyrias include:
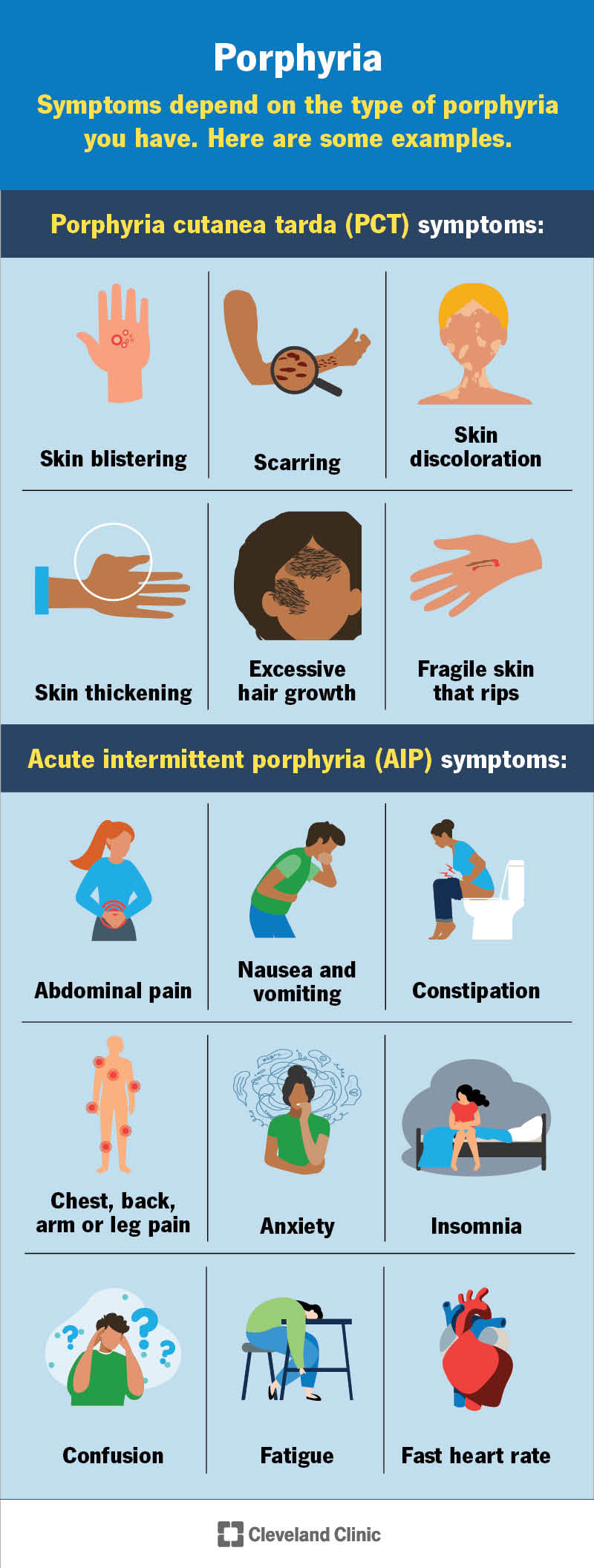
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/17760-porphyria.jpg)
The specific symptoms you experience — and how long they last — depend on the type of porphyria you have. Symptoms range from mild to severe. Some people with porphyria have no symptoms. In some cases, symptoms can be life-threatening unless treated.
An elevation of heme precursors called aminolevulinic acid (ALA) and porphobilinogen (PBG) causes acute porphyrias. These substances affect how your nervous system works. Your nervous system controls everything from muscle movement to digestion. Porphyria disrupts nervous system activity, causing symptomatic “attacks.”
Possible symptoms during an acute porphyria attack include:
Advertisement
If you have hereditary coproporphyria or variegate porphyria, your skin may be sensitive to sunlight. Sun exposure may cause you to develop a blistering rash, skin color changes and/or scarring.
An attack might last for three to seven days. But it’s possible for it to last much longer — especially if untreated —and symptoms can take weeks to months to resolve. You might have one or just a few attacks throughout your life. But it’s also possible to have multiple attacks within a single year.
Long-term complications of acute porphyria include high blood pressure, kidney failure and in rare cases liver cancer.
Cutaneous porphyrias cause skin symptoms when you’re exposed to sunlight. This includes direct exposure outside, as well as sunlight that comes at you through windows. Some types of artificial light can also cause symptoms. These types of porphyria don’t cause sudden, severe abdominal pain or the other symptoms typical of acute “attacks.”
You’ll likely feel tingling as the first sign of a reaction to the sun and develop what providers call a “phototoxic reaction” if you don’t get out of the sun. You’ll experience the following skin symptoms, especially on your face, hands and feet:
Advertisement
These reactions are very painful and usually last two to five days. You need to stay inside and try to cool the affected areas (for example, with cold air from an air conditioner).
People with PCT can have the following symptoms:
This severe type of porphyria starts showing symptoms shortly after birth or at a very young age. The first visible sign is usually red urine. Babies tend to have red-stained diapers, often prompting providers to test for a urinary tract infection.
Other CEP signs and symptoms include:
Changes in certain genes cause acute porphyria. But just because you inherit a gene change doesn’t mean you’ll develop symptoms of porphyria. Most people with gene changes associated with porphyria don’t develop symptoms. This means genetic testing isn’t sufficient to confirm a diagnosis. The only way to determine if your symptoms are caused by acute porphyria is to check ALA and PBG levels in your urine.
Advertisement
Experts think other factors, like hormones, medications and things you eat or drink, play an important role in causing acute attacks. If you’re born with a gene change linked with acute porphyria, these other things trigger attacks.
Known triggers include:
PCT occurs mostly in adults and is one type of porphyria that’s a bit different. It often has what providers call “acquired causes.” This means you can develop this condition even if you don’t inherit a gene change.
Usually, two or more risk factors combine to disrupt normal heme production. Such factors include:
Healthcare providers diagnose porphyria by doing a physical exam and running lab tests. You may need one or more of the following tests:
Your provider will explain which tests you need and what each test can reveal. Your provider may recommend genetic testing for you and your biological family members. This can identify specific gene changes known to cause porphyria.
Treatment depends on the type of porphyria you have and how it affects you. Your provider will help you understand what’s best in your unique situation. Here’s an overview of what you might expect.
If you have acute porphyria, you may need care at a hospital when an attack occurs. At the hospital, providers will do one or more of the following:
Your provider may prescribe a medication called givosiran to help prevent future attacks. This is an injection you receive every month to suppress the overproduction of ALA and PBG.
You may need to avoid the following trigger factors:
No matter the specific type of cutaneous porphyria you have, protecting your skin is vital to preventing symptoms. Sunscreen typically isn’t enough. Ideally, you should avoid being in the sun at all. If you must do so, wear sun-protective clothing. Your provider can advise you on what’s best. You may also need to avoid certain artificial lighting.
Your provider may prescribe afamelanotide. This is a tiny implant your provider puts just under your skin in your abdominal area. The implant releases medicine that can help reduce painful symptoms of sun exposure. Your provider will also monitor your liver function regularly and make sure that your vitamin D level isn’t too low.
Gallstones occur more frequently in EPP/XLP. Some people with EPP/XLP can also develop liver abnormalities. In severe cases, liver failure may develop. This may require a liver transplantation, sometimes followed by a bone marrow transplantation.
Your provider may prescribe:
Strict protection from sun and fluorescent light exposure is extremely important to avoid skin blistering and complications. If skin blistering happens, antibiotic creams may be necessary. You may need oral or IV antibiotics if the infections are severe.
Your provider will monitor your hemoglobin level regularly to decide if a blood transfusion is necessary. In people who are severely affected, a bone marrow transplant may be necessary, which is the only way to cure the disease.
When you have porphyria, follow-ups become a routine part of your life. Your healthcare provider will tell you when to come in for appointments. These are important for monitoring how the disease is affecting your body and catching signs of complications. You’ll likely need routine lab tests (blood and pee), along with other tests to check organ function.
Your outlook depends on:
Your healthcare provider can give you the most accurate sense of what you can expect going forward.
Porphyria might have a big impact on your day-to-day life. Severe symptoms can interrupt your routine and make it hard to work, take care of your family or enjoy hobbies. You might feel exhausted, physically and mentally.
Let your provider know how you’re feeling. They can suggest resources and support groups. Connecting with porphyria communities can help you learn more about your condition and ways to manage it.
Living with a rare disease like porphyria can be isolating, frustrating and downright scary. You might wish family and friends could understand how you’re feeling. Maybe you’re simply tired of having to explain porphyria to others and why you can’t do certain things.
Wherever you’re at, know you’re not alone. Even though porphyria is rare compared to many other diseases, there’s still a whole community waiting to support you. Connect with porphyria support groups online or ask your provider to put you in touch. Finding people who understand how you’re feeling can help make the ups and downs a lot easier to manage.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Do certain health conditions seem to run in your family? Are you ready to find out if you’re at risk? Cleveland Clinic’s genetics team can help.
