Sinus bradycardia is a heart rhythm where your heart beats slower than expected (under 60 beats per minute for adults) but otherwise works normally. It’s fairly common, especially in adults over 65 and those who exercise regularly. It’s usually not serious unless you have symptoms. It’s typically treatable with medications or a permanent pacemaker.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
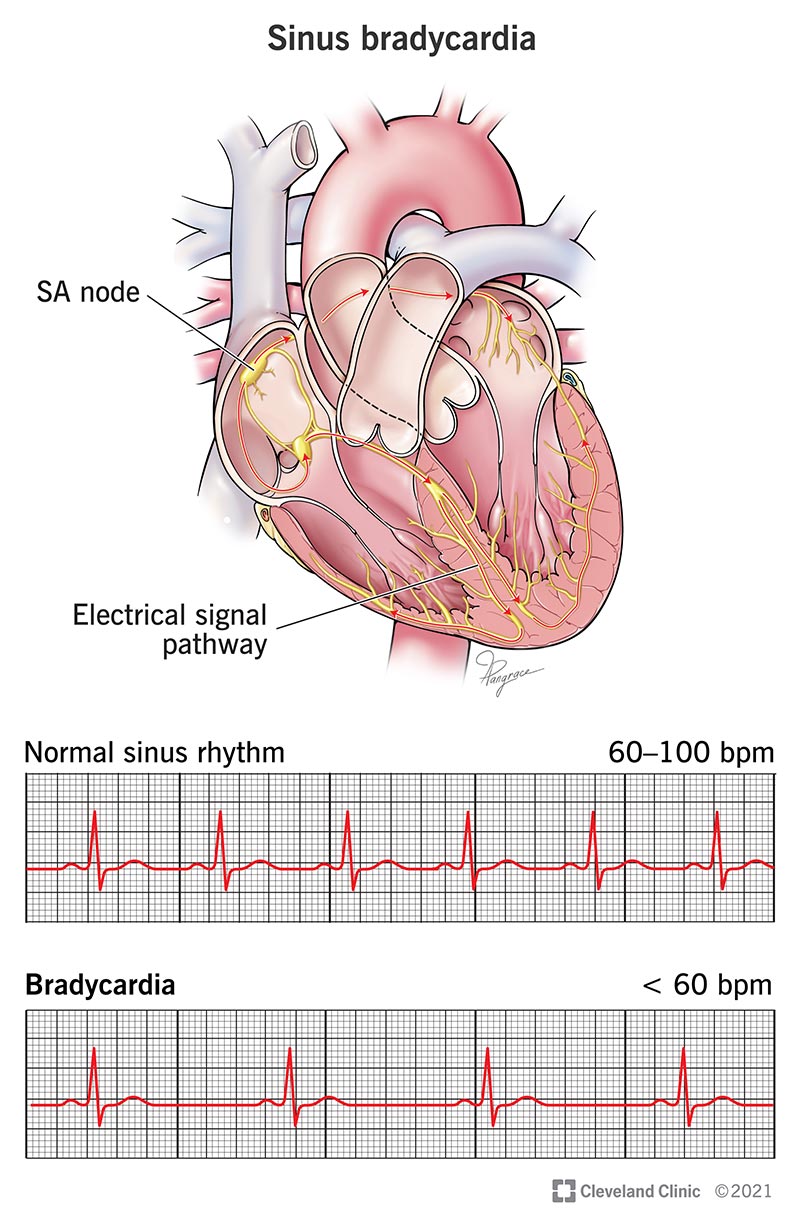
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22473-sinus-bradycardia)
Sinus bradycardia is a heart rhythm that’s slower than expected (fewer than 60 beats per minute in an adult) but is otherwise normal. It’s sometimes a symptom of certain heart conditions or problems, but it can also be a sign that a person is in very good shape because of regular exercise.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Most people don’t have symptoms, but when symptoms do happen, it’s usually because your heart is pumping too slowly to supply your body with enough blood.
The term “sinus bradycardia” breaks down based on the two words. Bradycardia comes from the Greek words “bradys,” meaning “slow,” and “kardia,” meaning “heart.” Sinus bradycardia means your heart is beating slowly but still using a sinus rhythm.
During sinus rhythm, every heartbeat you have starts in the sinoatrial (SA) node, a cluster of electrically active cells near the top of your heart. The SA node (also known as the sinus node) is your heart’s natural pacemaker and generates the electrical current that makes your heart muscle squeeze. Sinus rhythm means your sinus node is setting the tempo for your heartbeat, which is normal and expected.
Sinus bradycardia tends to happen in adults, especially those over age 65, as your heartbeat tends to naturally slow down as you age. Sinus bradycardia is less likely to occur in children (but still possible in rare cases) unless it happens because of a condition that a child has when they’re born (congenital).
Sinus bradycardia also happens normally to people who exercise regularly and are in very good physical condition. Regular exercise and training have a positive effect on your vagus nerve. This nerve, which has a direct connection to your brain, is part of your autonomic nervous system. The better your vagus nerve works, the lower your resting heart rate.
Advertisement
Sinus bradycardia with symptoms happens in about 1 out of every 600 adults over age 65. However, most people with this condition don’t have symptoms, especially because it’s common in very active people. That means the true number is unknown, but is almost certainly much higher.
Most people with sinus bradycardia don’t have symptoms, making this a benign (harmless) condition. Many people may not even know their heart rate is under 60 beats per minute unless they have a reason to check their pulse.
For people who have symptoms, sinus bradycardia is a sign that their body isn’t pumping enough blood. That means their brain and body aren’t getting enough oxygen, and that lack is the usual driving force behind symptoms.
For most people, sinus bradycardia doesn’t cause any symptoms. This is especially true for people who’re very physically active and have sinus bradycardia because their hearts are more efficient.
For others, symptoms of sinus bradycardia may include:
Sinus bradycardia can happen in connection with a number of factors.
Advertisement
Other conditions include:
Sinus bradycardia isn’t contagious, meaning you can’t pass it from person to person. However, some infections that can eventually lead to sinus bradycardia — such as strep throat — are contagious.
A healthcare provider, usually your doctor, can diagnose sinus bradycardia using a combination of diagnostic tests and methods.
While a physical exam alone is enough to diagnose sinus bradycardia, it’s only possible with a specific type of test called an electrocardiogram (ECG or EKG). That’s because analyzing your heart’s electrical activity is the only way to know that your heart rhythm is otherwise normal.
EKGs analyze your heart’s electrical activity through several sensors called electrodes, which stick to the skin of your chest. These electrodes then display the electrical power of your heartbeat as a wave on a paper printout or a screen. Healthcare providers look at the wave for signs that your heart’s electrical system isn’t working properly. If your heartbeat is slow but otherwise normal, that’s all a doctor needs to diagnose sinus bradycardia.
Advertisement
But if you have symptoms of sinus bradycardia, it’s important to know why. To answer that question, several other types of tests are possible.
While other tests can help determine the cause of your sinus bradycardia, your healthcare provider will be the best person to explain what tests they think you need. They can also tell you more about how the specific tests work and why they think those tests are necessary.
Sinus bradycardia usually doesn’t need treatment unless you have symptoms. This is especially true if you have sinus bradycardia because you’re in good physical condition and exercise regularly.
Advertisement
Treating sinus bradycardia can happen in two main ways for people who have symptoms: Medication or devices that use electrical energy to artificially stimulate your heart muscle (commonly known as pacemakers).
When your sinoatrial node (SA) — your heart’s natural pacemaker — isn’t working as it should, there are artificial ways to get the same effect. Permanent pacemakers, devices that a cardiologist or surgeon can implant in your chest, can deliver an electric current to make your heart beat properly. Those devices can last for over a decade and deliver regular electric pulses that are just powerful enough to simulate the same effect from your SA node.
In some cases, there’s also a short-term method that uses the same principles. That method, temporary pacing, uses a device that sends electrical pulses into your body through pads attached to your skin, or through a temporary wire inserted into your heart. This is usually an option when you need a permanent pacemaker but have to wait to undergo surgery to have it implanted.
For some people, a new type of pacemaker device is an appropriate and better option. Leadless pacemakers are implantable using a catheter-based procedure. During this procedure, your healthcare provider makes a small incision above a major blood vessel (usually one near the top of your thigh) and inserts the catheter. They then thread that tube-like device through your blood vessels and up to your heart. Once there, they can implant the leadless pacemaker — which is about the size of a large multivitamin — directly inside the right ventricle of your heart.
Medication may be an option depending on the cause of your sinus bradycardia — especially if that cause means it’s likely a temporary problem. Intravenous (IV) and injectable medications like atropine can speed up your heart rate for a short time.
Your healthcare provider is the best person to tell you what side effects to expect from any treatments, medications or procedures to treat your sinus bradycardia. Sinus bradycardia usually doesn’t have complications unless it’s severe enough to cause symptoms, and the risk of complications is higher when you wait too long to get it treated.
Because sinus bradycardia requires an EKG to diagnose, it’s not something you should assume you have based on symptoms alone. The best course of action is to see your healthcare provider if you have sinus bradycardia symptoms. They can diagnose this condition and determine if it’s severe enough to need treatment.
You should start feeling better soon after you receive effective treatment for sinus bradycardia (either medications or temporary pacing). If you need a permanent pacemaker, you should start feeling better after that surgery (especially after you recover from the surgery itself). If you have surgery to implant a pacemaker, most people recover within a few weeks.
Regardless of which treatments you receive, your healthcare provider is the best person to tell you how long it should take you to recover and what you can expect. That’s because they can take into account your unique circumstances and situation.
Most people who have sinus bradycardia won’t have symptoms, and it won’t affect your life in any way that you can see. If you have symptoms, quick diagnosis and treatment can make a big difference in how this condition affects you, though.
Sinus bradycardia can be a short-term problem, especially when it happens because of prescription or recreational drugs or other short-lived circumstances. When other conditions cause it, especially conditions you have when you’re born or inherited from your parents, it’s usually a life-long problem. In those cases, you’ll need to either take medication daily or have a pacemaker implanted to avoid symptoms and related problems.
For the most part, it isn’t possible to prevent sinus bradycardia. What you can do is act to avoid circumstances that make sinus bradycardia more likely to happen. These include:
If your healthcare provider diagnoses you with sinus bradycardia and you have symptoms, you should see your healthcare provider as recommended and take medications as prescribed. If you have a pacemaker implanted, you should also see your healthcare provider as recommended so they can make sure your pacemaker is working correctly (healthcare providers can check almost all modern pacemakers using wireless technology, making this part of the visit painless and easy).
If you have sinus bradycardia without symptoms, you should still see a healthcare provider for an annual physical. These yearly visits are a key way to detect new problems before they become severe enough to cause symptoms.
If you have sinus bradycardia with symptoms, you should see your healthcare provider if your symptoms change noticeably or if your symptoms start to affect your daily life and routine.
Because sinus bradycardia shares the following symptoms with other more serious heart conditions, you should go to the hospital if you experience:
Sinus bradycardia is a condition you may not even know you have, and for most people, it doesn’t cause any symptoms. When it does cause symptoms, your healthcare provider can help you find out why it’s happening and if it’s a cause for concern. Fortunately, for people who do need treatment, this condition is often very treatable, and it shouldn’t have a big impact on your daily life overall.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart rhythm is out of sync, the experts at Cleveland Clinic can find out why. We offer personalized care for all types of arrhythmias.
