Rheumatic heart disease (RHD) is a condition with heart valve damage from rheumatic fever. This can happen after an untreated strep infection. You may be at risk for RHD if you don’t have access to antibiotics. The condition can lead to serious health problems like heart failure. Medication and surgery are the main treatments, but not a cure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
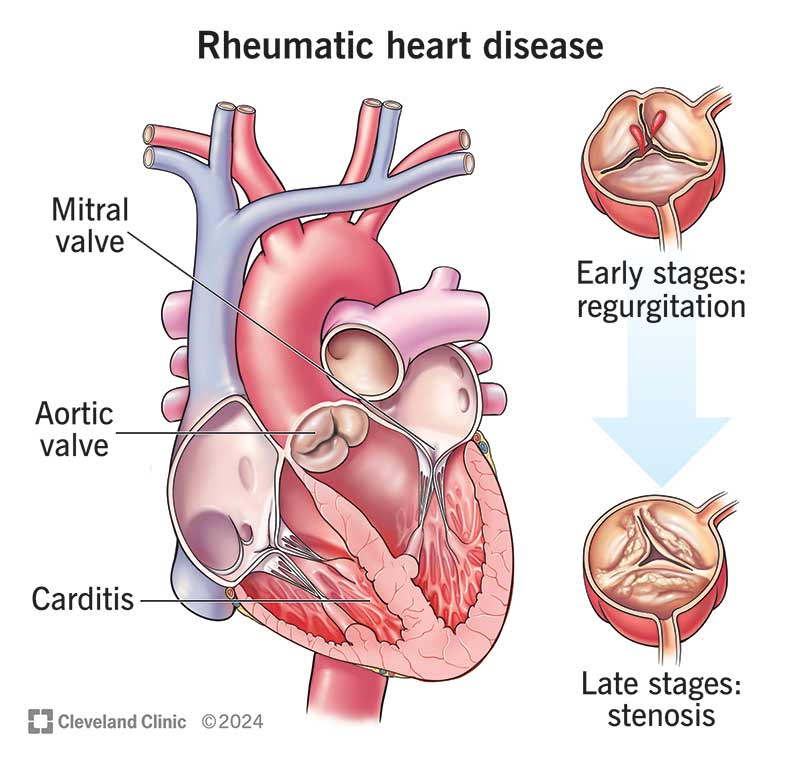
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/rheumatic-heart-disease.jpg)
Rheumatic heart disease (RHD) is heart valve damage from rheumatic fever. Bacterial infections from group A Streptococcus can cause rheumatic fever. An infection like strep throat or scarlet fever triggers your body’s immune response, causing inflammation throughout your body, including in your heart.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Inflammation from rheumatic fever can lead to permanent damage to your heart valves. Damaged valves reduce the amount of blood that can move through your heart. They also may allow some blood to go in the wrong direction.
Rheumatic heart disease is rare in the U.S. It’s more common in parts of the world with limited access to antibiotics. About 306,000 people worldwide die of rheumatic heart disease each year. More than 40 million people in the world have RHD.
Children and teenagers with untreated strep are the most likely to get rheumatic fever, often between ages 5 and 15. Signs of heart damage can develop years after the infection and fever are gone. People often show signs of rheumatic heart disease, like chest pain or shortness of breath, as young adults. Treatment includes medicines, procedures and surgery.
Some people may have symptoms of heart involvement while they’re sick with rheumatic fever. But in most cases, rheumatic heart disease symptoms may not appear until years after a strep infection or rheumatic fever. People with heart damage may experience these signs and symptoms of RHD:
Advertisement
Heart valve inflammation from rheumatic fever causes rheumatic heart disease. The damage may happen right away. Or it can develop over time from repeated strep infections. Continuing inflammation leads to heart valve scarring and narrowing.
RHD isn’t contagious. But strep throat is. It can lead to rheumatic fever, the cause of RHD.
If you’re at risk of rheumatic heart disease, you may need penicillin injections every three to four weeks for five or more years. This can also keep rheumatic heart disease from getting worse by preventing the disease that causes rheumatic fever.
You’re at a higher risk for RHD if you:
Rheumatic fever can affect your heart about 20 or 30 years after you've had an episode of it. If you had repeated episodes or were younger when you had rheumatic fever, you may see the effects of rheumatic heart disease at a younger age.
One or more of your heart valves can grow narrow (valve stenosis) or allow blood to flow backward in the wrong direction (regurgitation). Rheumatic heart disease tends to affect the mitral and aortic heart valves.
Rheumatic heart disease can lead to:
Some of these conditions can increase your risk of a stroke or blood clots.
Rheumatic heart disease is especially dangerous if you're pregnant. Pregnancy increases the amount of blood in your body. Your heart has to work harder to pump the extra blood. This means a woman with damaged heart valves can have serious health issues during pregnancy. The fetus's health is also at risk.
If you know that you have a rheumatic heart valve, discuss pregnancy with your healthcare providers.
To diagnose rheumatic heart disease, a healthcare provider will assess your symptoms and perform a physical exam. They’ll also review your health history, especially any history of fevers or bacterial infections.
Your provider may use the following tests to diagnose RHD:
Advertisement
Rheumatic heart disease treatments can help you manage symptoms and may delay disease progress. But they can’t cure the condition. Treatments include:
Visit your provider regularly to monitor your health. They can make sure you get antibiotics to prevent or treat strep throat.
Contact your provider if you experience new or worsened symptoms, including:
The right treatments may delay or prevent heart failure in people with rheumatic heart disease. But the disease is permanent and requires long-term care. Without regular checkups, rheumatic heart disease can lead to severe heart failure. Lack of treatment can be fatal.
Advertisement
RHD is highly treatable if providers recognize it and do follow-ups. A valvuloplasty can be curative.
The length of time that you can live with RHD depends on how severe it is at diagnosis. In a study of indigenous people in Australia under 25, those who had severe rheumatic heart disease at diagnosis got worse fairly quickly. Some people with moderate disease improved, while others stayed the same or got worse. Ten years after diagnosis, 6 out of 10 people with mild rheumatic heart disease didn’t get worse.
It’s hard to hear that an illness you thought you’d recovered from long ago left lasting damage. But there are steps you can take now to manage rheumatic heart disease. Take charge of your health by talking with a healthcare provider about the best ways to treat your heart issue and stay safe from another infection. The best thing you can do for your health is to follow a provider’s advice for staying healthy.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your heart needs some help, the cardiology experts at Cleveland Clinic are here for you. We diagnose and treat the full spectrum of cardiovascular diseases.
