Familial hypercholesterolemia (FH) is a genetic disorder that increases your risk of heart disease at a younger age than usual. Treatments like cholesterol-lowering medications and changes in what you eat can cut down your risk by more than half. Letting your family know you have FH gives them the chance to get tested and receive early treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
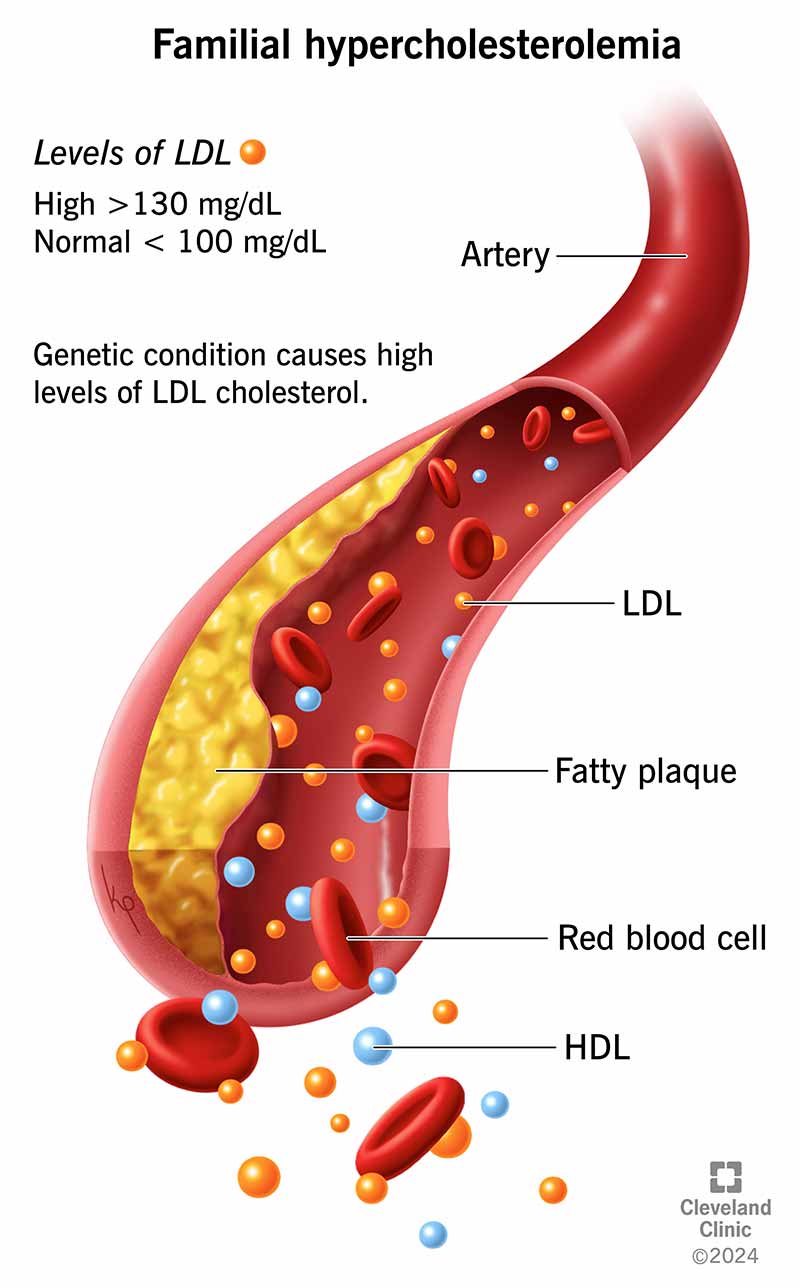
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22067-familial-hypercholesterolemia-illustration)
Familial hypercholesterolemia (FH) is a common genetic disorder that gives you very high levels of low-density lipoprotein (LDL) cholesterol. LDL is the “bad” cholesterol that can lead to cholesterol plaque buildup in your arteries. Over time, this can cause heart attacks, strokes or peripheral artery disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A healthy LDL level is less than 100 mg/dL (milligrams per deciliter). If you have familial hypercholesterolemia, your LDL may be 160 mg/dL or higher. Without treatment for this disorder, you’re at a higher risk of getting coronary artery disease before age 30. This can lead to heart and blood vessel problems at a much younger age than for people who don’t have FH.
Most people who have FH don’t know they have it. But once you know you have FH, you should start treatment right away. Medicines (as well as healthy foods and physical activity) can lower your LDL level.
There are two familial hypercholesterolemia types. The difference between them is whether one or both biological parents give you the genetic variant (change) that causes FH:
FH is a genetic disorder you inherit, or get, from one or both of your biological parents. In most people with this genetic issue, a specific protein (LDL receptor) that filters LDL out of your blood doesn’t work well, or there isn’t enough of it.
Advertisement
Most people with familial hypercholesterolemia will have a variant on one of four specific genes (APOB, LDLR, PCSK9 or APOE). But researchers are still finding more. If you appear to have familial hypercholesterolemia, but test negative for it, you may have gotten it from a genetic variant that researchers haven’t identified yet.
You may be at risk of having FH if you have a biological parent with the variant. FH is an autosomal dominant genetic disorder, which means it only takes one parent to pass it on.
Early treatment greatly reduces your risk of complications.
It’s common for people who have FH to have atherosclerosis, or plaque (atheroma) collecting in their arteries. This can lead to:
A provider can use a lipid panel or a DNA test to make an FH diagnosis.
A lipid panel blood test measures your cholesterol levels, including your LDL cholesterol. Children with familial hypercholesterolemia can have LDL levels higher than 160 mg/dL. Adults can have LDL of 190 mg/dL or higher. In people with the severe form, homozygous familial hypercholesterolemia, LDL can be higher than 400 mg/dL.
A DNA test can find problems with one of the genes researchers know can cause FH. If you have familial hypercholesterolemia, your biological siblings, parents and children should get a test. You can start screening a child at age 2 if they have a high risk of FH.
Your healthcare provider can make an FH diagnosis based on:
Familial hypercholesterolemia treatment may include one or more medications to reduce your LDL level as low as possible. People with severe FH may need periodic blood filtering (LDL apheresis) or — rarely — a liver transplant.
Medicines to treat FH
| Heterozygous FH | Homozygous FH |
|---|---|
| Statins | Statins |
| PCSK9 inhibitors | PCSK9 inhibitors |
| Bile acid sequestrants | Ezetimibe |
| Ezetimibe | Fibrates |
| Fibrates | Mipomersen |
| Nicotinic acid | Lomitapide |
| Bempedoic acid | Evinacumab |
| Heterozygous FH | |
| Statins | |
| Homozygous FH | |
| Statins | |
| PCSK9 inhibitors | |
| Homozygous FH | |
| PCSK9 inhibitors | |
| Bile acid sequestrants | |
| Homozygous FH | |
| Ezetimibe | |
| Ezetimibe | |
| Homozygous FH | |
| Fibrates | |
| Fibrates | |
| Homozygous FH | |
| Mipomersen | |
| Nicotinic acid | |
| Homozygous FH | |
| Lomitapide | |
| Bempedoic acid | |
| Homozygous FH | |
| Evinacumab |
After you get an FH diagnosis, you can expect to see your provider regularly to check on your heart and blood vessel health. Regular visits with your healthcare provider are crucial to make sure your medication is working. Contact your provider if you’re having trouble with side effects from your medicine. They may be able to switch you to a different one.
Get help right away, call 911 or emergency services if you have chest pain, shortness of breath or another symptom of a heart attack or stroke.
Advertisement
With familial hypercholesterolemia, you have a much higher risk of atherosclerosis, which can cause heart attacks and stroke. Without treatment for FH, you have a much higher risk of coronary artery disease compared to someone without FH. The chances of getting coronary artery disease go up even more if you use tobacco products or have diabetes or other risk factors for cardiovascular disease.
Without early treatment, heart disease can start before age 10 for people who have homozygous FH. People with the heterozygous type may develop heart disease at age 30 without treatment. For either type, this can lead to a heart attack by age 50 or 60 (depending on your sex).
As FH is a condition you inherit from your parents, it’s a part of your DNA all your life. You’ll need lifelong treatment.
Healthcare providers don’t have a cure for familial hypercholesterolemia. But once you know you have FH, your provider can treat you for it and help you prevent cardiovascular disease. With early treatment for FH, the outlook (prognosis) is excellent.
You can most likely have a normal life expectancy if you know your risk at a younger age and get treatment. Getting treatment for familial hypercholesterolemia cuts down your risk of heart disease by more than half. Without treatment, people with the rare type of FH may not live to be 30.
Advertisement
You may feel scared or discouraged when you find out you have familial hypercholesterolemia (FH). But getting a diagnosis is the first step toward lowering your risk of heart attack and stroke. Going to regular appointments with your healthcare provider will help them keep tabs on how you’re doing with the medicines they prescribe for you. Eating foods low in saturated and trans fats can help, as well as being physically active and addressing other risk factors for heart disease.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Do certain health conditions seem to run in your family? Are you ready to find out if you’re at risk? Cleveland Clinic’s genetics team can help.
