Hypercholesterolemia is a disorder known for an excess of low-density lipoprotein (LDL) in your blood. Many people can treat it by making changes to their diet and adding exercise to their lifestyles. Others need to take medicine to bring their LDL level down to a normal level. These treatments lower your risk of heart attacks and strokes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
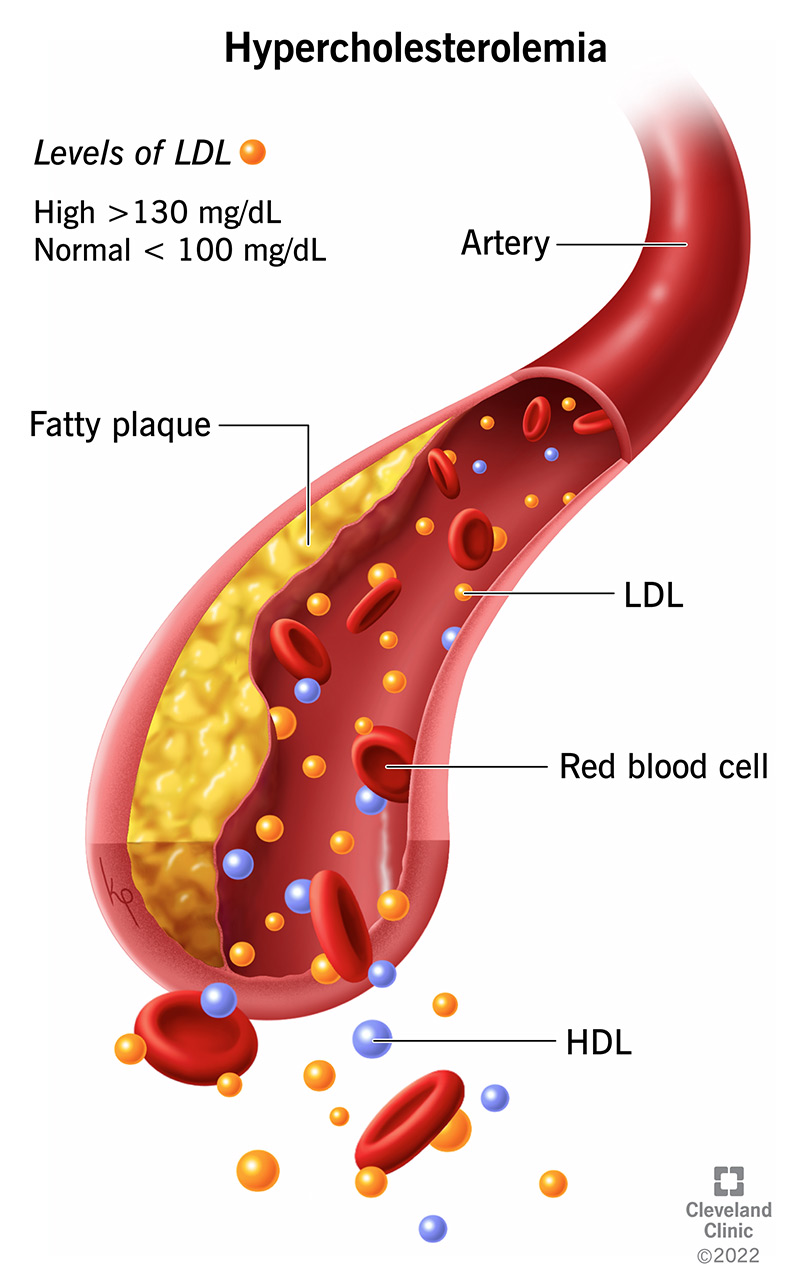
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/23921-hypercholesterolemia)
Hypercholesterolemia is a lipid disorder in which your low-density lipoprotein (LDL), or bad cholesterol, is too high. This makes fat collect in your arteries (atherosclerosis), which puts you at a higher risk of heart attack and stroke. Atherosclerosis is the main cause of cardiovascular disease, which is the reason for more deaths than anything else in the world.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
What your provider considers hypercholesterolemia depends on your other risk factors for cardiovascular disease.
Providers classify all of these as high levels of low-density lipoprotein cholesterol:
Depending on your risk of a cardiovascular event, your target LDL-C level can range from 116 mg/dL to less than 70 mg/dL.
Risk factors include:
No. Hypercholesterolemia is a type of hyperlipidemia that focuses on high LDL-C. Hyperlipidemia includes various disorders that feature high levels of fat in your blood — not just LDL.
You’re more likely to have a high level of LDL-C if you’re:
Hypercholesterolemia is very common. About 1 out of every 20 people has hypercholesterolemia. Nearly 1/3 of American adults have high LDL-C.
Hypercholesterolemia can lead to cardiovascular issues, such as:
There are no symptoms of hypercholesterolemia in most people. However, if you have severe hypercholesterolemia, you may have cholesterol deposits on your eyelid skin (xanthelasma) or connective tissue (xanthoma). Also, you may have cholesterol in your eye. This is called a corneal arcus.
Advertisement
Hypercholesterolemia causes include:
Usually at your annual physical exam, your healthcare provider will:
Once your provider rules out other causes of your hypercholesterolemia, they can do genetic testing. If you have pure hypercholesterolemia (familial hypercholesterolemia), your provider may suggest genetic testing for your family.
Hypercholesterolemia treatment involves bringing down your LDL level to prevent heart disease.
You can do this in several ways:
To lower the amount of LDL in your blood, you can:
Hypercholesterolemia medications include:
Providers prescribe other medicines for people with familial hypercholesterolemia.
Every medicine has side effects, but the benefits of cholesterol-lowering drugs make them worth taking.
Side effects may include:
Once you’ve taken medicine for 8 to 12 weeks, your provider will do another lipid panel test to see if your results improve. If your numbers don’t improve, they may increase your dose, switch you to a different cholesterol-lowering medicine or prescribe a second medicine for you.
You’ll need to manage your high LDL for the rest of your life. However, once you make healthy habits part of your routine, you won’t need to give them much thought.
You can start small, like having one meatless dinner a week or taking a daily walk after dinner. You can buy foods that are low in saturated or trans fats so you always have healthy food on hand. Also, you can add variety to your plant-based diet by trying vegetables you’ve never eaten before.
Advertisement
If you don’t treat your hypercholesterolemia, you can develop atherosclerosis. This is an artery-blocking issue that can cause a heart attack or stroke.
If you start living a healthier lifestyle, you can bring down your LDL. Doing this also lowers your risk of heart attack and stroke. Many medical studies have found that people have a good outcome when they manage their hypercholesterolemia.
You can lower your risk with a healthy lifestyle that includes:
Since managing cholesterol is a lifelong effort, you’ll need to keep up your lifestyle changes and continue taking your medicine.
Remember to:
Keep going to regular checkups with your provider. They’ll want to know if:
Your provider can switch you to a different medication if you’re having a bad side effect. Also, they may want to check your cholesterol regularly to make sure it’s at a normal level.
Advertisement
You’re not alone if you have a high level of LDL, which many call the “bad” cholesterol. Many people are dealing with this common problem. Your provider can be your ally in helping you get your LDL to a normal level. They can recommend ways to do it. If lifestyle changes don’t work, you can join the millions of people who take medicine to lower their cholesterol.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When heart disease runs in your family or you’re at risk, it’s important to keep an eye on your heart. Cleveland Clinic’s preventive cardiology providers can help.
