Oral lichen planus is a chronic inflammatory condition that affects the tissue lining inside your mouth. Symptoms include skin changes that look like white patches or lacy threads on the inside of your cheeks. Or your gums may be bright red in some areas. Oral lichen planus isn’t dangerous, but you might need medicine to ease your symptoms.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
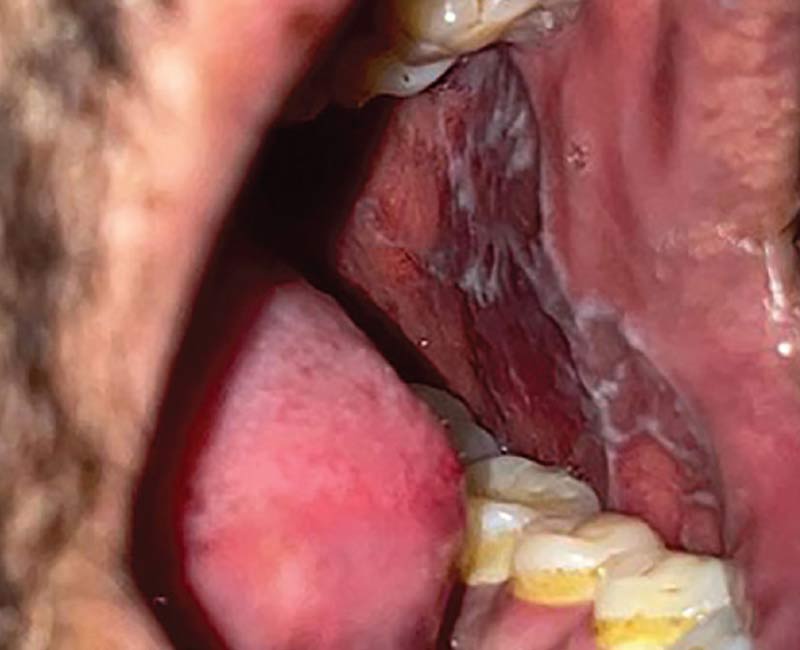
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/oral-lichen-planus)
Oral lichen planus (OLP) is a condition that causes inflammation inside your mouth. Normally, inflammation helps your body heal. But with OLP, it happens for unknown reasons and ends up damaging the thin tissue (mucosa) lining your cheeks, gums and tongue.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Oral lichen planus isn’t dangerous. It’s not contagious, so you can’t spread it to others. But it can cause abnormal tissue (lesions) to form in your mouth. It can make your mouth hurt.
This is why you should see a dental care provider if you notice signs of this disease. There’s no cure for oral lichen planus, but treatments can provide relief.
There are two main types of OLP:
Signs and symptoms depend on which type of OLP you have. Often, they occur as occasional flare-ups that go away on their own or with treatment. You may have:
People with oral lichen planus often have skin lichen planus. This form of the condition can cause an itchy rash on your genitals or scalp.
Advertisement
Doctors don’t know exactly why oral lichen planus occurs. But they do know that it’s related to your immune system. Typically, your immune system releases immune cells that attack harmful substances, like germs. In this way, your immune system keeps you from getting sick. But with OLP, the immune cells attack the tissue lining inside your mouth.
OLP shows up more often in people who take certain medicines, like:
It also sometimes occurs with diseases, like
But more research is needed to understand the connection between these conditions and OLP.
Many people with OLP learn to recognize triggers that spark symptom flare-ups. Common ones include:
Females are 3 to 4 times more likely than males to develop oral lichen planus. You can develop it at any age. But most people diagnosed are between 30 and 70 years old.
Oral lichen planus can lead to weight loss if eating hurts so much that you skip meals. Damage to the mucosa inside your mouth can also increase your risk of yeast and bacterial infections.
Research shows that about 1% to 4% of people develop oral cancer. The chance is greater if you have erosive oral lichen planus (the more severe form). But more studies are needed to understand why some people with OLP get cancer and others don’t.
Just to be safe, your healthcare provider will check your mouth for precancerous changes during check-ups. This is important because providers can often cure early-stage oral cancers.
A healthcare provider can diagnose oral lichen planus by examining your mouth. In many cases, providers take a tissue biopsy to confirm the diagnosis and rule out other diseases.
Treatment for OLP focuses on reducing symptoms and preventing flare-ups. This means you may not need treatment if you don’t have symptoms that are bothering you.
Treatment usually involves a mix of medications and lifestyle changes to avoid triggers.
If you have symptoms, your healthcare provider will likely recommend medications. Some may calm your immune system so there’s less inflammation. Others relieve pain. Common oral lichen planus treatments include:
Advertisement
Making small changes to your routine can help prevent flare-ups. Not everyone has the same triggers. But for many people, it helps to:
You should always talk to your healthcare provider before stopping medications. They can help you stop taking a medicine safely.
Most people notice major symptom relief within a month of using topical corticosteroids (the type you rub on the lesions). With a shot, it may take two to three treatments to feel better. With pills, it may take a few weeks.
Advertisement
Depending on the medication, your healthcare provider may gradually reduce your dosage so you take less of it over time. This reduces the chance of developing side effects from the medicine.
Once you’re diagnosed with oral lichen planus, you’ll need regular check-ups to keep tabs on your condition. This is the case even if you’re going through a period with no symptoms. For example, it’s important that your healthcare provider checks for precancerous changes. You may need more frequent dental cleanings to keep your mouth healthy.
If you’re experiencing a symptom flare-up, let your provider know. They can start you on treatments that can help you feel better.
Oral lichen planus never fully goes away. But this doesn’t mean you have to live with uncomfortable symptoms. Most people have periods of both symptom flares and remission. Remission means there aren’t any signs or symptoms of OLP.
And the experience of symptoms differs. Some people with OLP have painless lesions that don’t require treatment. Others need strong prescription medicines to feel relief.
Your healthcare provider can explain what you should expect based on your symptoms.
Speak to a therapist if the stress of managing your condition is taking a toll on your emotional health. Many people with long-term conditions benefit from therapy to help keep stressors at bay. This is especially important with OLP, as stress is a common trigger for symptom flare-ups. Don’t hesitate to ask for the care you need.
Advertisement
Oral lichen planus can be mistaken for a yeast infection in your mouth (thrush) and leukoplakia. Like OLP, both involve white patches or spots in your mouth. But their causes are different, and so are their treatments. A healthcare provider will do tests to find out which condition you have.
The first sign of oral lichen planus (OLP) may involve looking in a mirror and seeing odd lacy, thread-like lesions in your mouth. It may be burning in your gums when you take a bite of food. The experience is different for everyone. And so are the treatments that work best.
No matter your experience, know that oral lichen planus is a condition that you can manage with the help of a dental care provider. It may take some time to find the right combination of medications and lifestyle changes that help. But your provider will help find the treatment plan that works for you.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Dentistry plays an important role in oral health. Cleveland Clinic’s experts can design a personalized plan that will keep you smiling for the long haul.
