Mouth ulcers are small sores that form on your gums, lips, tongue, inner cheeks or roof of your mouth. Lots of different things can cause them, including minor injuries, hormonal changes and emotional stress. Many mouth ulcers go away on their own. Others may require treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
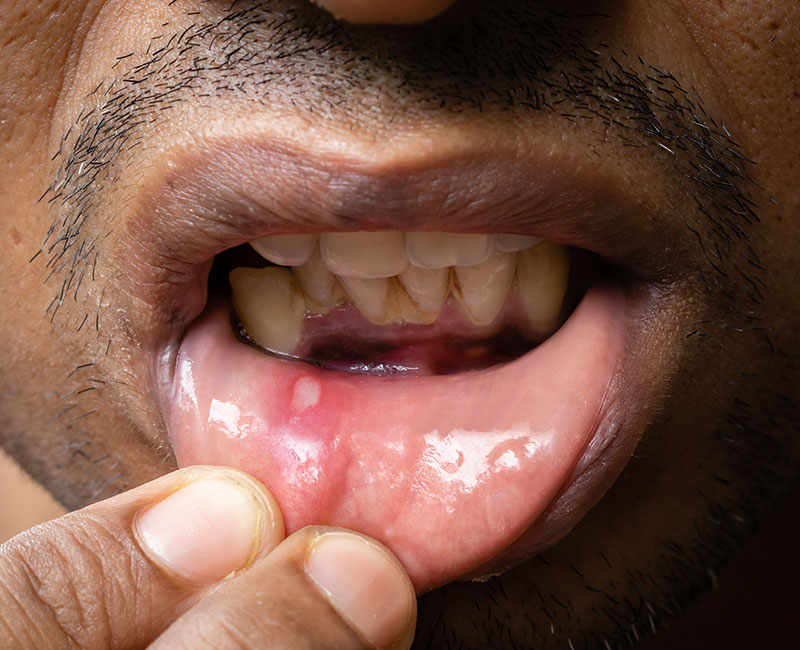
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/21766-mouth-ulcer)
A mouth ulcer is a sore that appears anywhere inside your mouth. These sores are usually red, yellow or white, and you might have one or several.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
You can get mouth ulcers on your:
These sores are often painful and can make eating, drinking and speaking uncomfortable.
Mouth ulcers can be alarming. However, they’re not a sexually transmitted infection (STI) and you can’t get or spread them from kissing or sharing food and drinks. Aside from any pain and discomfort, mouth ulcers are usually harmless and go away on their own in a week or two. But some types of mouth sores could point to underlying health conditions like viruses, autoimmune diseases or gastrointestinal issues.
There are many different types of mouth sores and lesions, including:
Advertisement
Mouth ulcers are usually easy to spot. They appear as sores on your gums, tongue, inner cheeks, inner lips or roof of your mouth.
Mouth sores are typically:
You may only develop one ulcer, or there might be more. Other symptoms could include:
Mouth ulcers may occur for a number of reasons, including:
Certain health conditions, including many autoimmune diseases, can also cause mouth ulcers. These conditions may include:
No. Unlike cold sores, mouth ulcers aren’t contagious, and they can’t spread through kissing or sharing food.
Cold sores (fever blisters) appear on the outside of your mouth, often on your lips. A virus causes them, and they’re very contagious. If you have a fever blister, you should avoid sharing personal items with other people to reduce the spreading of the virus.
A healthcare provider can diagnose a mouth ulcer with a visual examination. If you have a severe breakout, or if they suspect a specific health condition, they may order blood tests.
While most mouth sores heal on their own, your provider may prescribe medications to help ease discomfort. Common mouth ulcer treatments include:
There are also things you can do at home to relieve mouth sore symptoms:
In most cases, mouth ulcers go away on their own in about 10 to 14 days. If you have a mouth sore that lasts longer than three weeks, schedule an appointment with your healthcare provider. They can recommend treatment and tell you how to get rid of your mouth ulcer.
Advertisement
While you can’t prevent mouth ulcers altogether, there are things you can do to reduce your risk:
If your provider thinks you have an underlying condition that causes sores, treating your condition can reduce the risk of ulcers returning. Talk to your provider about ways to manage your health.
Anyone can get mouth ulcers. But you should call your healthcare provider if you have:
If you get severe or frequent mouth ulcers, here are some questions you might want to ask your healthcare provider:
Advertisement
“Mouth ulcer” is a broad term that describes any sore or ulceration inside your mouth. As we mentioned earlier, canker sores are the most common type of mouth ulcer. They affect about 20% of the general population. Many people use the terms “mouth ulcer” and “canker sore” interchangeably.
You might get a canker sore if you have a folate, vitamin B or iron deficiency. But in most cases, canker sores appear without a known cause and for no apparent reason. They can also recur (return), meaning they come and go over the course of your lifetime.
Some people confuse canker sores with cold sores (fever blisters), but they’re very different. A canker sore appears inside your mouth. A cold sore forms outside your mouth, usually on your lips. Canker sores aren’t contagious, but cold sores are.
Anytime you have a mouth sore that lasts longer than three weeks, schedule a visit with your provider. Mouth ulcers that don’t go away could point to other underlying health conditions.
Usually not, but it’s possible. A mouth ulcer that doesn’t go away could be a sign of oral cancer. In most cases of mouth cancer, mouth ulcers appear on or under the tongue.
Most mouth ulcers are harmless. But if you have a mouth sore that won’t heal, you should talk to a healthcare provider.
Advertisement
Most mouth ulcers aren’t dangerous. But they can be a huge inconvenience. Mouth sores cause pain that can keep you from enjoying the things you love, like eating certain foods, drinking comfortably, playing an instrument or kissing your partner. Your mouth ulcer will probably go away within two weeks. In the meantime, you can try over-the-counter medications and home remedies to reduce pain until the sore heals. If you have a mouth ulcer that doesn’t heal after three weeks, schedule a visit with a healthcare provider. You might have an underlying condition that needs treatment.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s primary care providers offer lifelong medical care. From sinus infections and high blood pressure to preventive screening, we’re here for you.
