Pelvic inflammatory disease (PID) is an infection that occurs in your uterus, fallopian tubes or ovaries. Sexually transmitted infections typically cause it. Symptoms include stomach, lower abdominal pain and vaginal discharge. Prompt PID treatment, usually antibiotics, helps avoid complications such as infertility. Your partner should get tested and treated, too.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
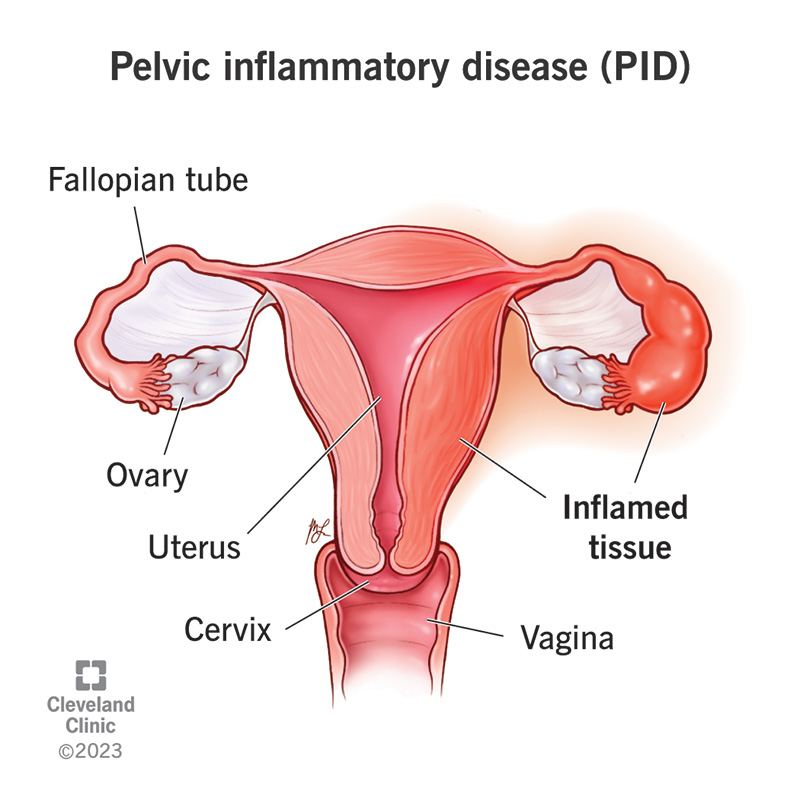
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/9129-pelvic-inflammatory-disease-pid)
Pelvic inflammatory disease (PID) is a serious infection in your uterus, fallopian tubes and/or ovaries. It affects females. PID develops when certain types of bacteria spread from your vagina to your reproductive organs. Bacteria from untreated sexually transmitted infections (STIs) are the most common cause of PID. However, bacteria normally found in your vagina can also cause PID.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When you have PID, you may feel pain in your lower abdomen (belly) or pelvis. You may also have unusual discharge (leaking) from your vagina. Severe PID can cause permanent damage your reproductive organs and prevent you from getting pregnant. Getting tested and treated for STIs is the best way to prevent PID.
Most people get PID through unprotected sex. Sex lets bacteria enter your reproductive system, where they can infect your organs.
Each year, more than 1 million females in the U.S. get PID. And more than 100,000 people become infertile because of it. PID occurs most frequently in females between 15 and 25 years old.
You may not realize you have PID. Symptoms might be mild or unnoticeable. But symptoms of PID can also start suddenly. They can include:
Pelvic inflammatory disease pain is mainly felt in your lower abdomen or pelvic region. It may feel tender and sore or like a dull ache. You may also feel pain deep in your pelvis during sex.
Advertisement
Bacteria entering your reproductive tract causes pelvic inflammatory disease. These bacteria are passed from your vagina, through your cervix and up into your uterus, fallopian tubes and ovaries. Normally, when bacteria enter your vagina, your cervix keeps them from spreading deeper to other reproductive organs. However, any type of infection can disrupt your cervix, preventing it from doing its job.
Many types of bacteria can cause PID, but the two most common infections that cause PID are gonorrhea and chlamydia. You get both of these infections through unprotected sex. These two STIs cause about 90% of all PID cases.
Less commonly, PID happens when normal bacteria gets into your reproductive organs. This can happen after:
It can take anywhere from a few days to a few weeks to develop PID if untreated gonorrhea or chlamydia is the cause. If you get PID from something else, it may take several months to develop it.
Most studies report only an association between douching and PID. What can be said is that douching can lead to bacterial vaginosis infections, but there’s only a potential association between douching and PID. Most healthcare providers advise against douching.
Yes, PID spreads most often during direct sexual contact.
You’re at higher risk for pelvic inflammatory disease if you:
The longer you have PID, the more serious its effects can become. The infection can cause scar tissue to form inside your fallopian tubes. The scarring can lead to several problems, including:
Advertisement
If you feel symptoms of PID, see your healthcare provider right away. The sooner you get care, the greater your chances of successful treatment. There isn’t one specific test for PID. Usually, your healthcare provider can diagnose PID through:
Your provider may also order:
In some cases, your provider may recommend:
Your provider will prescribe antibiotics that you take by mouth, typically for 14 days. Make sure to take all your medicine, even if you start feeling better. Often, your symptoms improve before the infection goes away. Your provider may recommend you return a few days after starting the medicine. They can check that treatment is working.
Advertisement
Some people take antibiotics and still have symptoms. If that happens, you may need to go to the hospital to receive antibiotics through an IV. You may also need IV medication if you:
You shouldn’t have sex until you finish treatment. When you do have sex again, use condoms every time to prevent infections.
Surgery is rare for PID but can help in some cases. If you still have symptoms or an abscess after taking antibiotics, talk to your healthcare provider about surgery.
If you have pelvic inflammatory disease, tell your sexual partner(s). They should receive treatment. Otherwise, you may get PID again when you resume sex.
If you get prompt diagnosis and treatment for an infection, antibiotics can cure PID. But treatment can’t reverse any damage that already happened to your reproductive organs. Don’t wait to get treated. See your provider right away so you can get the help you need.
PID can affect fertility. Of the people who had PID, studies found that 1 in 8 had difficulty getting pregnant. Up to 1 in 10 people ultimately received a diagnosis of infertility. People who had repeat infections had a harder time getting pregnant.
Advertisement
Bacteria from PID can cause scarring on your fallopian tubes. This scar tissue makes it harder for an egg to get from your ovary to your fallopian tube, then down to your uterus. If an egg can’t get through your fallopian tube, sperm can’t fertilize it.
Yes, you can get PID again. Getting PID once doesn’t protect you from getting it again.
You and your partner should wait a week after finishing your antibiotics before resuming sex. Doing so will help prevent re-infection.
Yes, women who have sex with women (WSW) can get PID. This is because bacteria that cause PID can live on a vagina, penis or any object you place in your vagina.
Sometimes, PID isn’t due to a sexually transmitted infection. It can come from normal vaginal bacteria traveling to your reproductive organs. Avoiding douching may lower the risk.
Most of the time, though, PID happens because of unprotected sex. Take steps to practice safe sex. Ways to protect yourself from sexually transmitted infections (STIs) that can cause PID include:
If you’re sexually active, talk to your healthcare provider about yearly testing for sexually transmitted infections. Providers often recommend testing for chlamydia and gonorrhea to help keep you safe. Also, before having sex with a new partner, it’s a good idea for both of you to get tested for STIs.
If you feel symptoms of PID, see your healthcare provider right away. If you have PID, the most important thing you can do is get treatment.
Other tips for taking care of yourself include:
See your provider if you experience any symptoms of PID. Seek immediate medical care if you have:
If you have PID, ask your provider:
Yes, it’s possible to get PID when the bacteria that normally exist in your vagina travel up into your reproductive organs. This is usually not the cause, though.
Yes, PID can be serious. Early diagnosis and treatment are essential to reducing your risk of long-term complications like infertility.
Pelvic inflammatory disease (PID) is an infection of your reproductive organs. A sexually transmitted infection, such as gonorrhea or chlamydia, typically causes it. If you notice symptoms of PID, such as pain in your lower abdomen, talk to your healthcare provider. The provider can diagnose PID and give you antibiotics to treat it. Early treatment is key to avoiding complications of PID such as infertility. Your partner(s) should get treated, as well. You can prevent PID by using a condom every time you have sex.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From routine pelvic exams to high-risk pregnancies, Cleveland Clinic’s Ob/Gyns are here for you at any point in life.
