Pancreatic cancer starts in your pancreas, a gland in your abdomen that aids in digestion. Diagnosis is often delayed because symptoms aren’t usually noticeable until the cancer is already advanced. Treatments include surgery, chemotherapy and radiation therapy. Pancreatic cancer is hard to treat, and the survival rates are low.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
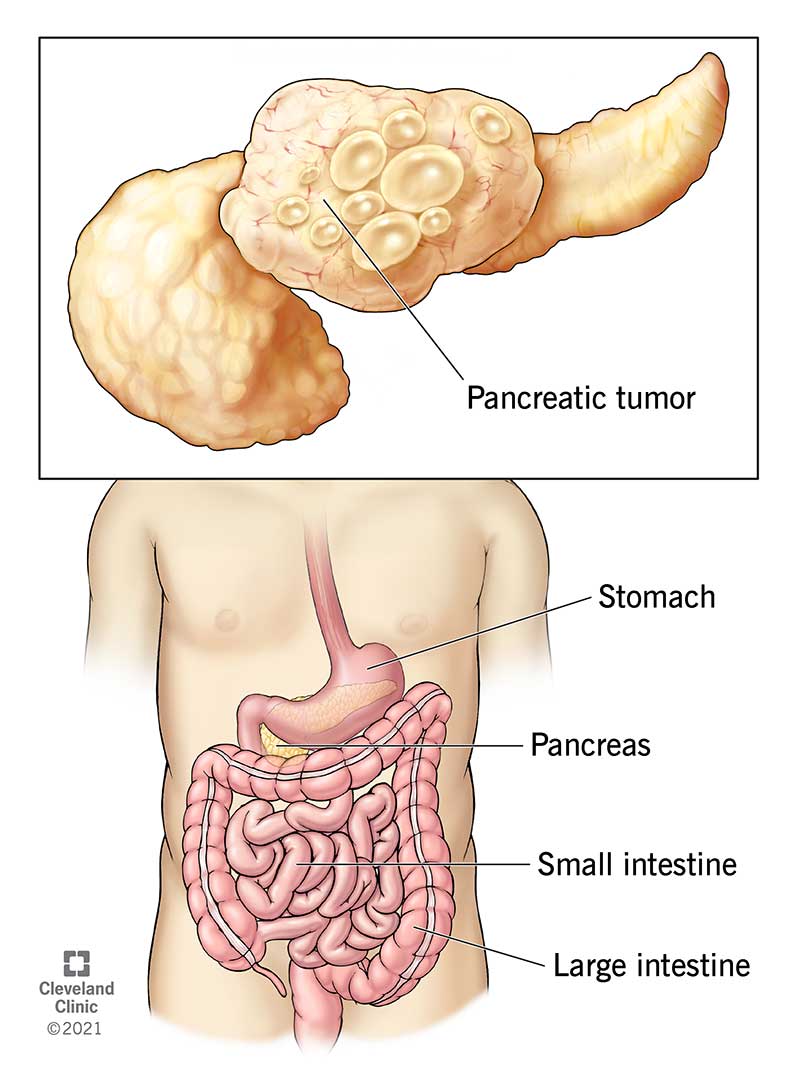
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/21786-pancreatic-cancer-illustration)
Pancreatic cancer is an aggressive tumor that forms in your pancreas, a gland that aids in digestion. This disease is the 11th most common cancer in the U.S. It’s on track to be the second most common cause of cancer-related deaths by the year 2030.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It often doesn’t cause symptoms in the early stages, so many people don’t learn they have it until it’s already spread. It’s also resistant to many common cancer drugs, making it notoriously difficult to treat. Even when it’s caught early, more than half of people will not survive beyond five years because it’s so aggressive and difficult to treat.
Still, no two diagnoses are the same. Your healthcare provider will let you know what to expect based on your situation.
There are two main types:
The differences are important because treatments and outlook vary by type. PNETs are usually less aggressive than adenocarcinoma.
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_hk0ofhgx/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Warning signs of pancreatic cancer and how to spot them.
Unfortunately, there aren’t any early signs of pancreatic cancer. Symptoms often start once the tumor impacts other organs in your digestive system. At this point, the disease is often advanced.
Symptoms include:
Advertisement
Your healthcare provider might suspect pancreatic cancer if you’ve recently developed pancreatitis — inflammation in your pancreas — or diabetes. This is because your pancreas helps manage your blood sugar levels.
It happens when gene changes (mutations) cause cells to grow out of control. Over time, they can form a tumor. Experts don’t know why it happens. But they’ve found mutations common in pancreatic cancer. For instance, more than 9 out of 10 cases involve errors in the KRAS gene.
About 1 out of 10 people with this condition inherit genes from a biological parent that raise their risk. But most people develop mutations linked to cancer that are not hereditary in their lifetimes.
Most people diagnosed are over 60 years old. The risk is greater among males and people who are Black or of Ashkenazi Jewish descent.
Other risk factors include:
You can’t change most of these things. But you can reduce your risk by choosing not to smoke (or quitting if you do) and losing weight if you have obesity.
It’s difficult to detect pancreatic cancer early. Diagnosis is often delayed because symptoms don’t start until the cancer is advanced. Also, healthcare providers can’t feel lumps in your pancreas during routine exams. It’s too deep inside your abdomen.
Instead, you’ll need several tests, including:
Healthcare providers mainly use imaging scans, like CT, MRI or PET scans, to determine the stage of pancreatic cancer.
Advertisement
They’ll label the tumor as:
Sometimes, providers use laparoscopy to see how much the cancer has spread. They’ll make a few small cuts in your abdomen and insert a scope with a camera on the end. This allows them to see inside your abdomen and look for signs of cancer.
Your provider may also rank the cancer from stages 1 to 4. Stage 1 means early-stage disease, while stage 4 is metastatic.
They’ll explain how the cancer stage impacts your treatment options.
Pancreatic cancer is one of the hardest cancers to treat. In addition to often being advanced at diagnosis, your pancreas is hard to access. First, it’s behind your stomach and close to key blood vessels. This makes surgery challenging. It’s enclosed by dense tissue called the stroma. Drugs trying to reach the tumor can’t always cross this tissue barrier.
Advertisement
This is why one of the best options may be to take part in a clinical trial to access new treatments that are trying to overcome these challenges.
Surgery on your pancreas is the only way to cure pancreatic cancer. But surgeons only recommend it when they think they can remove all of the cancer. Otherwise, there’s little to no benefit.
For surgery to be successful, the cancer must be in only your pancreas. There are different techniques, depending on the location and size of the tumor:
You can live without a pancreas, but it can cause major side effects. Your pancreas makes insulin and other hormones that keep blood sugar at a safe level. Without a pancreas, you’ll develop diabetes and need insulin shots to survive. You’ll also need to take pancreatic enzyme pills to help with digestion.
Advertisement
Chemotherapy uses drugs to kill cancer cells throughout your body. Healthcare providers give these drugs in pill form or through an IV in your arm. It’s the most common treatment for people diagnosed with pancreatic cancer.
Providers may use chemotherapy alone, especially if the cancer is advanced. They may recommend chemotherapy before surgery to shrink the tumor or after surgery to kill any remaining cancer cells.
Radiation therapy uses high-energy X-rays to kill cancer cells. Most often, providers combine radiation therapy with chemotherapy. They may recommend it before surgery, after surgery or as part of your main cancer treatment.
This treatment uses drugs that “target” certain proteins. These proteins help cancer cells grow and spread. You may benefit from a targeted therapy if the cancer cells contain the gene changes that the drug targets.
Providers may combine targeted therapy with other treatments. Researchers are testing promising new forms of this treatment in clinical trials.
It may be a good idea to speak with a genetic counselor if you’re concerned about inherited gene mutations linked to pancreatic cancer. There aren’t standard screening guidelines for this disease. But we know that in some cases, there’s a biological family link.
If your diagnosis involves an inherited mutation, a genetic counselor can help you understand how to communicate potential risks to family members.
If you have a family history of pancreatic cancer, a genetic counselor can help you decide whether you'd benefit from hereditary gene testing.
A pancreatic cancer diagnosis can feel overwhelming. Most people learn they have it once they’re already at stage 4, where it’s most challenging to treat.
Still, no two cases are the same. Your care team will help you decide the best treatment plan for your situation. This may involve treatments to send cancer into remission for early-stage pancreatic cancer. It may involve managing symptoms and helping you feel better. This is called palliative care.
Unlike hospice treatments, palliative care isn’t end-of-life care. It can help no matter your prognosis. It can:
Most people who are diagnosed with pancreatic cancer die within the year. The five-year survival rate is 13%. This means that about 13 out of 100 people with this diagnosis survive beyond five years.
Remember, though, that survival rates are estimates. They can’t tell you how long you will live or how you’ll respond to treatment. Also, the numbers are about the past. They don’t account for the impact new treatments can have on your outlook.
This is why your healthcare provider is your best resource to explain your prognosis.
Yes. Cancer survivors include people with pancreatic cancer. The best chance for survival involves having a successful surgery for early-stage cancer. The National Comprehensive Cancer Network recommends treatment in a center that does at least 15 to 20 pancreatic cancer surgeries each year.
A pancreatic cancer diagnosis is life-changing. No matter your prognosis, your next steps will likely involve major challenges. You might consider joining a support group for people with this disease. Spending time with others who are going through the same things can be beneficial. You can also talk with a counselor, therapist or social worker about how you’re feeling. And there are resources available for both you and your family.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
A pancreatic cancer diagnosis can make your world tilt. Cleveland Clinic experts are here to start personalized treatment for the best possible outcome.
