Ascites is a buildup of fluid in your abdomen causing a swollen belly. It most often occurs because of cirrhosis, a liver disease. Talk to your healthcare provider if you have cirrhosis and notice you’re gaining weight very quickly. Your provider will talk to you about treatments, which could include a low-sodium diet, medication, surgery or a liver transplant.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
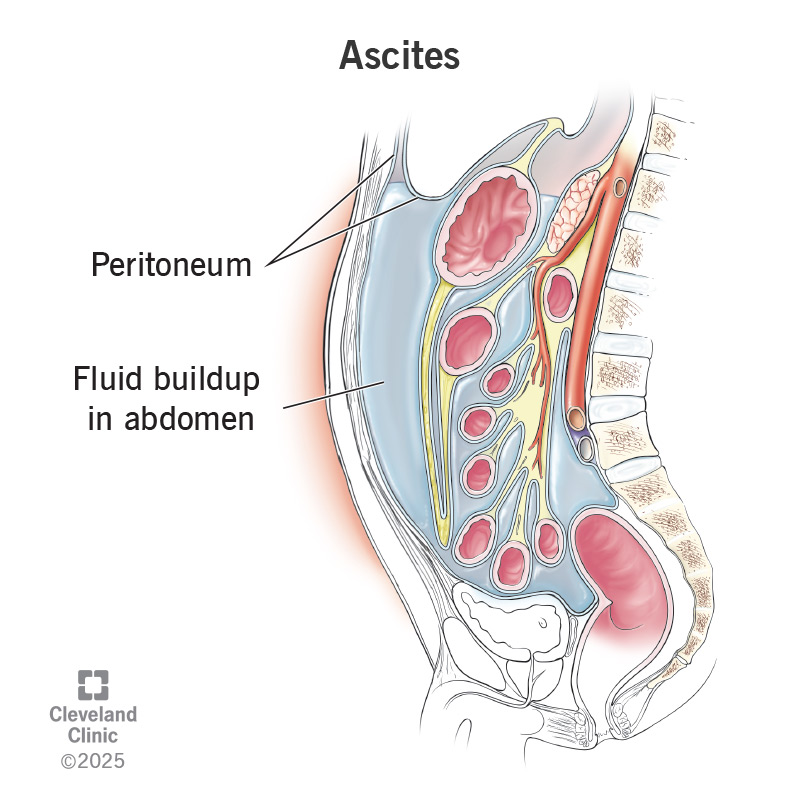
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/14792-ascites.jpg)
Ascites (ay-SITE-eez) is when too much fluid builds up in your abdomen (belly). This condition most often happens in people who have cirrhosis (scarring) of the liver. It can make movement difficult and be very uncomfortable.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A sheet of tissue called the peritoneum covers your abdominal organs, including your stomach, intestines, liver and kidneys. The peritoneum has two layers. Ascites happens when fluid builds up between the two layers. The fluid can make it look like you have a watermelon or basketball in your belly.
The main symptoms of ascites are a large belly and rapid weight gain (two or three pounds per day for three days). You may also have swelling in your ankles (edema).
Other symptoms include:
Cirrhosis is the most common cause of ascites, but it’s not the only cause. Other conditions that can cause it include:
An even less common cause is nephrotic syndrome.
Cirrhosis damages your liver and affects how blood flows through it. This damage can increase pressure in your portal vein, which carries blood to your liver. When this happens, it’s called portal hypertension. This sends an incorrect signal to your kidneys to hold onto sodium and water. When this goes on long enough, salt and water spill out into your abdominal cavity.
Advertisement
Having a condition that causes cirrhosis puts you at the greatest risk of developing ascites. These conditions include:
Ascites can lead to:
Your healthcare provider performs a physical exam and checks your belly for signs of fluid buildup. They’ll ask you about your symptoms and medical history. They may also order blood tests to check your liver and kidney function.
After the exam, your provider will recommend other tests to confirm a diagnosis:
Your healthcare provider will check to make sure the ascites aren’t due to heart or kidney problems or cancer.
Treatment for ascites involves reducing fluid buildup in your belly. Healthcare providers typically try these treatment methods first:
Advertisement
Sometimes, diuretics and lowering sodium intake aren’t enough to improve ascites. You may need other treatments, including:
The treatment your provider recommends is based on factors like the severity of ascites, your medical history and the overall health of your liver.
Contact your provider if you have cirrhosis of the liver and notice the following symptoms:
Go to the emergency room right away if you have:
If you have ascites, ask your healthcare provider:
Advertisement
Ascites is a sign that your liver isn’t working as it should. It can impact your quality of life and cause uncomfortable symptoms. Medications, low-sodium foods and procedures like paracentesis can help improve your symptoms and reduce your risk of complications. Your healthcare team will monitor you to make sure treatment is working.
If you have ascites, these steps can help you manage the condition:
The best way to prevent ascites is to take care of your liver. Some things you can do are:
Ascites is a sign of liver damage that can lead to uncomfortable symptoms. It may make you feel self-conscious about your appearance or worry about the health of your liver. There are treatment options available to you that help you manage ascites so you can feel your best. Restricting your salt intake is one of the most effective treatments. Ask your provider about working with a dietitian to plan meals that are low in sodium. Regular check-ins with your provider are important so they can make sure treatment is helping to manage ascites.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cirrhosis is a serious condition that causes liver damage. At Cleveland Clinic, our experts will help you manage cirrhosis and relieve symptoms.
