Osteosarcoma is cancer that begins in your bones, usually in the arms or legs. Limited movement, bone pain, a lump and an unexplained broken bone are the most common symptoms. Many treatments are available. Around 7 in 10 people survive if the osteosarcoma doesn’t spread to other parts of their bodies.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
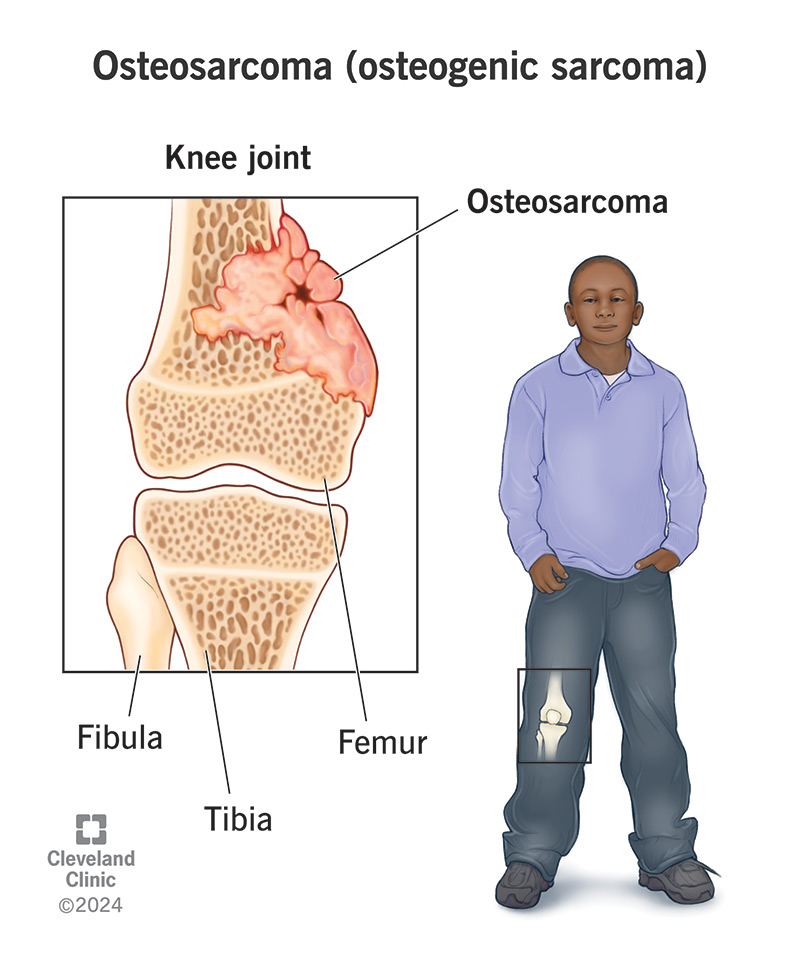
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/osteosarcoma-osteogenic-sarcoma)
Osteosarcoma is a type of bone cancer. In the beginning, the cancer cells appear to be regular bone cells. Then, they create malignant (cancerous) tumors, and those tumors create irregular, diseased bone.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Healthcare providers sometimes call it osteogenic sarcoma. A “sarcoma” is a type of cancer that develops in connective tissue such as bone, cartilage or muscle. “Osteo-” refers to bones. “Osteogenic” means it makes bone cells.
Osteosarcoma most commonly affects kids and teens. Experts estimate that fewer than 1,000 people in the U.S. develop osteosarcoma each year.
Osteosarcoma most often affects long bones, like the ones in your arms and legs. It usually develops near the ends of your bones around joints, especially near knees, hips or shoulders.
The bones most often affected include the:
Other less common locations for osteosarcoma include the:
Providers categorize osteogenic sarcomas by three grades depending on how quickly they’ll spread (metastasize):
Low-grade tumors grow slowly and usually remain where they form. A high-grade tumor will grow quickly, and is more likely to spread.
The most common symptoms of osteosarcoma include:
Advertisement
Osteosarcomas can cause intense pain. But some are painless. It depends on where they develop and how fast they grow.
For example, it may be painful to lift things if the tumor is in your arm bones. Or you might limp if it’s in your leg bones.
Experts aren’t certain what causes osteogenic sarcoma. Some causes may include:
Teens are the most likely group to develop osteosarcoma. In fact, more than 3 out of every 4 people with osteosarcoma are younger than 25. The average age of diagnosis is 15.
You might have a higher risk if you’ve ever had treatment for another type of cancer. Radiation therapy and taking alkylating agents (certain types of cancer medication) can increase the chances that you develop osteosarcoma in the future.
Having certain health conditions can increase your risk, including:
A healthcare provider will begin with a thorough history and physical examination. They’ll ask about your symptoms and medical history. Tell your provider if you’ve had any prior radiation treatment or if anyone in your biological family has a genetic condition or history of cancer. Your provider will look for lumps that may be protruding from your bones. You’ll probably need to see an oncologist — a healthcare provider who specializes in diagnosing and treating cancer.
Your provider might also use some tests when making a diagnosis, including:
Advertisement
After your provider diagnoses osteosarcoma, the next step is to find out if the cancer cells have spread. This is called “staging.” The cancer can spread through your blood, your lymphatic system or tissues. You may need additional imaging tests like a whole-body bone scan or PET scan. These tests will help your provider see if the cancer has metastasized to other bones, organs or areas of your body.
The most common treatments are chemotherapy (chemo) and surgery to remove osteosarcoma tumors and cancer medications to kill cancer cells throughout your body. You’ll probably need chemo, then surgery, then more chemo.
Your providers might use radiation therapy to treat osteosarcoma, especially if the cancer spreads to areas where you can’t have surgery.
You’ll probably need surgery to remove the osteosarcoma. Your surgeon will try to preserve as much of your natural bone and tissue as they can. But they’ll remove some of the healthy tissue around the tumor to make sure they’re taking out as many cancer cells as possible.
Some surgeries you may need include:
If you have limb salvage surgery, your surgeon will replace the removed section of your bones with either an artificial implant (prosthesis) or a bone graft.
Advertisement
You may need a prosthetic limb after amputation or rotationplasty.
You may experience complications or side effects right away. Some can last for months or even years. They might include:
The survival rate depends on which type of osteosarcoma you have, and if it spreads from its original location.
Experts estimate that 7 in 10 people survive osteosarcoma if it hasn’t metastasized (spread). Survival rates for metastatic (spreading) osteosarcoma are around 5 in 10 people. Your provider will tell you what to expect.
Osteosarcoma can be aggressive. High-grade tumors can spread quickly. Lower-grade osteosarcomas will spread slowly (or not at all).
Cancers metastasize at different rates because everyone’s body and health are unique. Even though experts know that high-grade osteosarcomas can spread quickly, there isn’t a set amount of time that applies equally to everyone.
Two in every 10 cases of metastatic osteosarcoma cases have already spread by the time they’re diagnosed. Visit a healthcare provider as soon as you notice any symptoms or changes in your body that make you feel worried or concerned.
Advertisement
Because experts aren’t certain why it develops, there’s no way to prevent osteogenic sarcoma. Talk to your healthcare provider about genetic testing for cancer risk if you’re interested in screening yourself or your children. Your provider will tell you if genetic testing is a good idea for you or your family.
Maintaining or reclaiming a good quality of life is vital before, during and after treatment for osteogenic sarcoma. It’s not only about taking care of your physical health: your mental and emotional health are just as important. A mental health provider or therapist can help.
Your healthcare provider will tell you how often you’ll need follow-up visits. They’ll have to check for:
You’ll need more frequent at first (every three to six months). As you get further from treatment, you might only need one checkup a year. You’ll probably need routine physical exams and lab and imaging tests to monitor any changes in your body.
You might want to ask your provider:
Living with osteosarcoma isn’t easy. But there are lots of treatment options. Your providers will help you find the best ones.
Work closely with your healthcare providers and get support from your loved ones. Never be ashamed or afraid to ask for help. Your loved ones, providers and mental health professionals can all support you, no matter what you’re feeling on any given day.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When your child has bone cancer, you want them to have the best care. Cleveland Clinic Children's healthcare providers deliver expert osteosarcoma treatment.
