The tibia is the second-longest bone in your body. It plays an important role in how you stand, move and keep your balance. It’s also an anchor for other tissue, like muscles, tendons, ligaments and nerves. Tibias are strong. So, it usually takes a serious injury like a car accident to break them.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
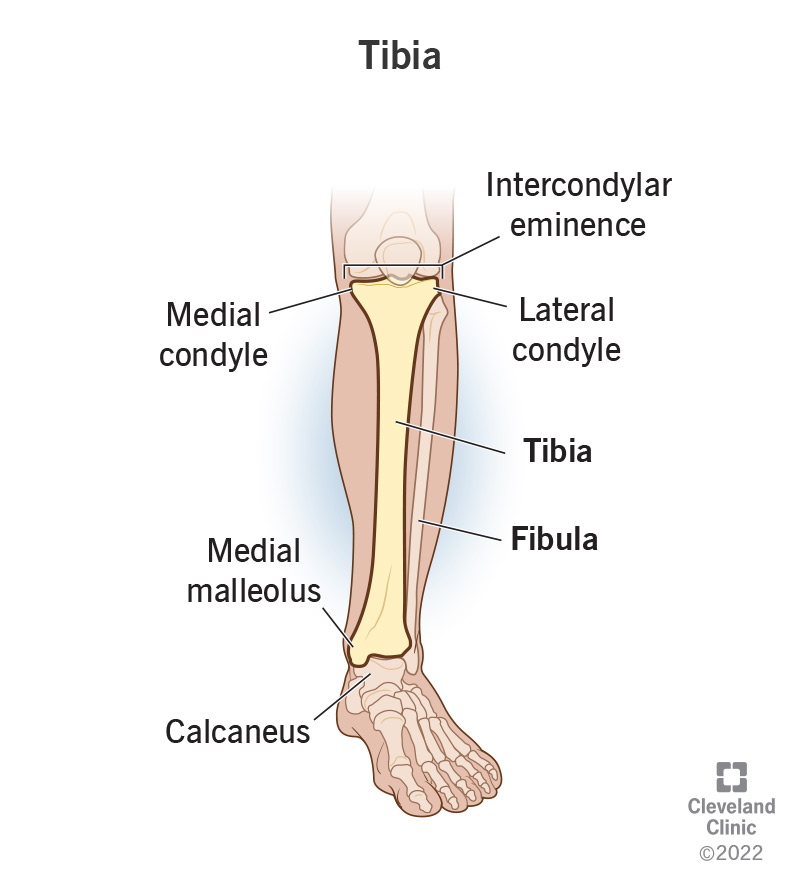
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/23026-tibia)
The tibia is your shin bone. It’s an important part of how you can stand and move.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s the second-longest bone in your body. Most adults’ tibias are around 15 inches (38 centimeters) long. Only your thigh bone (femur) is longer.
Your tibias are some of your strongest bones. So, they won’t need much maintenance. But listen to your body if you’re feeling pain or any other symptoms. Everyone has an occasional ache or pain. See a healthcare provider if you’re feeling bone pain from deep inside your shin or know you experienced an injury.
Your tibia has several important jobs, including:
You have one tibia in each shin. It’s the bigger bone in your lower leg that’s closer to the front. The calf bone (fibula) is the other.
The tibia runs from just under your knee to your ankle. It’s closer to the inside of your body than the fibula.
The tibia has a flat end that forms a shelf at the bottom of your knee, a long middle shaft and a notch at the bottom where it forms your ankle.
These three sections each have a medical name:
Advertisement
You’ll probably never need to know or remember these medical names and labels. They’re usually more for your healthcare provider to use as they describe where something is affecting your tibia. You might see some of these words on an X-ray result, for example.
Your tibias are strong, but injuries and some health conditions can damage them, including:
Visit a healthcare provider if you notice any new pain or other symptoms in your shin. Especially if they last more than a few days. Go to the emergency room if you think you might have a broken tibia. Don’t try to walk or put weight on that leg.
You might only think about your tibia when you bang your shin into the edge of a coffee table. Whether or not it’s top of mind, the tibia is a huge part of your ability to stand and move throughout your day.
Talk to your healthcare provider about keeping your bones healthy. They’ll help you understand your osteoporosis risk. Anything you do to improve your overall health will also help keep your bones strong.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
From sudden injuries to chronic conditions, Cleveland Clinic’s orthopaedic providers can guide you through testing, treatment and beyond.
