Purpura causes red, purple or brown blood spots on your skin. It happens when small blood vessels leak blood under your skin’s surface. There are different types of purpura. Treatment for purpura depends on the underlying condition causing it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
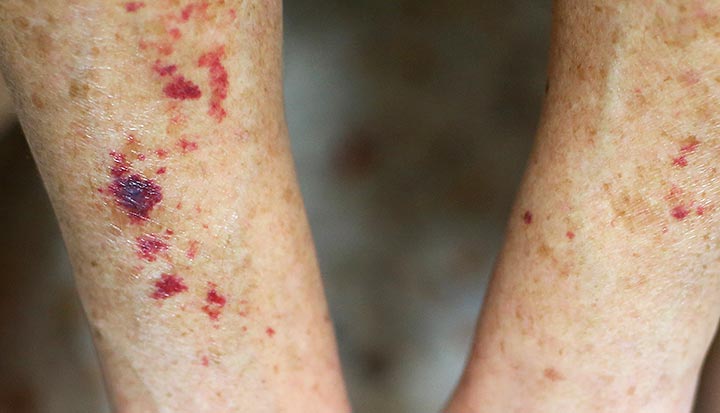
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/22695-purpura)
Purpura is purple spots or patches on your skin or in your mucus membranes (such as your mouth and throat). The spots appear differently depending on your skin tone. For example, they may appear brownish-black on darker complexions and reddish-purple on lighter complexions. Purpura may resemble a bruise or look like a spot of blood under your skin.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
They happen when small blood vessels leak blood under your skin’s surface. Purpura isn’t a medical condition but a sign of another condition causing the bleeding. Purpura can also be caused by drug interactions, vitamin deficiencies or congenital disorders.
There are many different types of purpura. They’re classified based on the underlying condition causing them. Your healthcare provider should treat bleeding or bruising under your skin (that isn’t from a known injury), as it may be a sign of a more serious condition.
Purpura is small, flat spots on your skin. They look red or purple on lighter skin tones but appear brown or black on darker skin tones. Purpura is commonly referred to as a blood spot under your skin. Purpura usually consists of smaller dots that cluster in a specific area but may appear as one larger patch. Applying pressure to the area doesn’t affect the color (blanching the skin).
Purpura can develop anywhere on your skin. It’s most common on your limbs (arms, hands, feet and legs) but can appear in your mouth or on any other mucus membrane.
The two main types of purpura are related to blood platelet levels. Platelets help your blood clot and prevent severe bleeding.
Advertisement
Other serious (but rare) types of purpura require emergency medical treatment. These include:
If you have senile purpura, you may have bruises or spots on the skin due to age or sun exposure. This type of purpura happens when our blood vessels become weak. It’s common in older adults.
Petechiae are tiny, dot-like purpura. Purpura is between 4 millimeters (mm) and 10 mm in diameter. If the purpura spot is less than 4 mm wide, it’s called petechiae. Purpura larger than 1 centimeter (cm) is called ecchymoses (or bruises).
Anyone can get purpura. It’s slightly more common in adults than in children. Children typically recover quickly and without treatment. In adults, purpura is usually a sign of an underlying condition but can also resolve without treatment.
The cause of purpura depends on the type.
Common causes of thrombocytopenic purpura are:
Common causes of nonthrombocytopenic purpura are:
Purpura isn’t a medical condition. Instead, it’s a sign of another condition. There’s usually nothing you can do to reduce your risk. Specific risk factors for purpura are:
Purpura itself doesn’t usually cause complications; however, the underlying condition or disease causing purpura can. If a blood clotting disorder is causing the purpura, it could cause severe or fatal bleeding. Talk to your healthcare provider about any suspicious blood spots or bruises so they can treat the cause and minimize your risk of complications.
Advertisement
Purpura isn’t a diagnosis. It’s a sign of something else. Once your healthcare provider determines the discolored skin spots are purpura, they must determine what’s causing it.
Your healthcare provider will begin with an examination of your skin. They’ll discuss your medical history and any drugs or medications you’re taking. They’ll take note of the size and color of the purpura and ask you when they first appeared.
Your healthcare provider may recommend tests such as a complete blood count (CBC) or a skin biopsy to determine the cause of the purpura.
Determining if the purpura is related to a blood clotting disorder or platelet issue is the first step in diagnosing the condition causing purpura. A blood test will reveal a low platelet level. If platelet levels are OK, a skin biopsy may be the next step.
Treating purpura involves identifying and stopping the underlying cause of the bleeding. Sometimes, treatment isn’t needed and the purpura goes away on its own. Once your healthcare provider determines the cause, they can:
Advertisement
Some common treatments for purpura are:
As with most treatments, there are potential side effects. Discuss these with your healthcare provider to make sure you know what to expect.
Contact your healthcare provider if you notice purpura or any blood spots, patches or skin discoloration. Purpura can be a sign of a severe disease or underlying condition. For example, if purpura is related to a blood clotting disorder or low platelet levels, it can put your life at risk. In other cases, purpura isn’t serious and resolves with minimal treatment. Unless you get checked out by your healthcare provider, there isn’t a way to be sure.
Most people don’t experience itching or painful purpura. However, some people may feel their skin is more sensitive or tender.
Advertisement
It can look like both. If you’re bleeding under your skin, it can appear as one larger patch (bruise) or several smaller dots (petechiae). It’s common for petechiae to resemble a rash because the dots are tiny and tend to cluster.
Purpura (or blood spots) on your skin can be a sign of a more serious condition. Contact your healthcare provider if you notice any discolored patches, spots or bruises on your skin. Treating purpura involves finding the cause and treating that condition or disease. Certain conditions may make you more prone to purpura such as low platelet counts or a blood clotting disorder. In most cases, purpura isn’t serious and goes away with treatment.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Every day, people see your skin, hair and nails. At Cleveland Clinic, our expert and caring dermatology team will make sure they’re healthy and strong.
