A bone marrow biopsy is a procedure that involves removing a sample of bone marrow and testing it for signs of disease. Your healthcare provider may perform a biopsy to diagnose blood disorders, cancer and many other conditions that may affect your bone marrow. The procedure lasts around 30 minutes and doesn’t usually involve a hospital stay.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
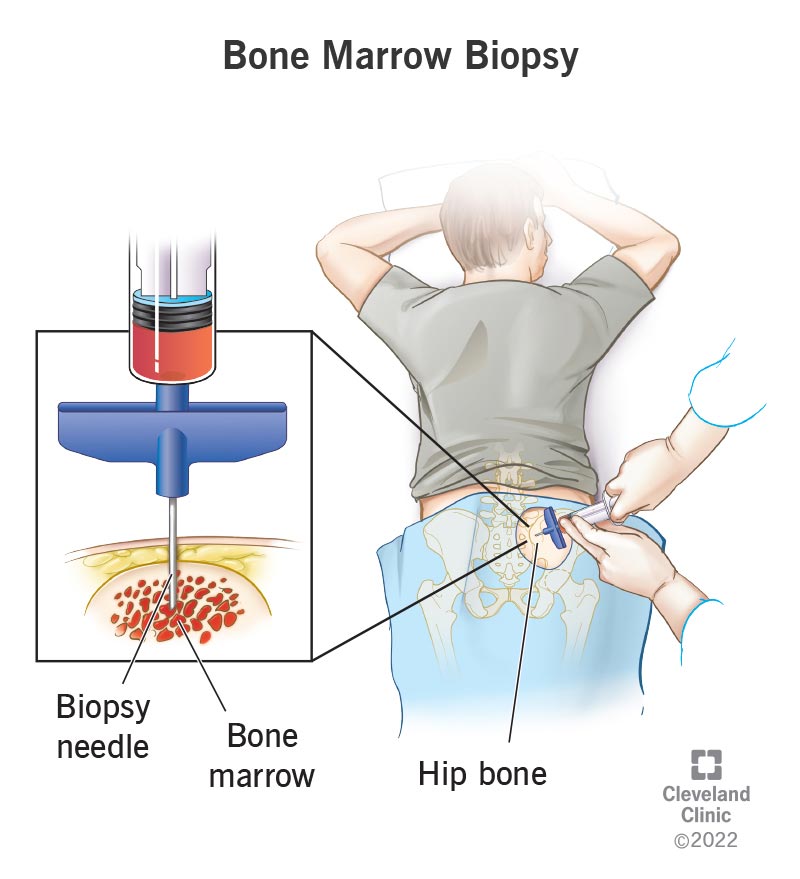
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/Images/org/health/articles/17735-bone-marrow-biopsy)
A bone marrow biopsy is a procedure used to diagnose conditions affecting your blood and bone marrow. Your bone marrow is where your body’s blood cells get made. During the procedure, your healthcare provider removes a small sample of marrow from inside a bone. Afterward, a specialist called a pathologist examines the cells from the marrow under a microscope, looking for signs of disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Many conditions — including blood disorders and some cancers — require a bone marrow biopsy to confirm a suspected diagnosis.
Bone marrow is located inside the hollow center of your larger bones. Bone marrow consists of soft, sponge-like tissue and a liquid.
The tissue part of bone marrow produces:
The liquid part of bone marrow contains stem cells, or maturing blood cells. It also makes vitamins needed for cell production.
While a bone marrow biopsy tests the tissue part of your bone marrow, a separate procedure called a bone marrow aspiration tests the liquid portion. On the day of your procedure, your provider will likely perform a bone marrow aspiration immediately before the biopsy.
A bone marrow biopsy provides valuable information your provider can use to:
Advertisement
A bone marrow biopsy can also determine whether a donor is a good match for an allogeneic stem cell transplant. In some instances, a person with too few healthy blood cells may need new, healthy stem cells from a donor. For this to happen, the cells from the donor and recipient must match.
Your provider may perform a bone marrow biopsy to diagnose conditions involving too many or too few blood cells. Bone marrow biopsies may also be used to diagnose cancers affecting your blood or bone marrow.
Conditions include:
A bone marrow biopsy can also detect abnormalities in chromosomes and vitamin deficiencies, which can trigger your bone marrow to produce red blood cells that are misshapen or too large.
A provider specializing in blood disorders (hematologist) or cancer (oncologist) may perform your bone marrow biopsy. Nurses who are specially trained in this procedure also perform bone marrow biopsies.
Your provider will explain the procedure and instruct you on how to prepare. For instance, if you receive a sedative to help with the pain the day of the procedure, you may need to fast (no food or drink) the night before. You’ll need to arrange for someone to drive you home.
Your provider should have detailed information about your medical history and current medications. Tell them about:
Your provider will also need to know if you’re pregnant.
A bone marrow biopsy can occur in your healthcare provider’s office or hospital. The entire process lasts about 30 minutes. You’ll be awake during the procedure, but your provider will numb the biopsy site (local anesthesia) to keep you comfortable.
Advertisement
Before the procedure, you’ll change into a hospital gown. Your provider may give you a sedative to help you relax.
Your provider will send the sample to a lab, where it can be examined for signs of disease.
You may feel a sharp sting during the bone marrow aspiration, and you may feel brief, dull pain during the core biopsy part of the procedure. Unfortunately, bone can’t be numbed. You may feel pressure, pushing and pulling that may cause discomfort.
Advertisement
Talk to your provider about any concerns you may have about pain. In addition to numbing the biopsy site, they can provide medications to keep you more comfortable during your biopsy.
You’ll likely go home the same day of your procedure. If you received a sedative during the biopsy, you’ll need someone to drive you. Follow your healthcare provider’s instructions about caring for yourself as you recover.
They may advise you to:
Complications, like heavy bleeding and infection at the biopsy site, are rare. Usually, applying pressure to the site stops excess bleeding. Your provider may prescribe an antibiotic cream if you get an infection.
A specialist called a pathologist will analyze your bone marrow sample underneath a microscope. Your provider will review the pathologist’s findings and share next steps with you. Your provider may confirm a diagnosis, order more tests, or recommend or adjust treatments depending on your results.
Ask your provider what your results mean for you.
Call your healthcare provider if you experience signs of a complication, including:
Advertisement
A bone marrow biopsy may be necessary if you have signs of a blood disorder or another condition involving your bone marrow. Talk to your healthcare provider if you have specific questions about the procedure or concerns about the sensations you may feel during a biopsy. They can provide pain medication to keep you comfortable and relaxed. They can also talk you through each step of the procedure so you feel more informed and confident on your biopsy day.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
When you want expert blood disorder care, look no further than Cleveland Clinic. Our hematology experts offer personalized care and support.
