Continuous glucose monitoring (CGM) devices help you manage diabetes with fewer fingerstick checks. A sensor just under your skin measures your glucose levels 24 hours a day. A transmitter sends results to a wearable device or cell phone so you can track changes to your glucose level in real time. Learning how to use a CGM takes time, but it can help you more easily manage your health.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
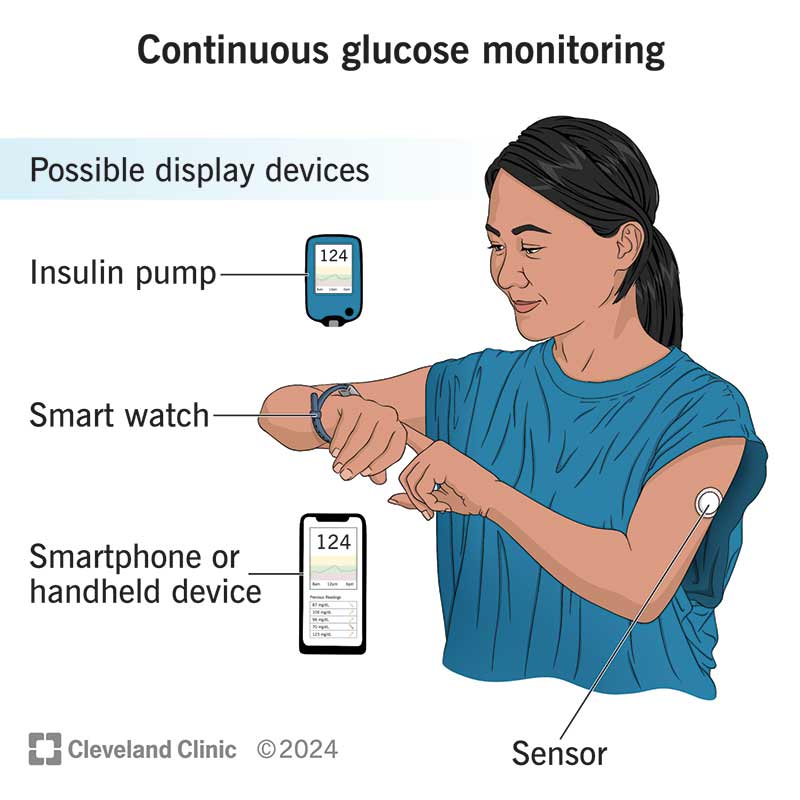
Image content: This image is available to view online.
View image online (https://my.clevelandclinic.org/-/scassets/images/org/health/articles/continuous-glucose-monitoring-cgm)
Continuous glucose monitoring (CGM) is wearable technology that tracks your glucose (sugar) levels over time. It measures the glucose level in the interstitial fluid just under your skin 24 hours a day while you’re wearing the device. People also call it a continuous glucose monitor (a CGM).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A CGM device is mainly a tool for people with diabetes. Managing diabetes involves managing your blood sugar levels. A CGM gives you real-time information on how your glucose levels are changing. This is especially important because several factors affect blood sugar levels — some of which you can’t predict.
There are several types of CGM devices on the market, and the technology is rapidly evolving. Some CGMs connect with insulin pumps to offer automated insulin delivery systems. Talk to your healthcare provider if you’re interested in learning more about CGMs.
Interstitial fluid is the fluid in the spaces around your cells. It comes from substances that leak out of your blood capillaries. One of these substances is glucose (sugar).
The sensor in a CGM goes just under your skin where this fluid is — not in a blood vessel. It measures the glucose in your interstitial fluid.
Glucose hits your bloodstream first and then leaks into your interstitial fluid. So, there’s a lag between your blood glucose level and interstitial glucose level. This means there may be a few minutes delay in your CGM sensor glucose readings compared with fingerstick (manual) blood glucose readings.
You can choose among a handful of CGM devices available today. Each works pretty much the same way. The main differences are in a device’s features, look and feel.
Advertisement
But all CGMs have three basic components:
In general, here’s how a CGM works:
You can download CGM data (trends and history) to a computer at any time. Some CGM systems will send data continuously. You can also share the information with your healthcare provider.
Advertisement
CGM devices are complex little machines. They do require some upfront time to understand their technical aspects.
For example, you’ll need to learn how to:
It takes time and patience to understand how a CGM device works. But you don’t have to do it alone. Once you’ve decided to get a CGM — and have a prescription for it — a qualified professional will help you learn how to use it safely. Your provider may recommend taking a diabetes education class or speaking one-on-one with a certified diabetes care and education specialist (CDCES).
Using a CGM should drastically decrease the number of times you need to do a fingerstick. But it’s still important to have a fingerstick meter and unexpired supplies on hand. If your CGM fails or falls off unexpectedly, you can use the fingerstick meter to check your glucose level until you can apply a new sensor.
Fingerstick checks can also act as a backup tool to confirm CGM results. Like all technology, CGMs can be inaccurate. If your CGM reading seems questionable, it’s always a good idea to do a fingerstick check to be sure. For example, a fingerstick check may give you peace of mind if your CGM device shows rising or falling numbers, but you feel OK. It can also provide answers if you don’t feel well, but the CGM says your glucose levels are in range.
Advertisement
You may also need to do fingerstick checks to calibrate (set up or adjust) a CGM device.
CGMs are mainly for people with diabetes. But healthcare providers may recommend CGMs for other conditions that impact glucose levels, like:
Talk to your healthcare provider if you think a CGM may benefit your health.
Using a CGM device can make it easier to manage diabetes. Several studies show that people with Type 1 and Type 2 diabetes who use a CGM have fewer episodes of low blood sugar and a lower A1C.
A CGM device can:
Advertisement
You can regularly check your blood glucose levels using a fingerstick with a blood glucose monitor. Many people do just that.
But fingerstick checks only measure blood glucose at one moment in time. It’s like reading one page of a book. Doing more fingerstick checks gives you more snapshots, which can offer clues to what’s happening with your blood sugar levels.
The vast majority of diabetes experts recommend the use of a CGM to manage diabetes. It provides significantly more information about blood sugar trends than fingerstick checks alone.
CGMs are extremely helpful tools. But they have some limitations. Like all technology, CGM systems can run into issues, be inaccurate or fail. Your CGM trainer will go over issues to look out for and how to troubleshoot them.
Certain medications and supplements can also affect the accuracy of certain CGM sensors, including:
These medications and supplements may make your CGM read your glucose level as higher or lower than it actually is. It’s important to check with the manufacturer of your CGM device to see what may affect the accuracy of it.
Some things that you may see as drawbacks of CGMs include:
Consider making an appointment with a CDCES if you’re facing any of these challenges. They can teach you tips and tricks to make a CGM easier to use.
Reach out to your diabetes healthcare provider if you have any questions about how to use a CGM device safely.
Very high or low blood sugar levels can be dangerous when left untreated for too long. In the most severe cases, this can lead to seizures, coma or even death. You can avoid these complications by keeping blood sugar levels in a healthy range. Call your provider if you have any symptoms you’re worried about.
Currently, there’s one CGM that’s available over the counter (OTC). That means you don’t need a healthcare provider or prescription to get it. Other CGM manufacturers are also in the process of making OTC CGMs.
OTC CGMs may not be suitable for people who use insulin to manage diabetes or who experience significant low blood sugar episodes. Make sure you understand the capabilities and limitations of OTC CGMs before using them.
Managing diabetes can feel like trying to hit the bullseye of a moving target — it’s very difficult to begin with. With just fingerstick checks, it’s as if you’re blindfolded until the second before you’re able to throw the dart. With a CGM, it’s as if you can watch the target moving — its direction and how fast or slow it’s moving — before you throw the dart. CGMs are a very powerful tool to have in your diabetes management toolbelt. Talk to your healthcare provider if you want to learn more about using one.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about the Health Library and our editorial process.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Cleveland Clinic’s health articles are based on evidence-backed information and review by medical professionals to ensure accuracy, reliability and up-to-date clinical standards.
Whether you’ve been living with diabetes for years or you’re newly diagnosed, you want experts you can trust. Our team at Cleveland Clinic is here to help.
